Delivery of dental care falls into two categories: single provider care (uni-disciplinary) and collaborative care. The structure of a practice—that is, solo practitioner, private multi-practitioner or corporate dentistry model (dental support organisation or orthodontic support organisation)—and a provider’s overall viewpoint on the delivery of dental care influence adoption of one versus the other approach. Multidisciplinary and interdisciplinary care are two forms of collaborative delivery of dental care.
In the multidisciplinary model, the patient will be treated by multiple providers specialised or focused on certain subdomains of dentistry. The overall treatment plan and goals are not coordinated, and the delivery of care is often in a tandem fashion; for example, the orthodontist optimises space for an implant and then passes the patient to the periodontist to place the implant, and the general dentist delivers the implant-supported restoration. The treatment outcome in multidisciplinary care can be successful, especially if all providers think similarly and have an overlapping treatment philosophy. Nonetheless, the likelihood of complications and substandard treatment outcomes is also high, primarily owing to a lack of communication.
Collaborative dentistry ideally ought to be delivered in an interdisciplinary model. Specifically, various providers with an array of expertise collaboratively develop a treatment plan, involving the patient in this process. The delivery of the interdisciplinary treatment plan is sequenced and timed with milestones defined for each provider. The team collaborates through the delivery of care and adjusts the plan as needed, based on a common vision. An example of such an interdisciplinary team is the Northwest Network for Dental Excellence, a study club developed by Dr Ralph O’Connor.
Various advantages of interdisciplinary collaborative dentistry have been highlighted.1 These benefits can be divided into patient-related improvement of care and provider-focused professional development. Examples of patient-related advantages are greater quality of care, decreased potential error or duplication of services, enhanced cost-effectiveness and treatment efficiency, and an overall elevated patient and caregiver experience. For providers, delivering care as part of an interdisciplinary team allows them to advance professionally. These collaborations have a compounding effect and create more collaborations. Furthermore, having a group with whom to discuss the daily ups and downs of practising dentistry is an indirect benefit of delivering dental care according to an interdisciplinary approach.
To develop an interdisciplinary team, one should identify potential members that excel in the following five characteristics: collaborative mindset, commitment to learning, supportive personality, time management skills and trustworthiness.2 Specifically, one should prioritise collective goals over individual achievements and understand that collaboration leads to better patient care outcomes. The interdisciplinary team members ought to possess deep expertise in their respective fields, raising the overall standard of care. An ideal member of an interdisciplinary team encourages and supports other team members while maintaining focus on treatment objectives and the overarching vision. High-level time management skills to enable regular participation in group discussions and meetings is essential, and an interdisciplinary team member ought to share opinions openly and honestly, fostering a culture of transparency and non-judgement. Individuals with inflated egos are likely to weaken the team.
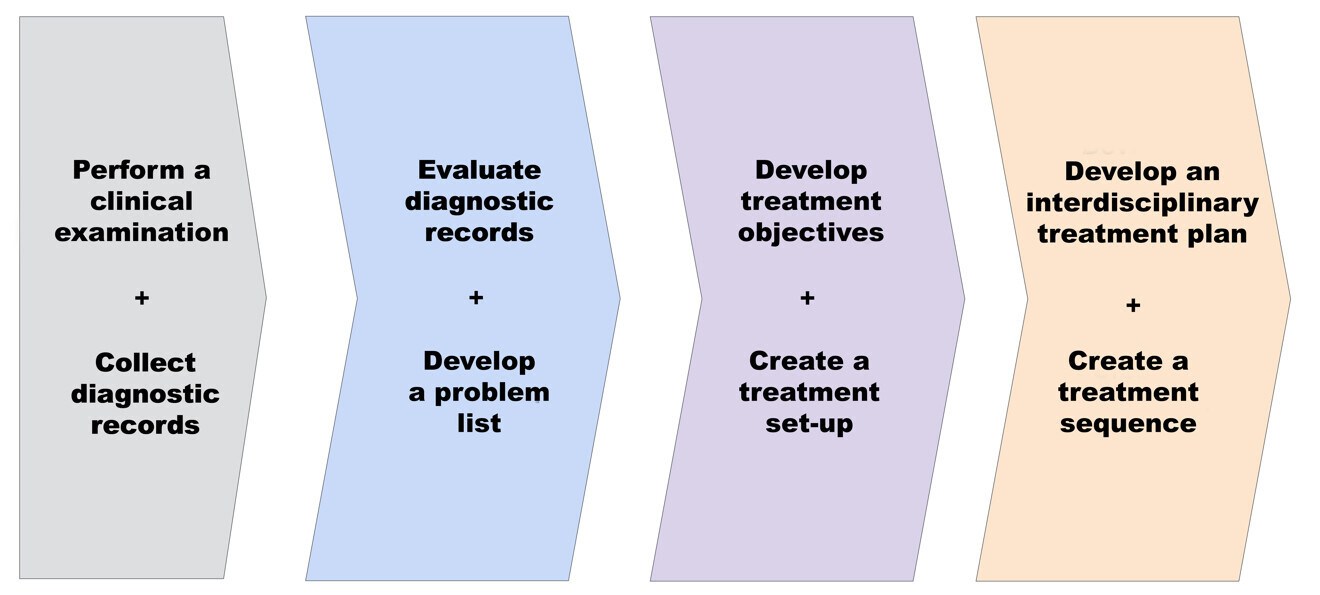
Fig. 1: Four-step framework for achieving predictability and systematically developing and delivering interdisciplinary care.
