In recent years, dental implants have emerged as a pivotal advancement in dentistry, offering a popular solution for replacing natural teeth lost owing to various factors, such as caries, fractures and periodontal disease. However, within the dental community, there remains a divergence in approaches, some advocating for a more conservative stance focused on preserving severely compromised teeth.1 Prioritising the retention of a patient’s natural teeth should remain a fundamental objective for dental professionals.
One proposed method to address structurally compromised teeth is crown lengthening, aimed at providing optimal conditions for tooth restoration. However, challenges arise with this approach, particularly in the aesthetic zone, where certain techniques may be limited by their impact on gingival symmetry.2, 3 The diagnostic and planning process for crown lengthening of anterior teeth is notably intricate, necessitating careful consideration to avoid potential asymmetry in gingival margins. Particularly prevalent in the aesthetic zone, notably the maxillary incisors, dentoalveolar trauma often results in the loss of coronal structure.4, 5 In such cases, restoration of the affected tooth may require additional procedures to achieve adequate supragingival height.
Surgical extrusion is a procedure through which the remaining dental structure is repositioned in a more coronal position within the alveolus.6–8 The primary objective of this technique is to elevate the affected tooth to a more coronal position, thereby creating favourable conditions for establishing an adequate ferrule, crucial for facilitating the placement of a restoration that preserves a healthy biological width.3, 7 Consequently, surgical extrusion can be a valuable approach in the treatment of severely damaged teeth, particularly in the aesthetic zone.
Surgical extrusion has various names, including intra-alveolar transplant, intentional reimplantation and forced eruption.6, 9, 10 Although the technique was initially described in 1978,11 the first case report was not published until 2002.12 Despite its early documentation, surgical extrusion remains relatively uncommon in dental practice.
