Modern dentistry is undergoing a technological revolution, driven by the integration of advanced digital tools in diagnostics, planning and treatment. Among these, computer-guided implantology has become a cornerstone, particularly in complex procedures like aesthetics and full-arch rehabilitation.1 This approach not only increases surgical precision, but also reduces complications, enhances patient comfort and streamlines the workflow.2 By combining CBCT imaging, intra-oral scanning and planning software, clinicians can carry out virtual simulations that transition seamlessly into clinical execution. Surgical guides allow implants to be placed almost exactly as pre-planned.3
Full-arch rehabilitation remains one of implantology’s greatest challenges, requiring restoration of function, aesthetics and long-term stability in patients with limited anatomical reference points. The digital workflow enables accurate planning tailored to each patient, improving control and predictability throughout treatment. In addition, intra-oral scanners allow for fast, precise and non-invasive data acquisition.4 Their high-quality output now rivals that of traditional impressions, offering an improved patient experience and immediate usability in prosthetic design.5
The integration of intra-oral scan data with CBCT data forms a unified digital model—a digital twin—that supports prosthetic planning, surgical guide fabrication and identification of anatomical constraints. Artificial intelligence (AI) adds further potential by processing large datasets to assist in diagnosis, implant positioning and biomechanical analysis.6, 7
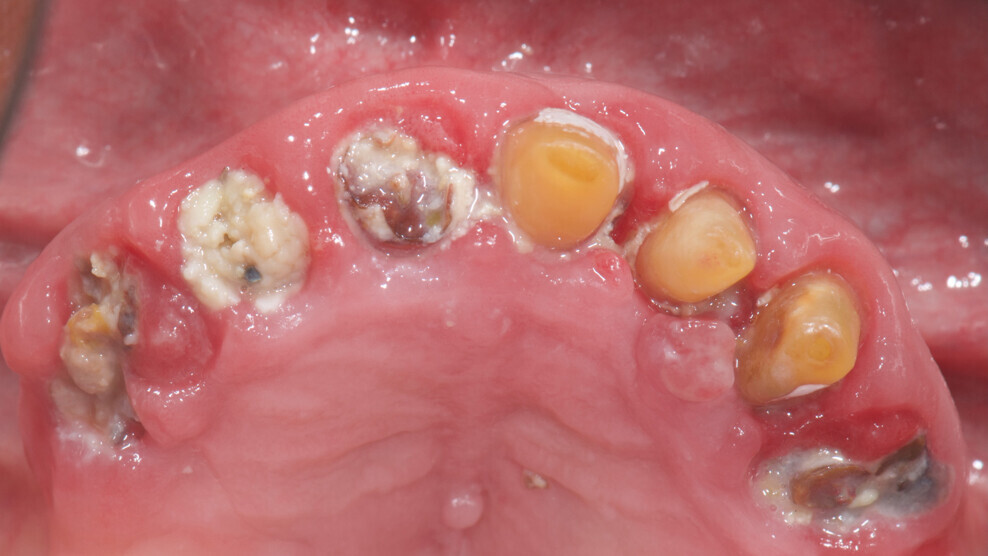
Fig. 2: Initial situation, occlusal view.
Clinically, these technologies lead to more accurate implant placement, optimised prostheses and shorter, less invasive procedures—often making immediate loading easier. However, success depends also on implant characteristics and proper training. Decades of research has shown that implants with superior hydrophilicity potentially improved clinical outcomes by accelerating healing and facilitating immediate loading protocols.8
Clinicians must understand digital workflows, software logic and how to manage complex edentulous cases, where diagnosis, precision and accuracy are vital. Guided surgery translates virtual planning into highly accurate clinical procedures.9 3D-printed guides help minimise deviations and reduce surgical trauma. Still, maintaining high standards throughout the workflow is essential—from impressions and guide design to delivery of the definitive prosthesis. Collaboration with dental laboratories is key. Digital communication allows for custom prostheses that are virtually validated and precisely manufactured using CAD/CAM. This enhances efficiency, reduces errors and elevates overall treatment quality.
