Over the last two decades, there has been an increasing demand for accelerated dental implant treatment protocols to minimise treatment duration and to avoid the need for provisional removable prostheses. However, immediate loading of implants was considered a risk factor for early failure owing to occlusal overload.1,2 In the absence of any alternative proposals, implant companies resorted to the anecdotal design of tapered and aggressively threaded implants in an effort to enhance mechanical implant fixation into bone as measured by insertion torque.
This rather carpenter-like approach nonetheless yielded much higher success as clinicians looked to push the envelope with ever-higher insertion torques,3 perceived as increasing primary stability, and achieved comparable survival rates to those of conventional loading protocols, at least in the short to medium term. However, the literature has since become replete with evidence that such high insertion torques, typically > 50 Ncm, are in fact damaging the surrounding bone, these high strains resulting in microfractures, loss of vascularisation, osteocyte cell death and consequently waves of resorption propagating at some distance from the bone-to-implant interface.4–6 At the extreme, this has resulted in excessive marginal bone loss and ultimately compression necrosis and complete implant failure.7,8 In the longer term, it has been proposed that the damage induced in the bone makes it more vulnerable to advancing marginal bone loss and peri-implantitis.9 It is known that healing and therefore osseointegration are delayed and that the resulting integration is of inferior quality, bone-to-implant contact being reduced. Thus, while it may be true that success rates for immediate loading when higher insertion torque is used are comparable to those of conventional implant loading, there remains a broad lack of knowledge about the long-term consequences arising from the damage induced in the peri-implant bone as well as the misconception that lower insertion torques yield higher failure.
The issue is one of perception and threshold. Since many clinicians now happily use torques of 75 Ncm or more, the idea of placing an implant to 20 Ncm seems unreliable at best and high risk at worst, and there has been a complete failure to grasp the notion that 20–25 Ncm represents a likely threshold above which additional increases in torque yield little in the way of added stability, but only damage the bone. I first proposed this idea in 201110 and again discussed it in an editorial in the International Journal of Oral and Maxillofacial Implants,11 and I presented subsequent research demonstrating that baseline resonance frequency analysis (RFA) can yield implant stability quotient (ISQ) values approaching or even exceeding the desired target of 70 when using an insertion torque of ≤ 25 Ncm.12 More importantly, the singular benefit of RFA is the ability to repeat measurements over time, enabling the clinician to infer the dynamic biological changes that are taking place during healing and thus gain objective evidence of ongoing osseointegration, thereby allowing the clinician to restore the implant at the most appropriate time and with greater confidence. In contrast, insertion torque is a once-off measure and can therefore provide no longitudinal information about the dynamic process of osseointegration. The following case report is an everyday example of my own experience of placing implants into extraction sockets, followed by immediate provisionalisation, using low insertion torque and performing RFA to document the ISQ values over time.
Case report
A 37-year-old male patient was referred to my clinic for extraction and replacement of a failing maxillary right central incisor. The history revealed that the patient had suffered a childhood trauma at age 12, when the tooth was fractured close to the gingival margin. The patient underwent endodontic therapy for root canal obturation, and the tooth was crowned. After ten years, the patient became aware of symptoms, and a recurrent abscess was diagnosed. The root canal was partially filled with composite to attempt to further obturate it. After a further five years, the patient was provided with a new post and crown. Nonetheless, the infection remained, so approximately nine years before, the tooth had undergone apicoectomy, after which it settled down for a period, but it flared up again in early 2024. At that point, the patient was referred to my practice for treatment.
On examination, the patient presented with a minimally restored dentition with a few composite restorations and a crown on tooth #11. The tooth being in the aesthetic zone increased the challenge of delivering a good outcome. The patient had a healthy periodontium and only a few isolated non-pathological pockets of 4–5 mm in depth at the lingual surfaces of the mandibular molars, accompanied by some minor bleeding on probing. The patient was advised to seek more regular hygiene focusing on these areas.