Obstacles to delivering interdisciplinary dental care
Despite the significant advantages of delivering dental care through a collaborative interdisciplinary approach, most dental care is delivered according to uni-disciplinary or multidisciplinary approaches. Anecdotally, when dental professionals are asked about their reluctance to adopt an interdisciplinary approach to dental care, their responses generally fall into two categories: the complexity of delivering interdisciplinary care—essentially not knowing where to start—and the time-consuming nature of communication within an interdisciplinary team.
To address these challenges, a systematic framework—essentially an operating system for interdisciplinary care—is necessary. The core advantages of this approach are the consistency and standardisation of best practices, as well as the optimisation of treatment efficiency and resource utilisation.
A four-step framework for developing an interdisciplinary treatment plan
To overcome complex issues, a set of guidelines is essential for tackling the problem consistently.³ These guidelines help in formulating a clear plan and resolving each issue by breaking it down into simpler, manageable components.
An interdisciplinary treatment planning framework offers a comprehensive structure that encompasses various methodologies, techniques and processes. Essentially, it acts as an operating system guiding practitioners through each step—from collecting information and analysing records to developing problem lists and treatment objectives (Fig. 1). Finally, it aids in formulating an interdisciplinary plan and determining the sequence of treatment. This framework simplifies the process and helps practitioners develop muscle memory as they practise delivering interdisciplinary dental care.
The first step of interdisciplinary treatment planning begins with a clinical examination to collect both subjective and objective information. This includes acquiring diagnostic records such as 3D dental models, radiographs, questionnaires, and intra-oral and extra-oral photographs. Subjective information encompasses the patient’s medical and dental history, as well as social history (e.g. family structure and dynamics, distance to commute for care and level of interest and engagement). At this stage, it is also vital to assess the patient’s perceptions and expectations and conduct an objective assessment.
The clinical examination encompasses both extra-oral and intra-oral assessments of the patient. These assessments should take into account all three planes of space: anterior–posterior, transverse and vertical. During the clinical examination, it is essential to document facial and skeletal patterns, as well as collect smile arc records. Additionally, a thorough periodontal evaluation, an assessment of the patient’s restorative status (including aesthetic and functional occlusion) and a temporomandibular joint evaluation should be performed. The periodontal examination should include an assessment of gingival type, bone topography, oral hygiene, gingival aesthetics (including display, colour, contour and papillary form), probing depths, recession and furcation involvement—including horizontal bone loss. Restorative assessments should cover all aspects of the occlusion: contacts, guidance, mobility, functional mobility, tooth position (including rotation and tipping) and any existing restorative work or needs, such as caries. This comprehensive approach ensures a detailed and accurate evaluation of the patient’s overall oral health.
The second step involves evaluating the diagnostic records and clinical examination information to develop a comprehensive problem list. This evaluation should involve analysis of all diagnostic records, such as 3D scans and radiographs, video records (e.g. smile analysis), 2D photographs, questionnaires (e.g. nutrition or sleep evaluations) and reports (e.g. sleep reports and physician’s letters). To ensure thoroughness and consistency, it is advisable to use a standardised template for this step.⁴ This approach helps to avoid overlooking information and helps to maintain consistency over time, facilitating a more accurate and reliable development of the problem list.
The third step involves using the problem list to establish treatment objectives that aim to completely or partially address the identified issues. As part of this step, a treatment simulation should be conducted to evaluate the feasibility of the proposed treatment objectives. For example, one might consider how much mandibular anterior intrusion is required to level the mandibular arch completely and whether this level of intrusion is biologically achievable and predictable, or one might determine how much space is necessary to restore severely worn maxillary anterior teeth. By carefully examining these factors through treatment simulations, clinicians can ensure that the treatment objectives are realistic and achievable.