Ultimately, the convergence of CBCT, AI, intra-oral scanning and 3D printing is reshaping dentistry into a predictive, preventive and personalised discipline. Full-arch rehabilitation exemplifies the benefits of this shift, making computer-guided implantology not just a technique but a patient-centred philosophy built on precision, safety and clinical excellence.10
Case report
An 85-year-old partially edentulous patient was referred to our clinic for full-arch rehabilitation of the maxilla. The patient was in good general health and a non-smoker. His primary complaints included difficulty in chewing, maxillary pain and occasional halitosis. Clinical and radiographic evaluation revealed a short-span fixed metal–ceramic prosthesis supported by seven anterior maxillary teeth. The prosthesis had debonded, and four of the abutment teeth were structurally compromised. The remaining three showed varying degrees of caries and periodontal problems. A diagnosis of failing dentition was established (Figs. 1 & 2).
At the initial visit, digital impressions were captured using the Medit i700 scanner to document the residual teeth, soft tissue, existing prosthesis and opposing arch. The occlusal records were obtained at the current vertical dimension of occlusion and in centric relation. Mandibular movements were recorded with the zebris JMA jaw registration system (zebris Medical). Intra- and extra-oral photographs were also taken. A virtual diagnostic wax-up and a digital smile simulation were created based on these records (Smile Creator, exocad). Finally, eight implants were planned (Figs. 3 & 4) according to the new wax-up (exoplan 3.1, exocad), and both a surgical guide and a metal-reinforced temporary prosthesis were fabricated in advance (Figs. 5–7).
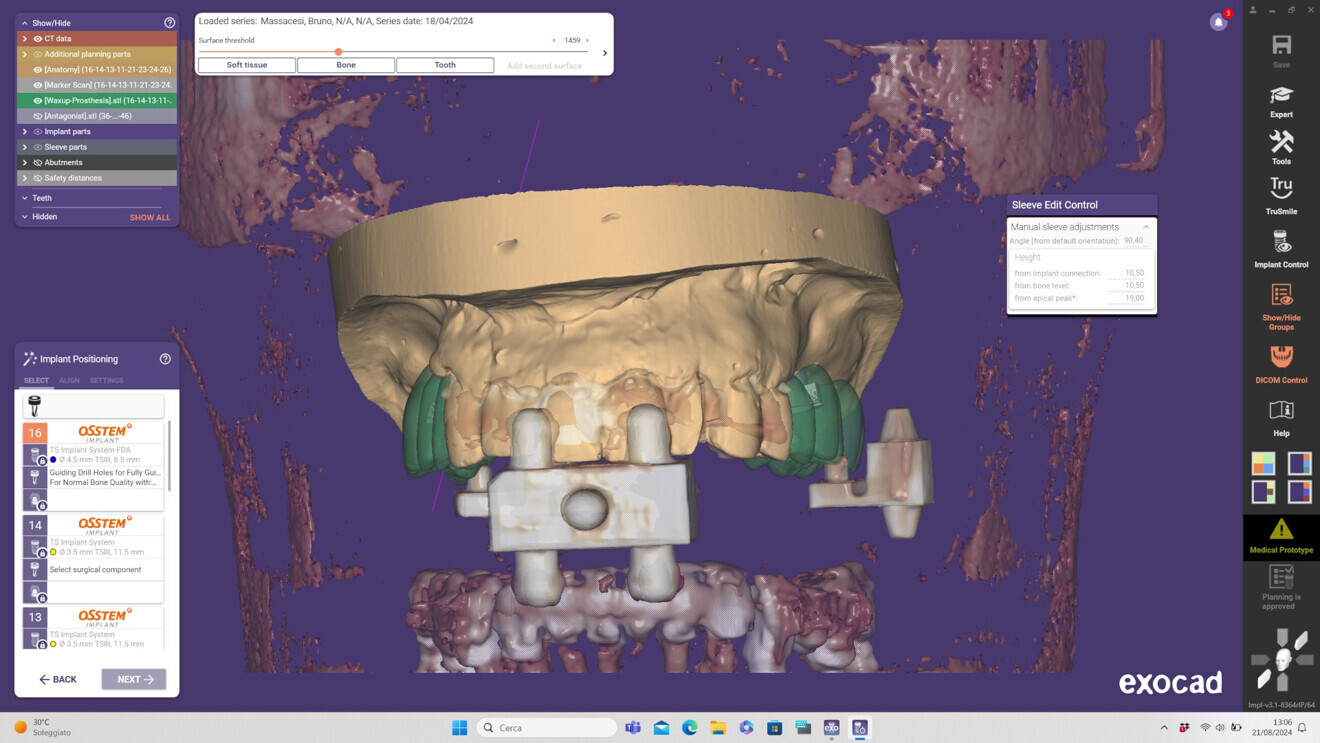
Fig. 3: Virtual implant planning. Matching of CBCT and intra-oral scans using an external marker in exoplan 3.1.