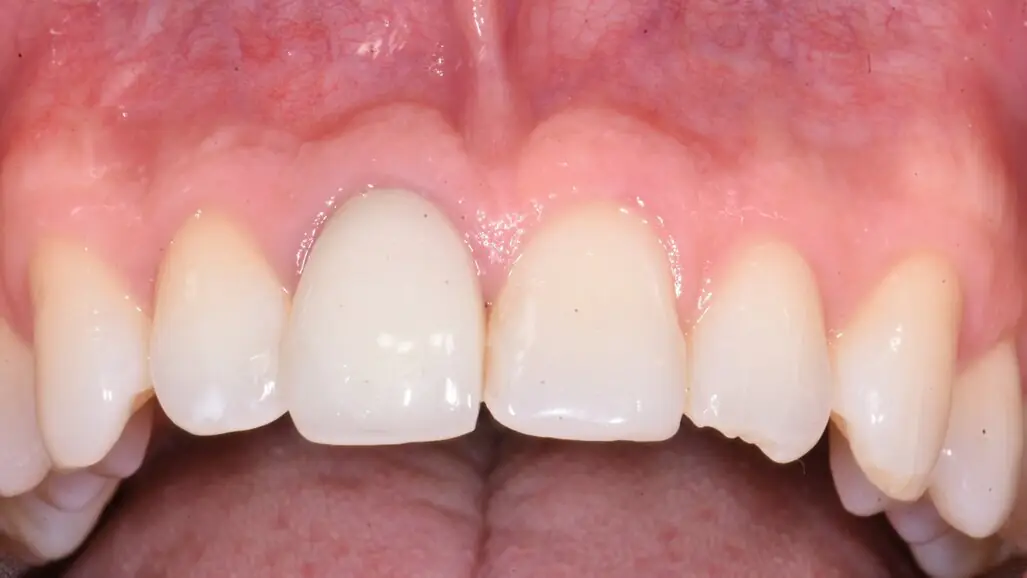
Tooth #11 was immobile and associated with adequate ridge width and a wide band of keratinised tissue (Fig. 1). There was also a favourable Class I incisor relationship and adequate space to accommodate an implant-supported restoration. A CBCT scan of the site revealed an inadequately endodontically treated tooth with a lack of an apical seal and incomplete obturation of the canal. The tooth benefited from good bone support provided by a robust facial bone plate at the alveolar crest (Fig. 2), but there