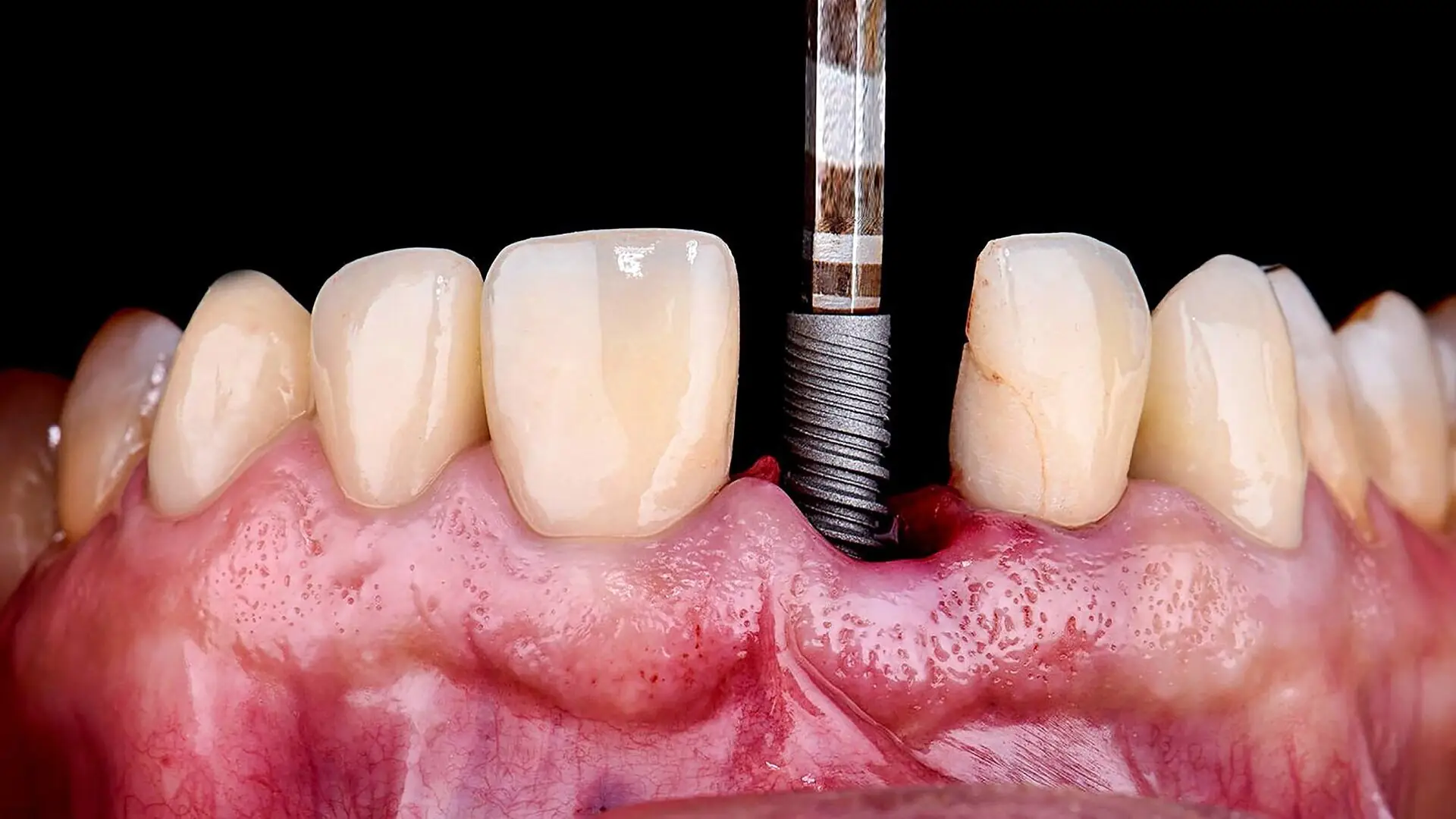
Implant dentistry has undergone a revolutionary transformation with the advent of digital workflows. These advancements have significantly improved the treatment of patients with periodontal disease and terminal dentition. One of the greatest challenges in full-arch rehabilitation has always been achieving predictability—ensuring consistent and reliable clinical outcomes. This involves careful planning and execution to optimise efficiency, reduce treatment time and create a more comfortable experience for the patient.