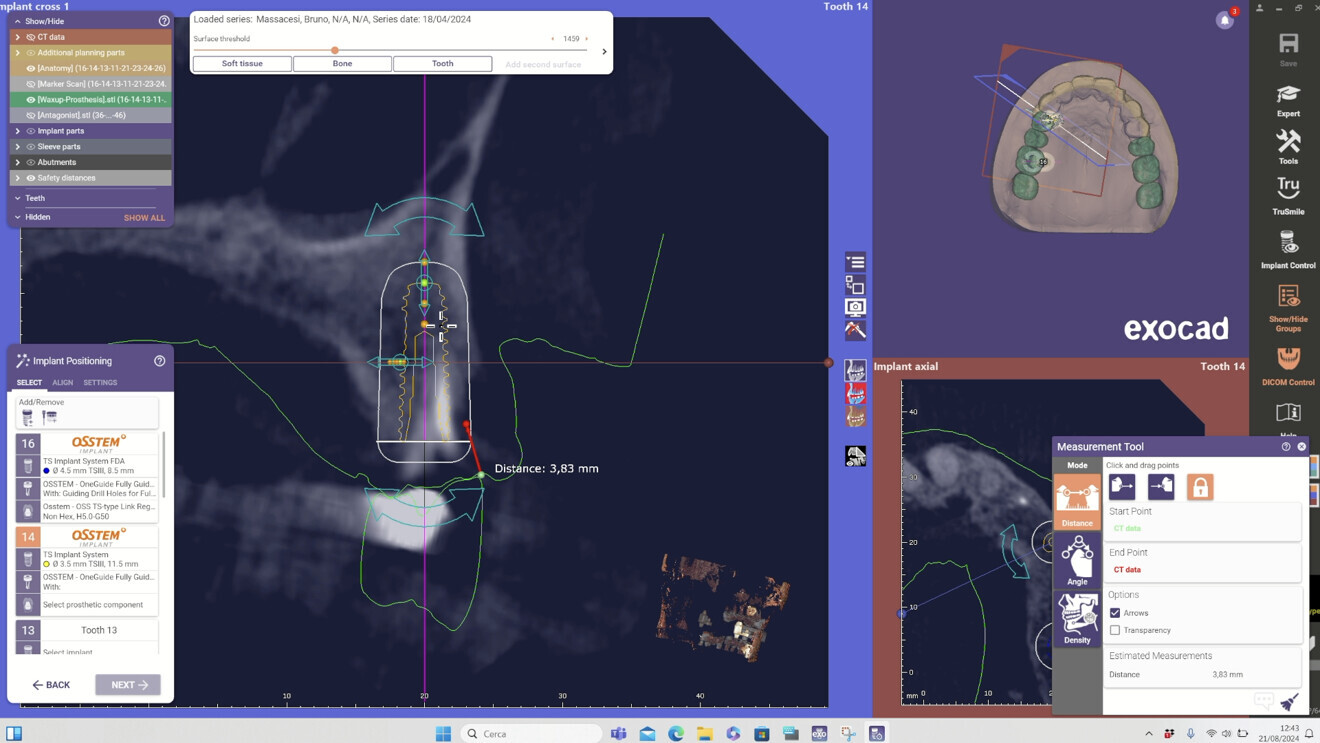
Fig. 4: Virtual implant planning of an immediate post-extraction site in exoplan 3.1.
