Presentation
Population
- Patients with previous extensive restorations (e.g., amalgam or resin restorations, crowns), trauma or recurrent caries with pulp exposure
- Medically-compromised patients
Signs
- Swelling (sometimes)
- Sinus tract (sometimes)
- Large periapical lesions (sometimes)
Symptoms
- Pain severity may vary
- Continuous flow of pus or serous-like fluid
- Bad taste in mouth (drainage from sinus tract)
Investigation
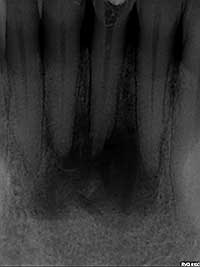 Fig. 1: Pre-treatment radiograph: large periapical radiolucency associated with two necrotic teeth.
Fig. 1: Pre-treatment radiograph: large periapical radiolucency associated with two necrotic teeth.
- Thoroughly assess the patient’s medical history: diabetes mellitus, bleeding disorders, history of radiation therapy and trauma.
- Perform a complete extraoral and intraoral examination:
- Examine for sinus tract inside or outside the oral cavity. If present, trace radiographically.
- Examine for swelling and periodontal pocketing.
- Examine teeth for caries, broken down restorations, crowns with open margins or recurrent caries.
- Perform pulp tests (hot, cold and electric) on the tooth in question and surrounding teeth to ensure they are not contributing to the problem.
- Perform a radiographic examination:
- periapical radiographs to check for periapical (PA) pathology and periodontal problems (Fig. 1)
- bitewing radiographs to check for dental caries
- Perform a radiographic examination to investigate:
- recurrent caries
- pulp exposures
- widened periodontal ligaments
- external and internal resorption
- calcifications
- length accuracy, perforations, strip perforations, or possible additional canals after the initiation of treatment
- pathology in the area around the teeth or in the maxillary sinus
Diagnosis
Based on the clinical and radiographic examinations and the patient’s medical history, a diagnosis of necrotic tooth with unstoppable drainage is determined.
Treatment
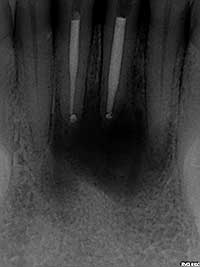 Fig. 2: Post-treatment radiograph: treatment involved both non-surgical and surgical endodontic procedures to resolve the unstoppable drainage.
Fig. 2: Post-treatment radiograph: treatment involved both non-surgical and surgical endodontic procedures to resolve the unstoppable drainage.
If the patient presents with a fluctuant swelling, consider doing an incision and draining prior to initiating treatment. Then begin instrumentation.
- Perform a more thorough cleaning and shaping of the canal spaces to ensure that all necrotic materials have been removed.
- Verify length determination (apex locator and radiographs) to ensure that over-instrumentation did not occur. Special care should be taken near the maxillary sinus, since over-instrumentation can lead to persistent drainage.
- If a strip perforation or perforation is noted, repair immediately with MTA or equivalent material. If unable to perform this procedure, refer the patient to an endodontist.
- Irrigate with NaOCl and leave in the canals and chamber for 10–15 minutes. Dry and place Ca(OH)2 in the canals and close, if drainage stops.
- Use negative pressure irrigation, if available.
- If all else fails, leave the tooth open, reappoint the next day, lightly instrument, irrigate and dry, and close the canal.
- In cases where there is a large PA radiolucency associated with a necrotic tooth and the drainage continues, both conservative and surgical endodontic treatments may be required (Fig. 2). Refer to an endodontist if uncomfortable dealing with this situation.
THE AUTHOR
|
Dr. Jafine is on staff at the Peel Memorial Hospital in Brampton, Ontario. He also maintains a private practice in endodontics and microsurgical procedures in Scarborough and Bramalea, Ontario. Dr. Jafine was a clinical instructor at the University of Toronto faculty of dentistry for 15 year in both the undergraduate and graduate programs. |
|
Correspondence to: Dr. Jafine, Partners in Endodontics, 709-2075 Kennedy Rd, Scarborough, ON M1T 3V3. Email: [email protected]
The author has no declared financial interests.
This article has been peer reviewed.
Suggested Resources
- Imura N, Zuolo ML. Factors associated with endodontic flare-ups: a prospective study. Int Endod J. 1995;28(5):261-5.
- Morse DR, Koren LZ, Esposito JV, Goldberg JM, Belott RM, Sinai IH, et al. Asymptomatic teeth with necrotic pulps and associated periapical radiolucencies: relationship of flare-ups to endodontic instrumentation, antibiotic usage and stress in three separate practices at three different time periods. Int J Psychosom. 1986;33(1):5-87.
- Walton R, Fouad A. Endodontic interappointment flare-ups: a prospective study of incidence and related factors. J Endod. 1992;18(4):172-7.
- Harrington GW, Natkin E. Midtreatment flare-ups. Dent Clin North Am. 1992;36(2):409-23.
- Harrison JW, Gaumgartner JC, Svec TA. Incidence of pain associated with clinical factors during and after root canal therapy. Part 1. Interappointment pain. J Endod. 1983;9:384.
- Fabricius L, Dahlén G, Sundqvist G, Happonen RP, Möller AJ. Influence of residual bacteria on periapical tissue healing after chemomechanical treatment and root filling of experimentally infected monkey teeth. Eur J Oral Sci. 2006;11(4):278-85.
- Seltzer S, Bender IB, Ziontz M. The dynamics of pulp inflammation: correlations between diagnostic data and actual histologic findings in the pulp. Oral Surg Oral Med Oral Pathol. 1963;16:846-71.
- Tsesis I, Faivishevsky V, Fuss Z, Zukerman O. Flare-ups after endodontic treatment: a meta-analysis of literature. J Endod. 2008;34(10):1177-81.
- Torabinejad M, Kettering JD, McGraw JC, Cummings RR, Dwyer TG, Tobias TS. Factors associated with endodontic interappointment emergencies of teeth with necrotic pulps. J Endod. 1988;14(5):261-6.