was a large periapical dentigerous cyst measuring approximately 10 × 8 mm, extending to the mesial surface of tooth #12, and complete fenestration of the facial plate superiorly (Fig. 3). The prognosis of the tooth was deemed to be hopeless, and extraction was indicated.
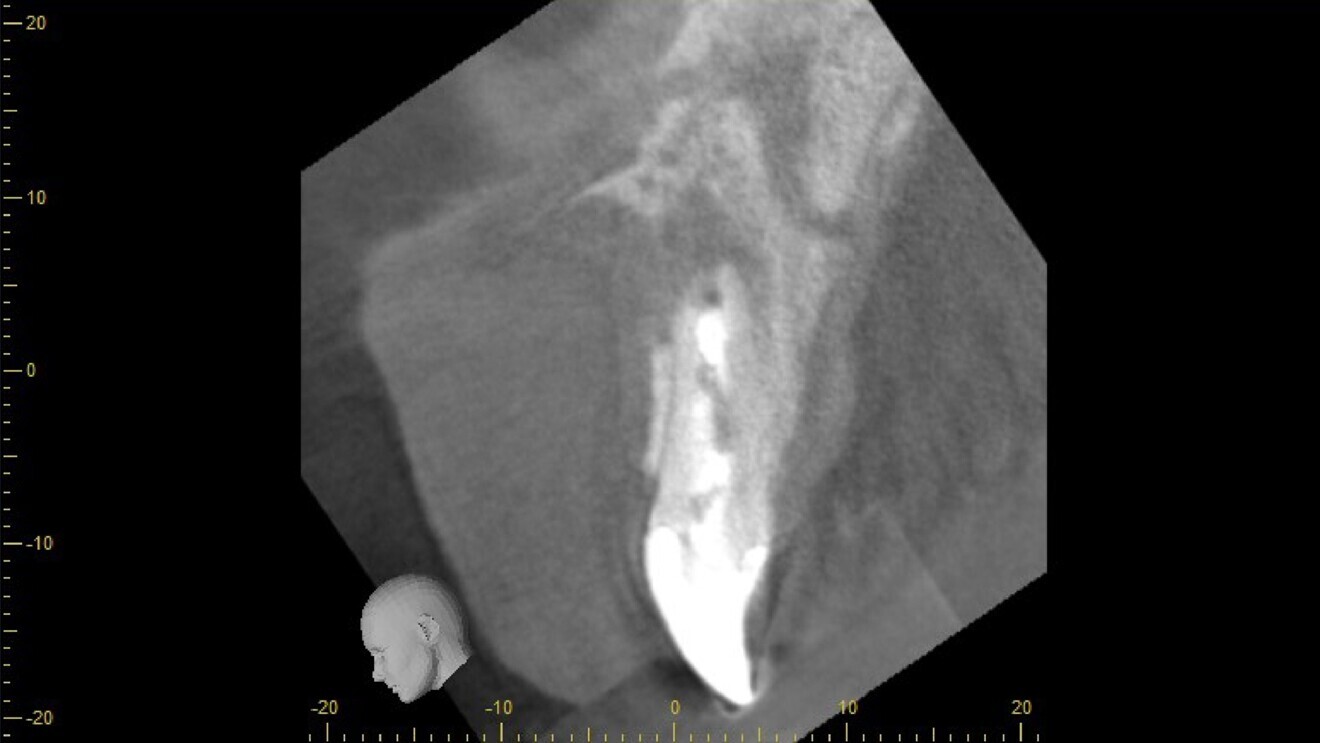
Fig. 2: CBCT scan of failing tooth #11, showing inadequate root canal treatment and apical fenestration but an intact labial-crestal plate.
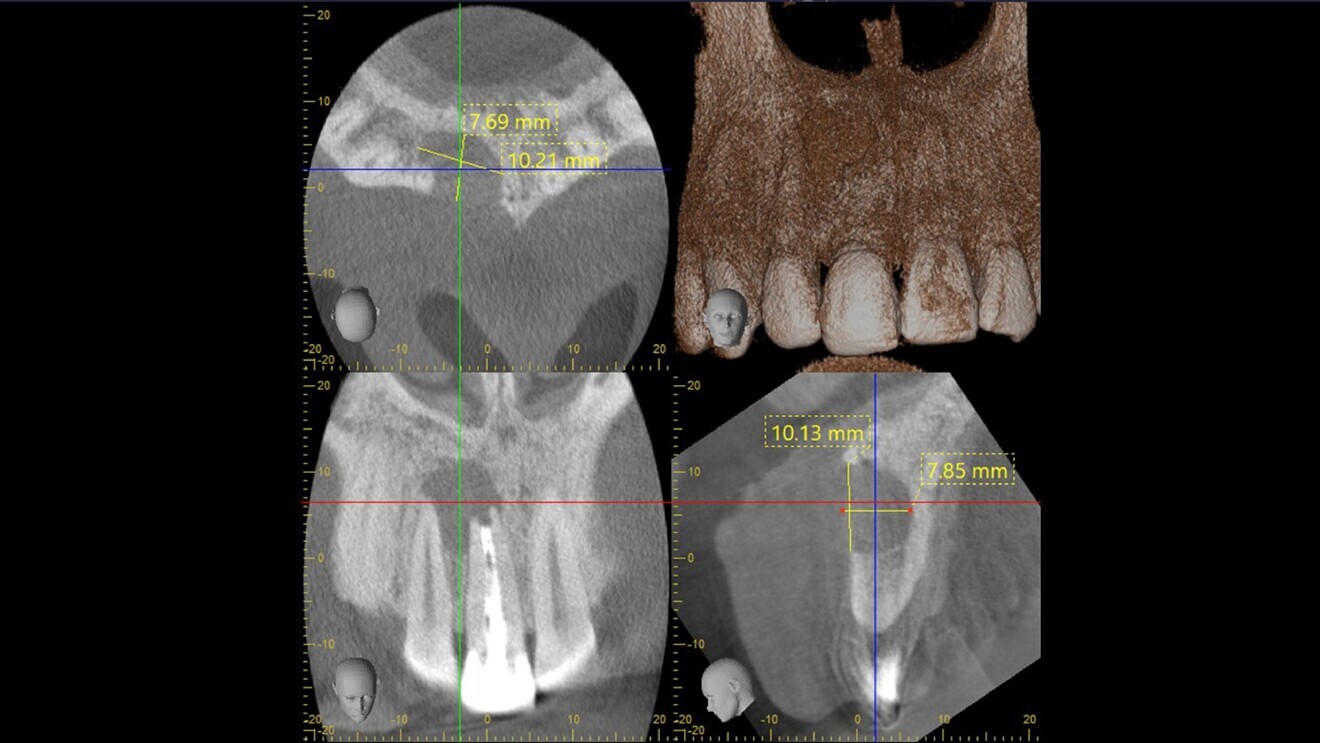
Fig. 3: Cystic cavity measuring approximately 10 × 8 mm.