The fourth step entails formulating the treatment plan and creating a treatment sequence with clear assignment of treatment objectives to be addressed by the respective members of the interdisciplinary team. When developing a treatment plan, one ought to clearly define the differences between normal and ideal conditions, appreciate dental and skeletal compensations, and recognise the limitations of all procedures and techniques in an interdisciplinary treatment plan.⁵ When finalising the treatment plan, the financial aspect of care must be considered. A practical and predictably successful interdisciplinary treatment plan can be developed around a compromised treatment, for example leaving an adult patient in posterior crossbite with a functional occlusion.
Following these four steps helps providers to develop a clear and structured approach to interdisciplinary treatment, regardless of the complexity of care. For more detailed information on this process, please refer to Nelson et al.⁴
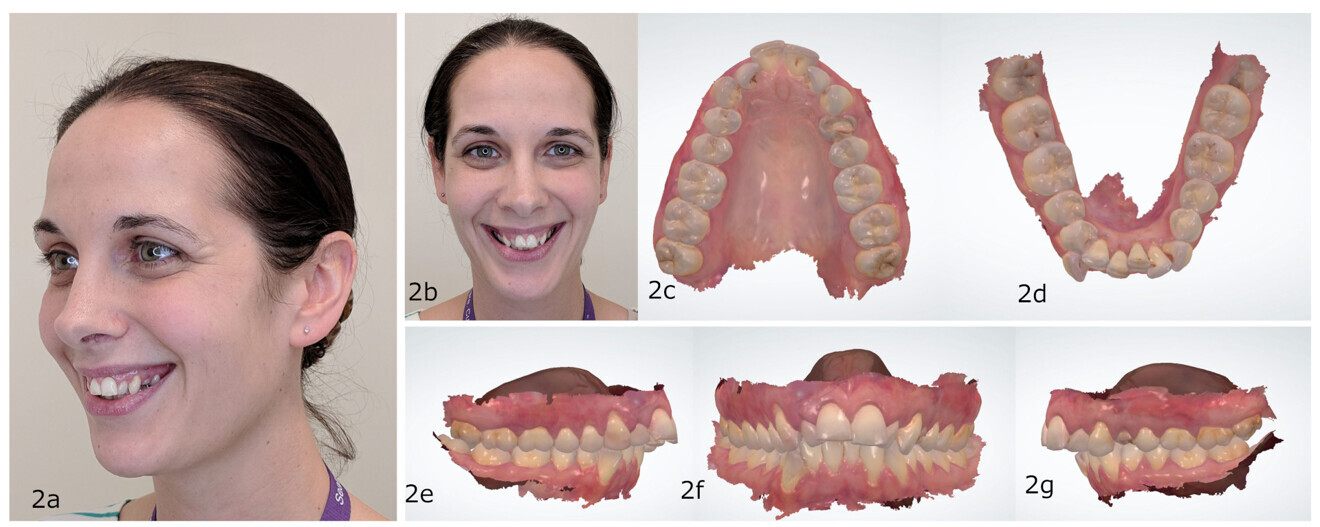
Figs. 2a–g: Illustration of the use of digital treatment simulation to assess the feasibility of extracting the maxillary first premolars and ultimately restoring the maxillary anterior teeth with veneers.
Leveraging treatment simulation to deliver a successful interdisciplinary treatment
Traditionally, treatment simulations—also known as set-ups—are performed using physical dental models mounted on articulators. This approach remains useful, particularly for treatments that require accurate replication of occlusion and facial records using an articulator. However, digital technology has significantly enhanced the process of simulating interdisciplinary treatments (Fig. 2). Historically, the cost and time involved have been major barriers to the widespread use of treatment simulations.⁶ Software programs have alleviated these issues by reducing or even eliminating costs. Some software, such as ClinCheck (Align Technology), is operated by third-party technicians and often provided at no additional cost. Additionally, provider time is minimised, as laboratory technicians create the simulations based on the provider’s recommendations.
Beyond cost reduction and time-savings, the advantages of digital treatment simulation include the precise identification of tooth movement and the ease of sharing simulations with the treatment team and patients. A recent thesis revealed that orthodontists found treatment simulations for patients with varying degrees of treatment needs to be useful, even though they do not routinely use them in their practices.⁶
Evaluating multiple digital treatment simulations can aid in developing realistic treatment objectives. These simulations should be collaboratively planned after creating the problem list and drafting the treatment objectives. Examples of matters to cover in an interdisciplinary treatment simulation include defining a healthy range of tooth movement with orthodontic care, estimating the response of periodontal tissue to planned tooth movements, determining the requirements of alveolar bone morphology (width and height) for dental implant placement and marking the position of gingival margins in the aesthetic zone.