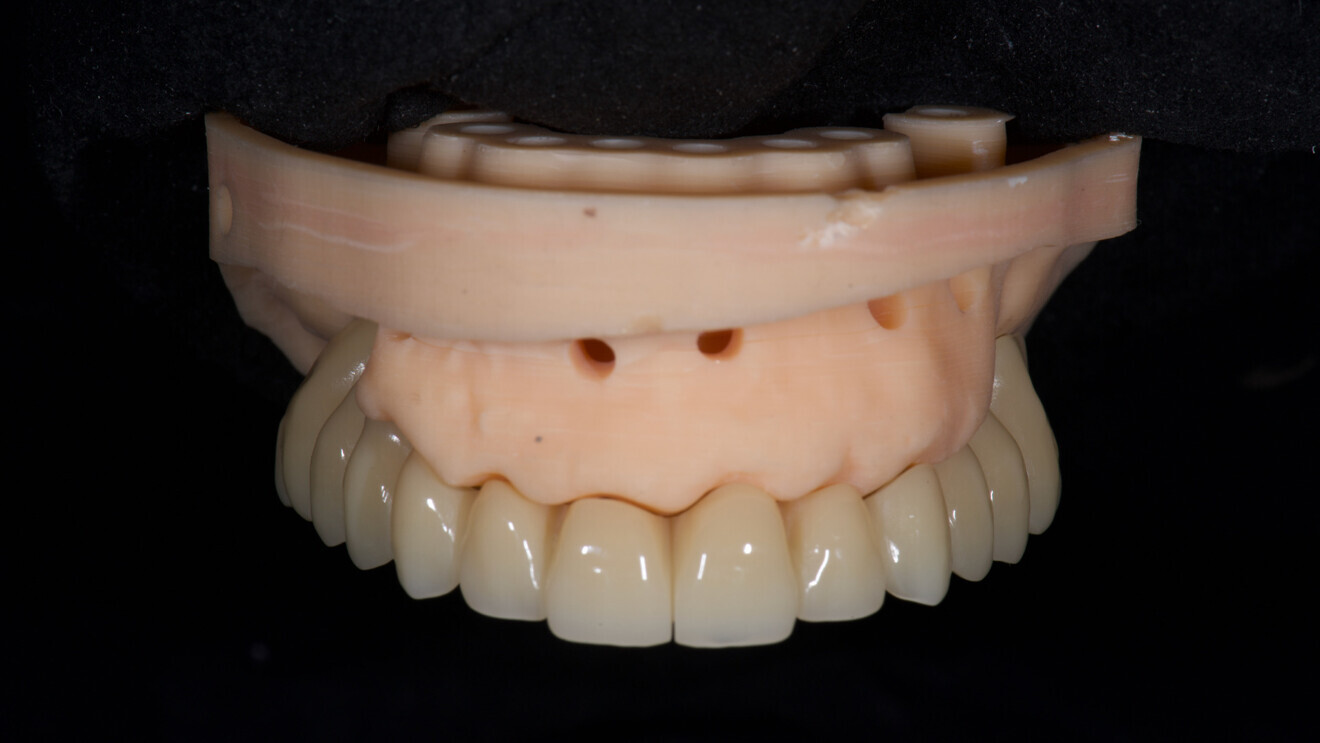
Fig. 5: Prefabricated temporary prosthesis made of PMMA.