Initially, the periodontal ligament is delicately loosened through syndesmotomy, followed by careful luxation facilitated by periotomes and/or elevators. Using forceps, the tooth is then gradually extruded, typically achieving a vertical displacement of 4–6 mm. To stabilise the tooth in its new position, it is immobilised for a period of two to three weeks with the aid of a flexible splint, followed by placement of a post and core and subsequently a definitive full-coverage restoration. This effective technique can be implemented with relative ease, requiring no specialised surgical expertise. Moreover, it often yields satisfactory aesthetic results, boasts a low failure rate and tends to be well received by patients.
Case series and clinical reports are classified as low-evidence literature because the causal relationships between intervention and outcomes cannot be definitively established without a control group.13, 14 Nonetheless, clinical reports can influence decision-making in dental practice,14 for example by raising awareness of new techniques, clinical approaches and research directions. The objective of this case report is to present a four-year follow-up clinical case in which a compromised anterior tooth was preserved through surgical extrusion.
Case report
A female patient was evaluated in the dental office after a traumatic event involving her maxillary teeth. She had an oblique fracture from the mesial to distal aspect of the maxillary left central incisor at subgingival level, and the tooth’s metal post and metal–porcelain crown presented with mobility. The tooth had healthy periapical tissue (Fig. 1). Upon radiographic and clinical evaluation, it was noted that there was insufficient dental structure for a predictable restoration.15 Treatment planning included measurement and analysis of the root length, of the width of the root canal walls and of the available supragingival structure. Various treatment options were considered to save the tooth, and after a comprehensive evaluation, surgical extrusion was chosen as the preferred option to achieve adequate healthy supragingival dental structure, thereby offering the patient a favourable long-term treatment solution.6, 8
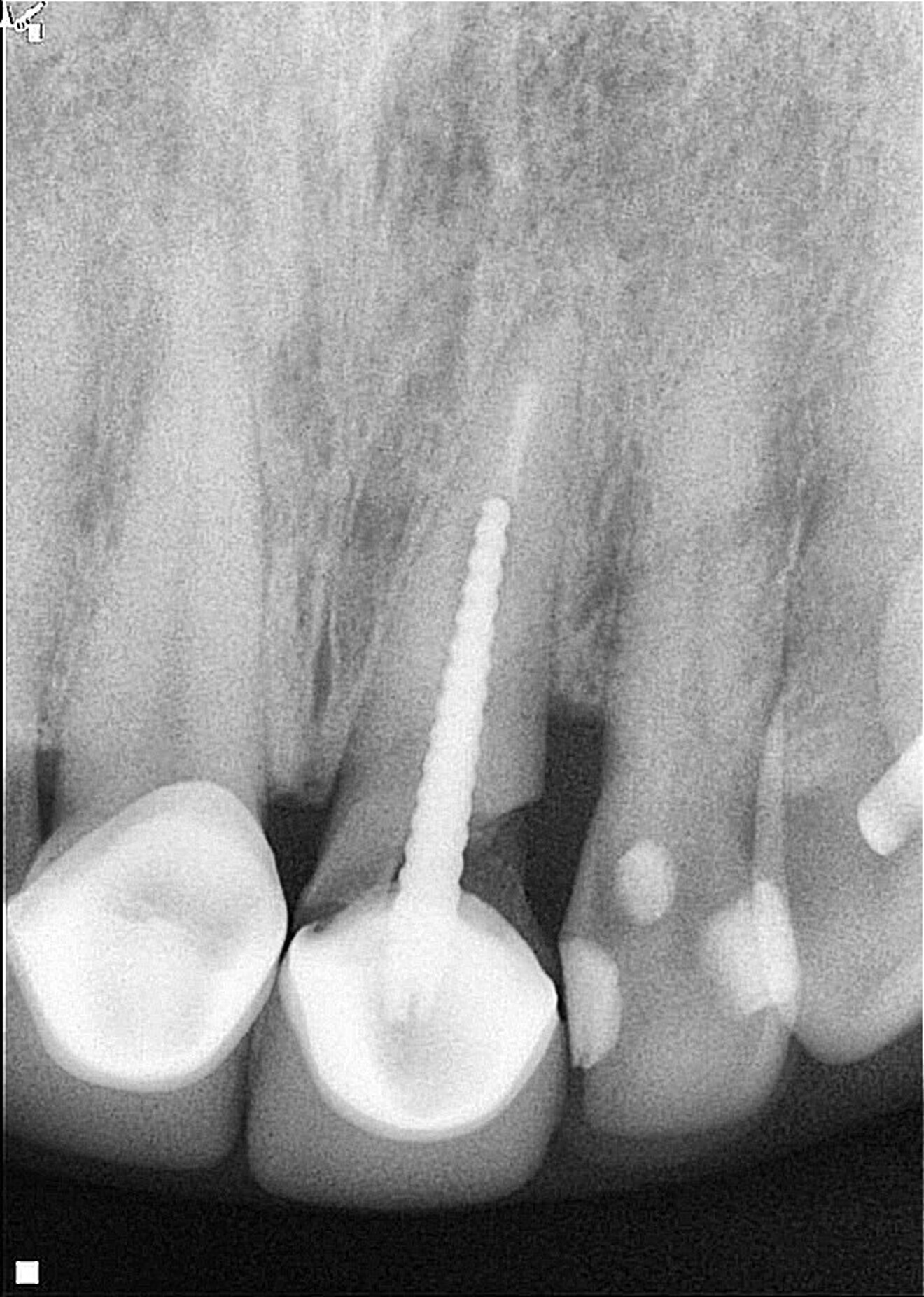
Fig. 1: Initial clinical radiograph showing tooth #21 with a previous root canal treatment, a metal post, a full-coverage coronal restoration and an oblique fracture from the mesial to distal aspect.