The tides have shifted in full-arch restorations, moving away from the traditional Misch classification FP-3 approach, which required extensive bone resection to accommodate a fixed hybrid prosthesis with a titanium bar. Instead, the focus is now on preserving the patient’s existing bone and soft tissue. Today, patients with terminal dentition can receive restorations that not only provide them with functional teeth but also maintain their natural soft-tissue architecture. The modern approach leans towards FP-1 restorations, enabling patients to achieve a natural smile that blends with their own gingival tissue.
Digital workflows have also brought greater precision and reduced stress for both dentists and dental technicians. The process eliminates many of the complexities associated with analogue impressions, such as splinting impression copings and repeating steps if passive fit checks fail. This was the final analogue step that dentists had to perform, even in the digital workflows we rely on today. Now with SmartFlag scan bodies (Apollo Implant Components), this step has been eliminated, allowing us to transition fully into the digital realm for complex full-arch restorations. By embracing digital methods, we achieve higher accuracy and efficiency, ultimately enhancing the patient experience.
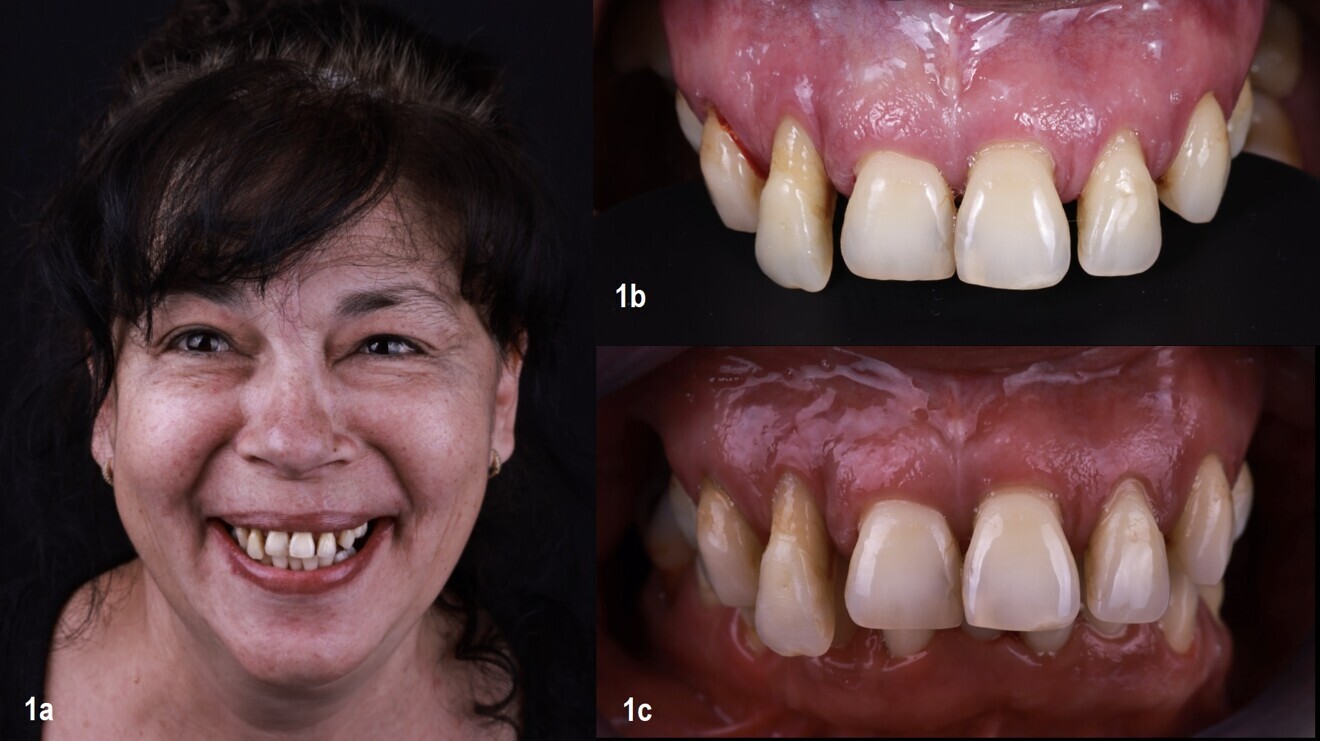
Figs. 1a–c: Initial situation.