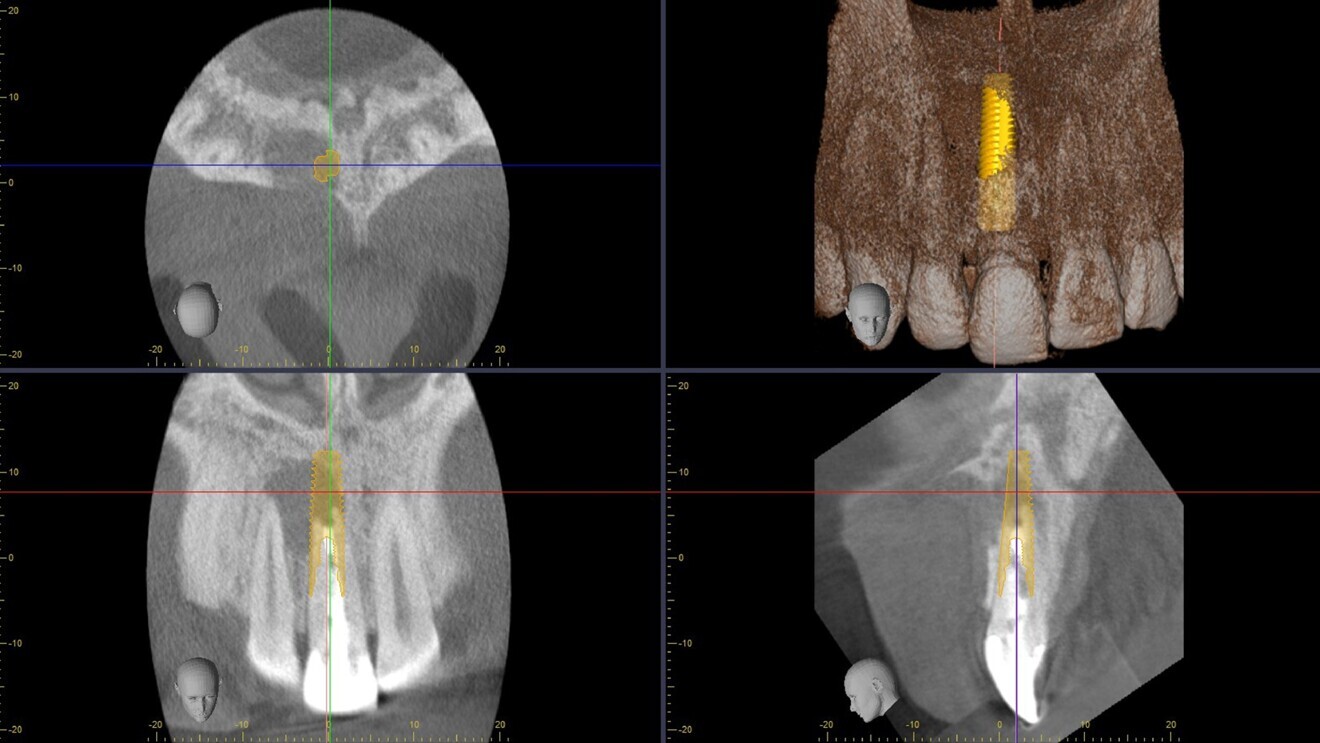
Fig. 4: CBCT scan showing the planned implant placement.
Typically, with such a large cyst, the treatment plan would be extraction, cyst enucleation and grafting, followed by implant placement after healing of the graft, and the patient would be provided with a provisional, often removable, prosthesis. However, I have for many years specialised in complex immediate implant placement and have published extensively on the use of low insertion torque with high success, even in the case of immediate provisionalisation. Accordingly, the risks and benefits were discussed with the patient, who elected for a simultaneous approach and immediate restoration. This was planned in the CBCT scan using i-Dixel software (Morita) for the placement of a PrimeTaper EV implant (Dentsply Sirona, 4.2 × 17.0 mm; Fig. 4), and a bovine bone mineral substitute was chosen as the grafting material.