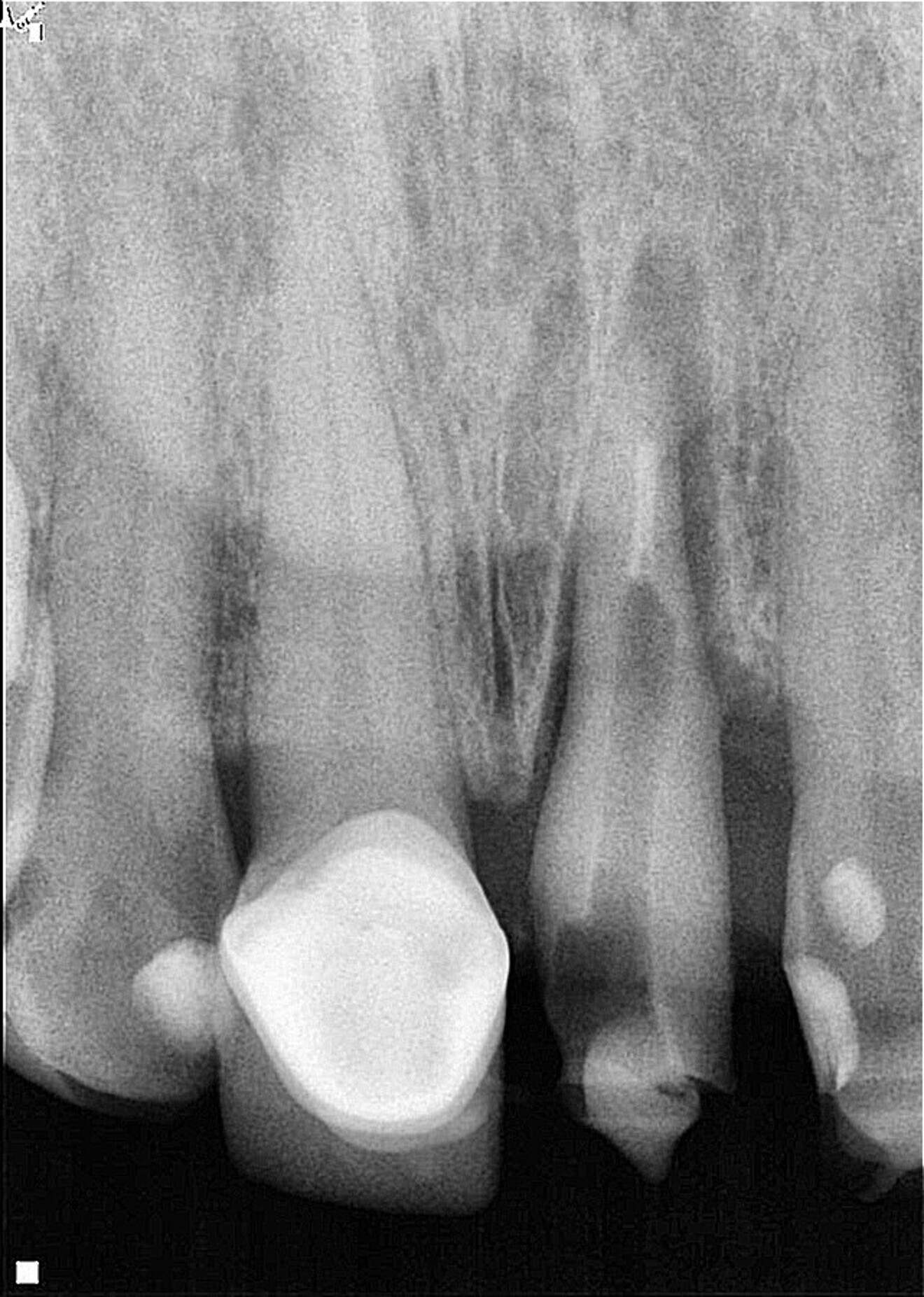
Fig. 2: Post-op radiograph of the tooth extruded by approximately 6 mm and rotated by 180°, locating the deeper zone of the fracture towards the mesial aspect.