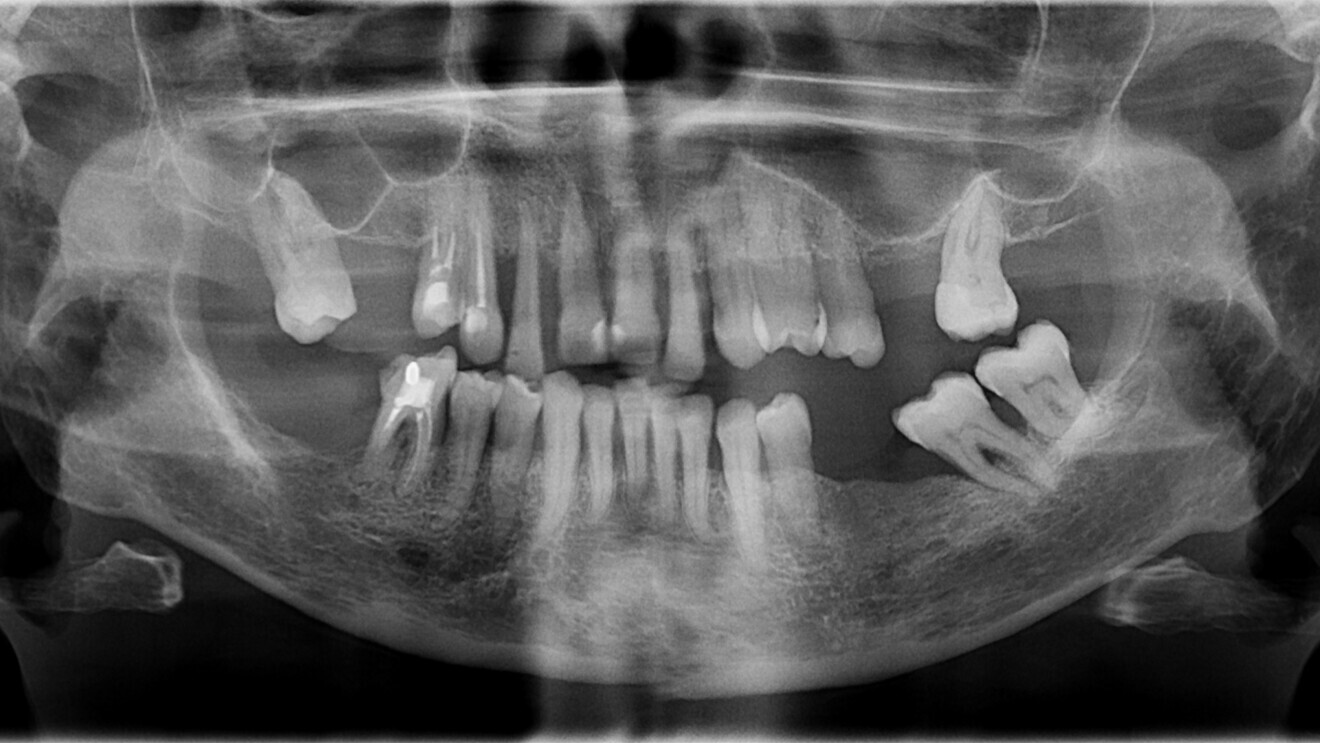
Fig. 2: Panoramic radiograph before treatment.