An atraumatic extraction protocol was used, involving initial luxation with a periotome and a rotational rather than facial-palatal method of displacement, thereby preserving the facial plate. Once the tooth had been extracted, a sub-sulcular envelope incision was used to gain access to the lesion, and the cyst was enucleated and the surrounding bone curetted and decontaminated (Fig. 5). A surgical guide was used to ensure the optimal position of the implant (Fig. 6), and the apical cutting threads of the PrimeTaper EV implant (Fig. 7) ensured that the implant engaged effectively with the apical bone, but the insertion torque only reached 20 Ncm owing to the large cyst-related cavity and the resulting lack of significant initial bone-to-implant contact. The baseline ISQ value was 61 and 65 in the facial-palatal and mesiodistal directions, respectively (Fig. 8), but in my experience, this combination of torque and ISQ value indicated that the implant was suitable for immediate loading, since the torque was ≥ 20 Ncm and the ISQ value was ≥ 65 in one direction.
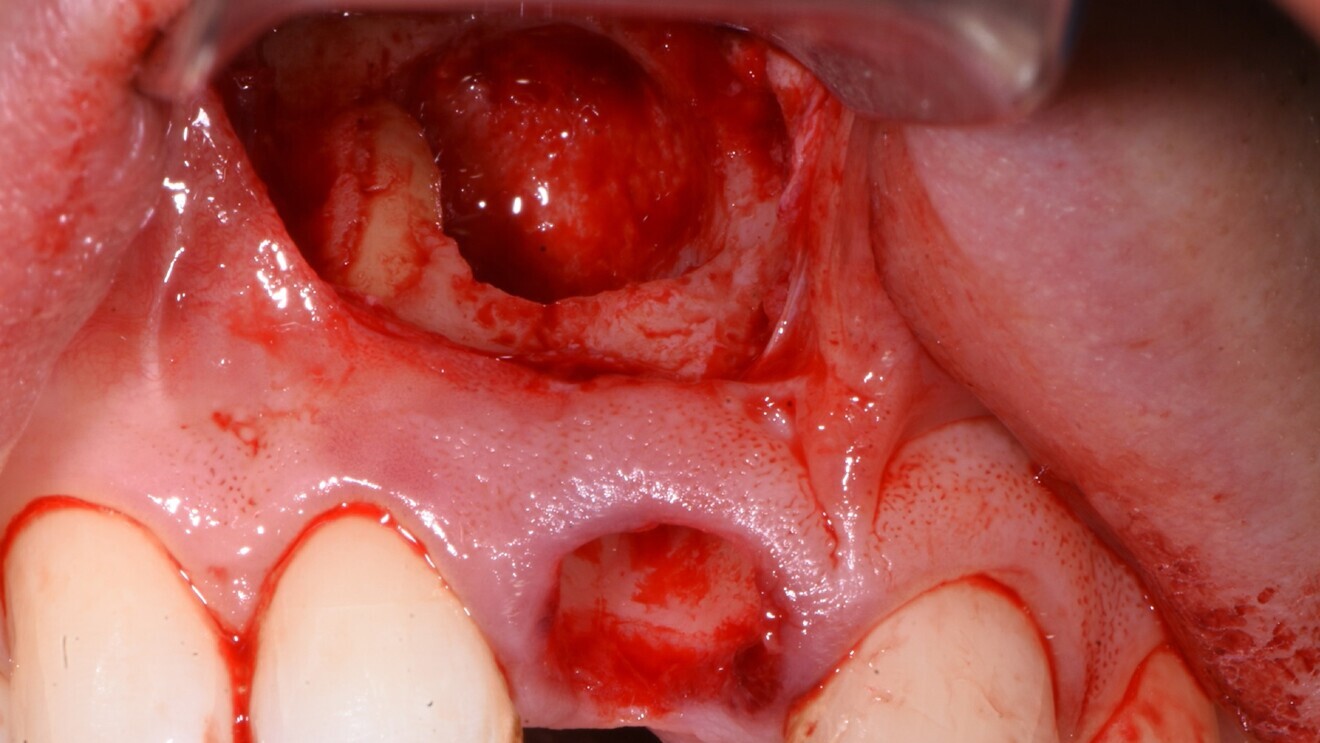
Fig. 5: Extraction socket with the infra-bony cyst cavity exposed.