Minimally invasive methods of oral cancer detection can aid in early diagnosis and prompt treatment planning. Here are two methods which are minimal or non-invasive methods of oral cancer detection.
Chemiluminescent Illumination – A minimally invasive method
- The term “chemiluminescence” refers to the emission of light from a chemical reaction.
- A nontoxic blue-white chemiluminescent light is shone into mouth and tissue reflectance is observed.
- Improve the identification of mucosal abnormalities with respect to the use of normal incandescent light.
- Devices working based on this principle: Vizilite, Microlux DL unit
Vizilite
- Is an oral lesion identification and marking system
- Used as an adjunct to the conventional head and neck examination
- Comprised of a chemiluminescent light source (ViziLite) to improve the identification of lesions and a blue phenothiazine dye to mark those lesions identified by ViziLite
- Has outer flexible plastic capsule containing aspirin or acetyl salicylic acid- inner fragile glass vial containing hydrogen peroxide
- These chemicals react to produce light of blue-white color (430-580 nm) which lasts for 10 min
- Normal epithelium will absorb light and appear dark
- Hyperkeratinized or dysplastic lesions appear white
Contraindications :
- For those who might have difficulties understanding instructions and for who have physical impairments.
Microlux DL
- Painless, non-invasive test, takes less than three minutes
- Acetic acid dehydrates the cytoplasm of acetowhite lesions and the lesion’s refractive properties are changed
- The irregular cells take on a whitish hue which contrasts with surrounding tissue, helping to identify abnormalities which require further testing
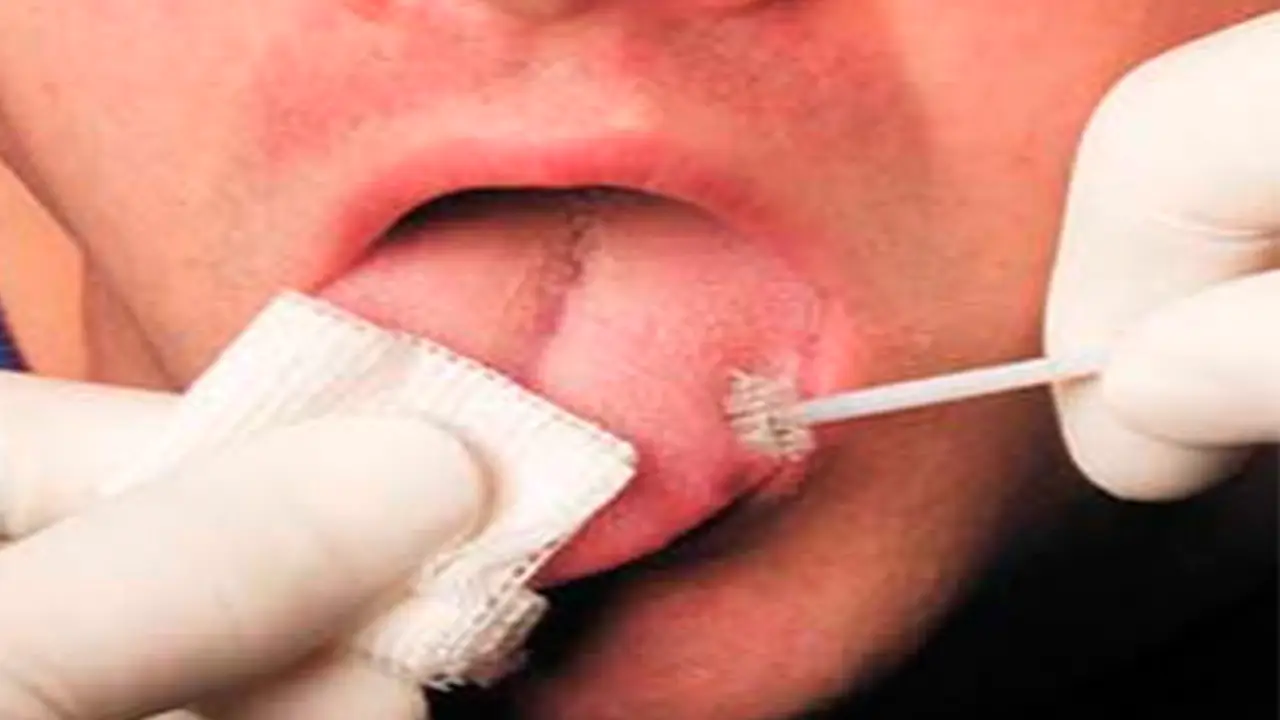
Oral Brush Biopsy
- Introduced in 1999
- It utilizes a stiff brush to collect the sample cells from the basal layer cells non invasively and assess the dysplasia by computer assisted neural network.
- Is a rapidly conducted chair side procedure
- Results in minimal bleeding, requires no topical or local anesthetic, and results in a collection of a complete transepithelial tissue sample
- The cutting edge of the brush is placed against the lesion and while maintaining firm pressure, rotated in a clockwise fashion
- The brush is repeatedly rotated about 5-15 times
- Red lesions and ulcerations generally require little pressure and few rotations.
- White lesions, lesions on the palate and gingiva which are typically covered with keratin, require more pressure and more rotations to reach the basement membrane
- After obtaining the sample – the cellular material on the brush – transferred and rotated on the glass slide from one end to another
- The high accuracy of OralCDx is due to the fact that analyses of oral brush biopsies are accomplished with the assistance of sophisticated computers and advances in image recognition
Indication:
- Small or tiny, nonsuspicious, common, unexplained red or white spots.
Contraindication:
- Lesions that are highly suspicious and require immediate scalpel biopsy.
- Lesions with an intact epithelium – submucosal masses, pigmented lesions, fibromas and mucoceles should be biopsied with a scalpel when indicated.
Article by Dr. Siri P.B.