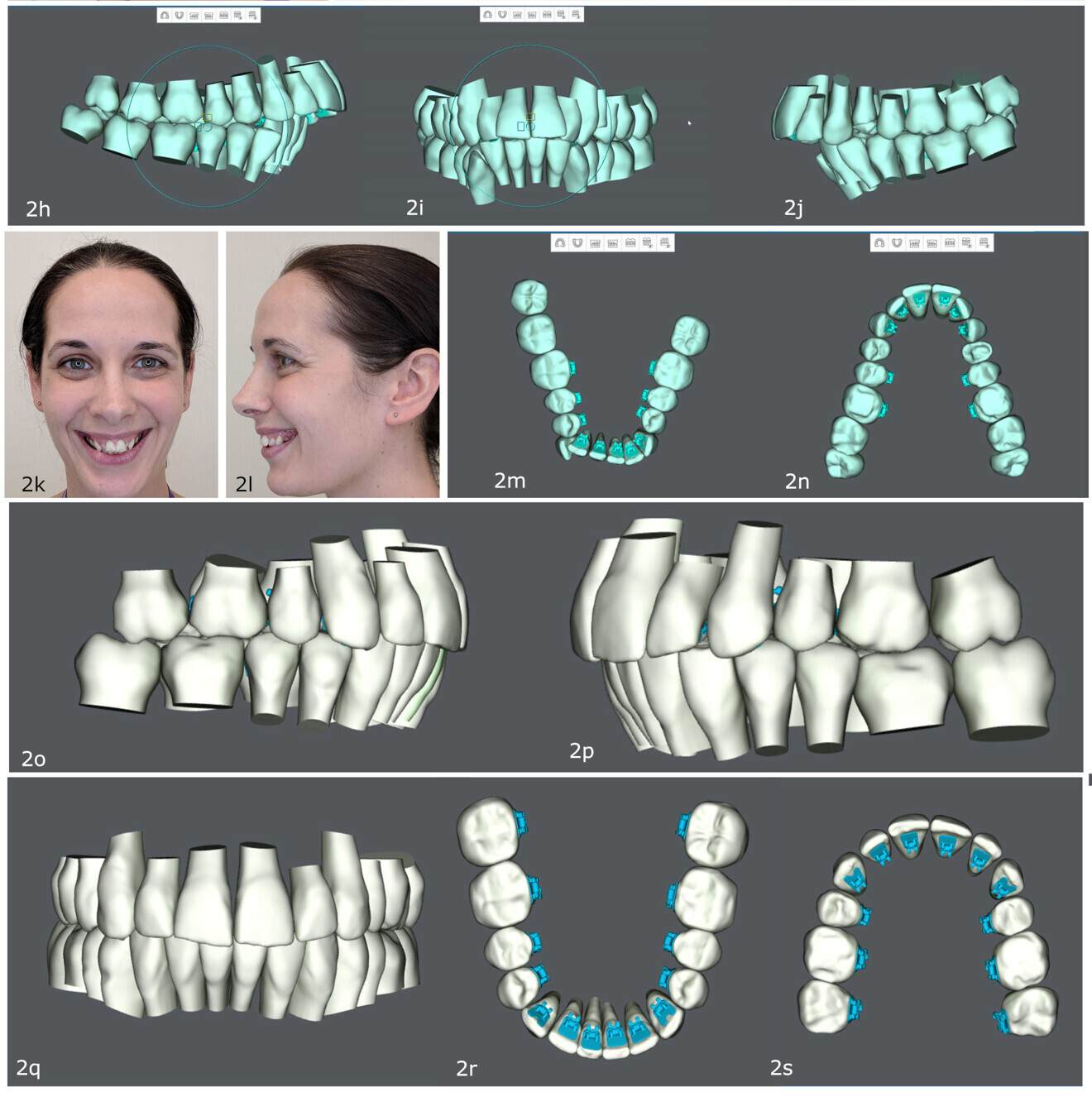
Figs. 2h–s: Digital treatment simulation in SureSmile (Dentsply Sirona) of treatment to be delivered through robotically bent lingual fixed appliances.
Enhancing interdisciplinary care with 3D printing
Dental 3D printing (additive manufacturing) has significantly improved over the last decade.⁷ As mentioned, developing treatment simulations is a key strategy for delivering successful interdisciplinary care. To further enhance the benefits of treatment simulations, the interdisciplinary team can integrate 3D printing into the process (Fig. 3).
Treatment simulations can be printed in various formats, including dental models, temporary restorations and surgical guides. These printed objects help solidify the treatment plan and bring the interdisciplinary team’s vision to life. The cost of these solutions has been decreasing owing to advancements in resin materials and affordable design services. I believe that 3D printing strengthens the third step of the interdisciplinary treatment planning framework.



