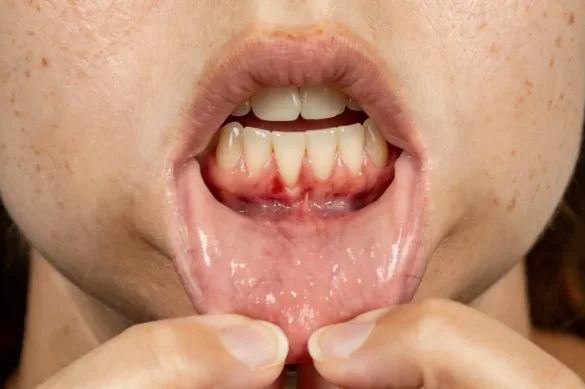
periodontal disease, commonly known as gum disease, is one of the most prevalent oral health problems worldwide. Many people may not understand exactly why it is classified as a disease. Learning about its characteristics, causes, and effects can help clarify why periodontal disease deserves serious attention and medical treatment.
What Is periodontal disease?
periodontal disease refers to a group of conditions that affect the tissues surrounding the teeth. The periodontium includes the gums (gingiva), bone, and connective tissue that anchor teeth in place. The most advanced and critical form of gum disease is called periodontitis. This condition goes beyond simple irritation or redness; it is a complex inflammatory disease process that can destroy the structures needed to retain teeth.
How periodontal disease Develops
periodontal disease usually begins as gingivitis, which is the mildest form of gum disease. gingivitis is characterized by red, swollen gums that may bleed during brushing or flossing. gingivitis is caused by an accumulation of plaque, a sticky film made primarily of bacteria, on the teeth. If plaque is not removed promptly, it can harden into tartar, which cannot be cleaned away with regular brushing and flossing.
As tartar and plaque remain on the teeth, bacteria in these substances continue to irritate the gums and cause an immune response. Over time, this inflammation becomes long-standing and can turn into periodontitis. The gums start to pull away from the teeth, forming pockets where even more bacteria and debris collect. Eventually, this process leads to the destruction of both the soft tissue and bone that support the teeth.
Why Is periodontal disease Classified as a Disease?
Meets Medical Criteria for a Disease
For a condition to be classified as a disease, it should demonstrate identifiable signs and symptoms, a clear cause, and predictable progression if left untreated. periodontal disease meets all of these criteria.
Inflammatory Process
periodontal disease is primarily an inflammatory process. The body’s immune system reacts to bacteria in the plaque. Over time, this response damages the very tissues the immune system is trying to protect. This self-destructive cycle is a hallmark of many diseases, especially those involving chronic inflammation.
Distinct signs and symptoms
Symptoms of periodontal disease distinguish it from simple gum irritation. These signs include swollen or puffy gums, persistent bad breath, gums that bleed easily, pain while chewing, receding gums, loose teeth, and, eventually, tooth loss. In advanced cases, pus may form between teeth and gums, and new gaps may appear between teeth. These symptoms are clear indications of a pathologic process, not just a minor or temporary annoyance.
Defined Etiology and risk factors
periodontal disease is not random. It has well-defined causes and recognized risk factors. The main cause is bacterial plaque, but risk is increased by poor oral hygiene, smoking or vaping, genetic predisposition, diabetes, hormonal changes (such as pregnancy or menopause), certain medications, and illnesses that weaken the immune system. These factors show that periodontal disease follows the established models used in medicine to define diseases.
Potential for Disease progression
Without intervention, periodontal disease worsens over time. It may start as mild gingivitis and progress all the way to severe periodontitis. Left unchecked, it leads to both tissue and bone loss. This clear trajectory is another reason why gum disease is classified as a true disease.
The Impact of periodontal disease on General Health
A disease does not only affect one part of the body; often, it has implications beyond its primary site. periodontal disease can impact overall health in several significant ways.
Risk of tooth loss
As the supporting bone deteriorates, teeth can become loose and may eventually fall out on their own or require extraction. Losing teeth affects eating, speaking, and self-confidence.
Role in systemic illnesses
Studies increasingly link periodontal disease to various systemic conditions. Bacteria from infected gums can enter the bloodstream, potentially contributing to or worsening conditions such as heart disease, diabetes, respiratory disease, and complications in pregnancy. chronic inflammation from the disease has also been implicated in conditions like rheumatoid arthritis.
Why prevention and Awareness Are Critical
Early stages of gum disease are often painless, and symptoms can be mild. This allows the disease to progress quietly until significant damage occurs. Awareness, prevention, and early detection are critical.
How to Prevent periodontal disease
Good oral hygiene is the primary defense against periodontal disease. Regular brushing (at least twice a day for two minutes each time), flossing once a day, and routine professional cleanings are essential. A healthy diet and lifestyle, including not smoking or using tobacco, also reduce risk.
Who Is at Higher Risk?
People with certain illnesses, those who smoke, or those with a family history of gum disease should be extra vigilant. They may need more frequent dental checkups and professional cleanings than the average person.
When to Seek Help
Seeing a dentist regularly is the cornerstone of prevention. If you notice red, swollen, or bleeding gums, persistent bad breath, pain when chewing, loose teeth, or new gaps between your teeth, make a dental appointment as soon as possible. Early intervention can reverse damage in the early stages and prevent progression to more serious disease.
Conclusion
periodontal disease is much more than a minor inconvenience or the result of poor oral hygiene. It is a true disease that features classic signs and symptoms, defined causes, and the possibility of progression to severe health problems if left unmanaged. The inflammatory and destructive nature of periodontal disease, and its connections to other health issues, make it a significant medical concern. Understanding why periodontal disease is classified as a disease empowers people to take it seriously, seek timely care, and protect both their oral and overall health.
Frequently Asked Questions
What are the early signs of periodontal disease?
Early signs include swollen, red, or bleeding gums—especially during brushing or flossing—and persistent bad breath.
Can periodontal disease be cured?
Early gum disease (gingivitis) can be reversed with good oral hygiene and professional cleaning. Advanced periodontitis may require more intensive treatments, and damage might be permanent.
Is periodontal disease contagious?
periodontal disease is caused by bacteria, which can be transmitted through saliva, but the disease itself is more about individual risk factors and immune response.
How often should I see a dentist to prevent periodontal disease?
Most people should see a dentist every six to twelve months. Those with higher risk factors should consult their dentist for an appropriate schedule.
Does treating periodontal disease improve overall health?
Yes. Addressing gum infections can lower inflammation in the body and may help improve or prevent complications with heart disease, diabetes, and other conditions.