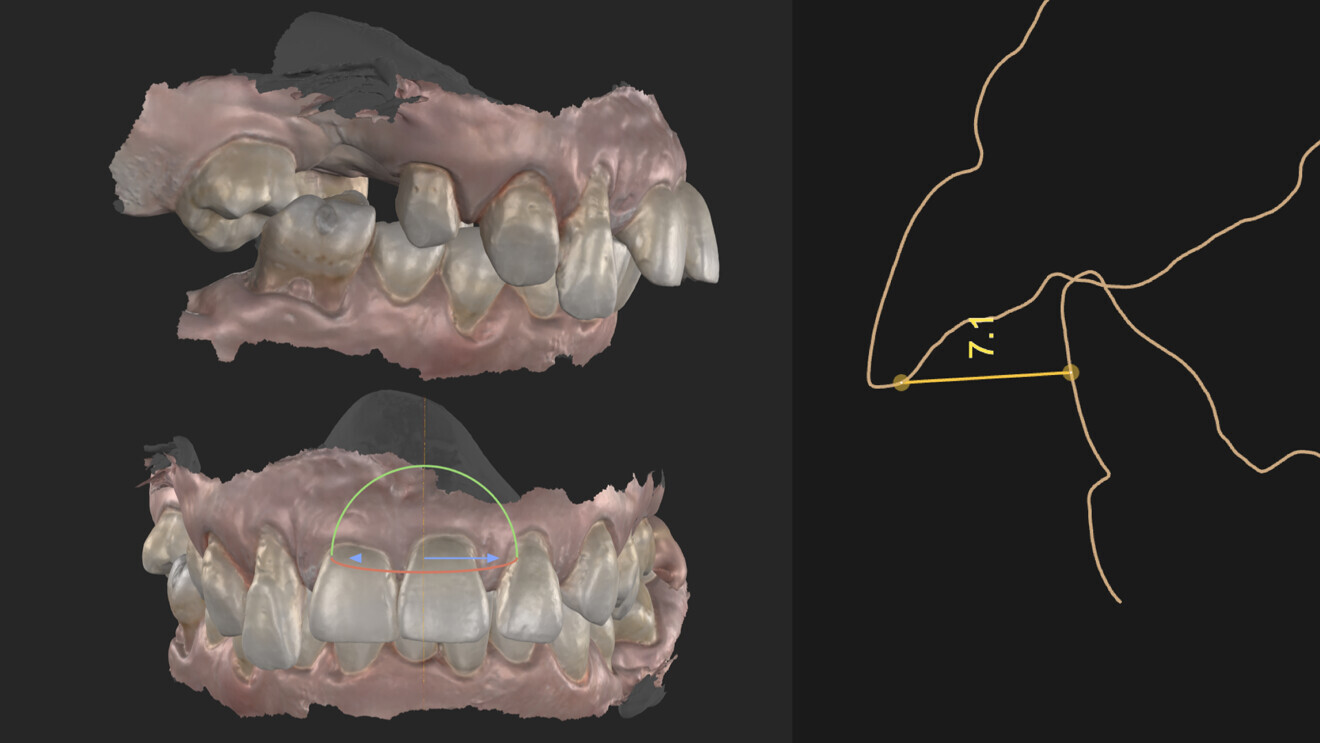
Fig. 3: Overjet and overbite.
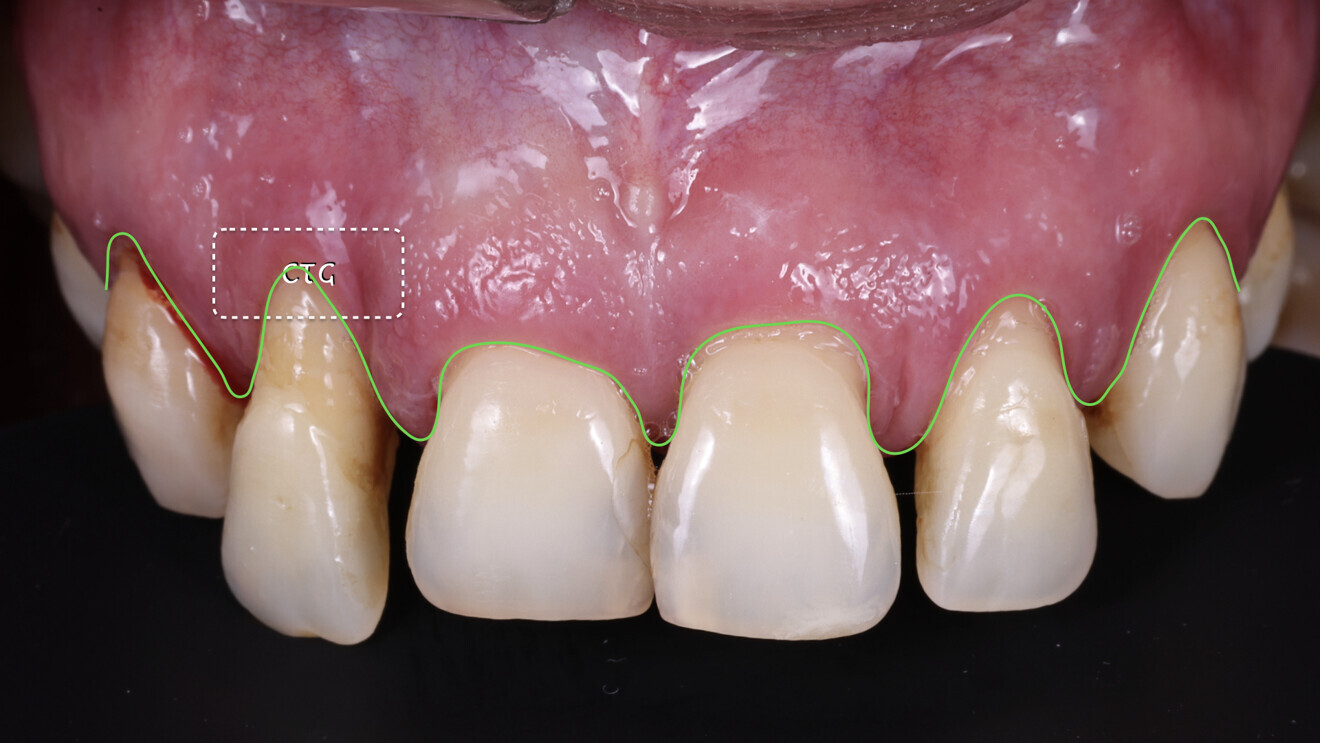
Fig. 4: Soft-tissue profile. We observed an excess of tissue overall except in the area of tooth #12, where a connective tissue graft (CTG) would be needed.
Case presentation
A 52-year-old female patient presented to our office seeking treatment for her periodontal disease. Her primary concerns were functional, in that she had difficulty chewing properly, but she also desired a more confident smile (Fig. 1).
After a thorough anamnesis, clinical evaluation and radiographic examination (Fig. 2), the patient was diagnosed with Stage IV, Grade C periodontitis. After a complete periodontal cleaning and full-mouth disinfection, it became evident that none of the teeth in her upper jaw were salvageable.
We presented the patient with three treatment options:
- Maintain her existing maxillary teeth: While this approach could prolong the life of her teeth, it would not address her primary concerns regarding functionality and aesthetics.
- Extract all her maxillary teeth and transition to a removable prosthesis: This would eliminate the bacterial load and compromised teeth. However, this option might not have provided the confidence or social integration the patient desired.
- Extract all her maxillary teeth and replace them with implants: This option would aim to preserve her existing gingival architecture, restore proper function and deliver an aesthetically pleasing result. In our professional opinion, this was the most reasonable and effective solution for the patient.
Diagnostic findings
From analysis of the patient’s documentation, it was clear that loss of bony support had caused her teeth to migrate and tilt forwards such that they extended over the lower lip, resulting in excessive overjet. Additionally, there was a noticeable deviation of the midline, which had shifted towards the right. The incisal edges no longer followed the natural contour of her lower lip during a smile.
From an occlusal perspective, the patient exhibited both an excessive overjet and overbite (Fig. 3). However, her gingival architecture remained largely intact. Despite the presence of deep, untreatable periodontal pockets, there was minimal recession, thanks to her thick periodontal biotype (Fig. 4). This offered us an advantage. With careful planning and proper design, we were confident that we could preserve and slightly modify her gingival tissue to meet her aesthetic goals.
Treatment planning
Restoration design
We begin with facial analysis and use planning software to select the appropriate tooth forms that complement the patient’s facial structure and determine the optimal apico-coronal tooth positioning. This step is particularly beneficial when the software allows us to modify tooth forms in relation to the patient’s soft-tissue contours, including papillary height, ideal gingival zeniths and other critical aesthetic parameters (Fig. 5). For this patient, as we aimed to achieve high papillae and have an excess of soft tissue to manipulate, we opted for trapezoidal tooth forms or potentially triangular forms rather than square ones. Once the desired tooth forms are selected, they are exported to a 3D CAD software program for precise positioning in the buccolingual dimension.
For effective 3D planning, having a combined extraction model is essential. This provides the dental technician with clear reference points for creating custom support that follows the emergence profile of each individual tooth (Figs. 6 & 7).
In this specific case, we strategically positioned the design palatally and more coronally. This compensated for the existing occlusal disharmonies while also shaping the soft tissue for prosthetically guided healing of the extraction sites. By integrating these adjustments, we could harmonise the patient’s bite and smile, achieving both function and aesthetics (Figs. 8–10).