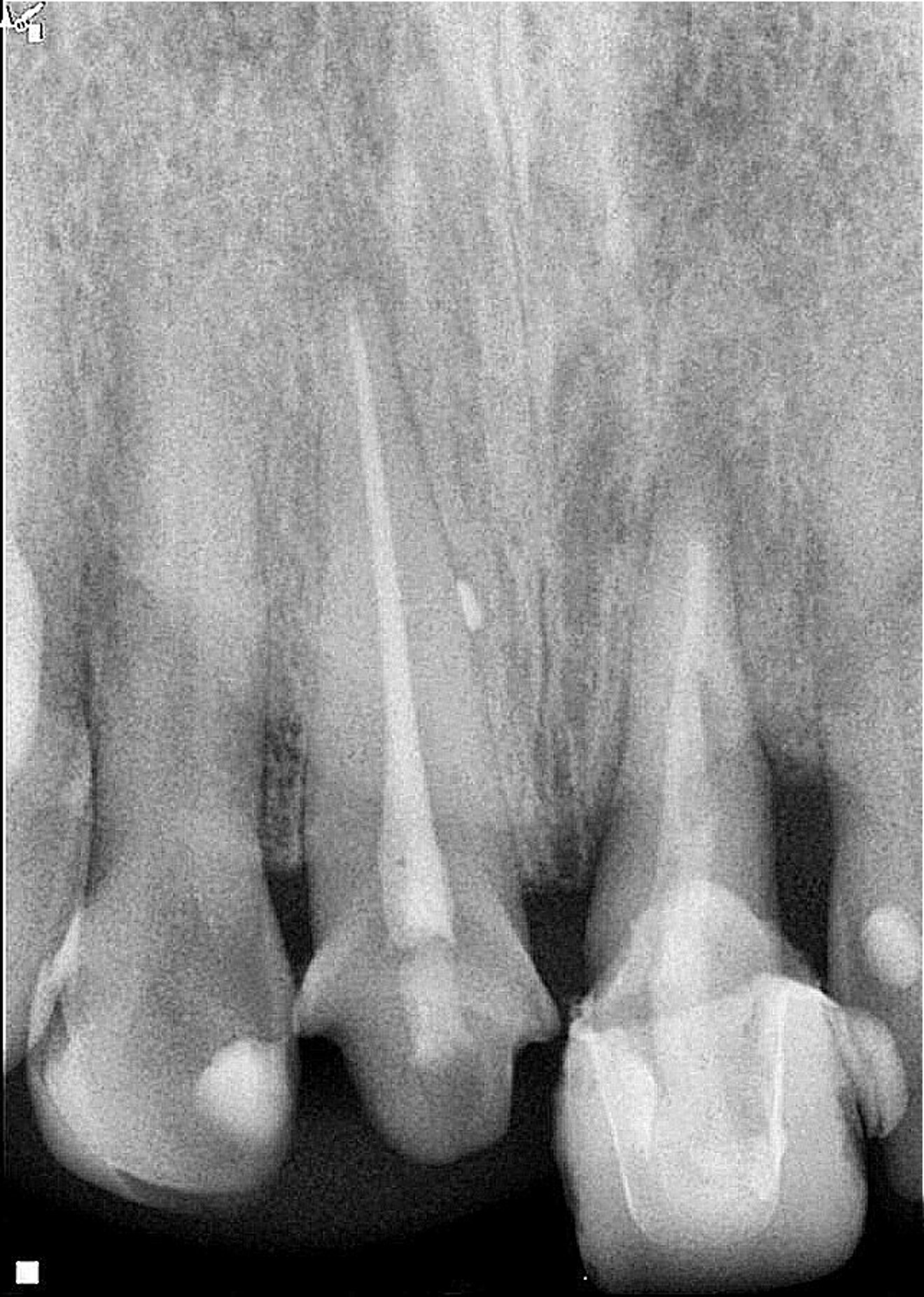
Fig. 3: Eight-week follow-up radiograph with the provisional crown in place showing bone remodelling of the mesial and distal aspects of the bone crest and periapical healing in progress.
After removing the metal–porcelain crown and disinfecting the affected area using a gauze dampened with 2% chlorhexidine (GLUCO-CHeX 2%, CERKAMED), syndesmotomy was performed with a No. 15c scalpel, followed by luxation of the root using a small periotome. Luxation forces were applied only to the first 3 mm of the radicular structure at the mesial aspect with the objective of avoiding damage to the periodontal ligament, which was intended to remain in an infra-osseous position. Once the tooth had been loosened, it was extruded by approximately 6 mm and rotated by 180° (Fig. 2). The rotation was performed with the purpose of positioning healthy periodontal ligament fibres in the distal area because the crestal bone already had an oblique defect at this site. Usually the bone follows the extruded periodontal ligament fibres during this type of procedure, making vertical bone gain possible.8, 15, 16 The rotation also allowed us to limit the extent of extrusion. The extrusion and rotation were managed with forceps, grasping only the coronal portion of the tooth, which was planned to remain in a supra-osseous position after the treatment.
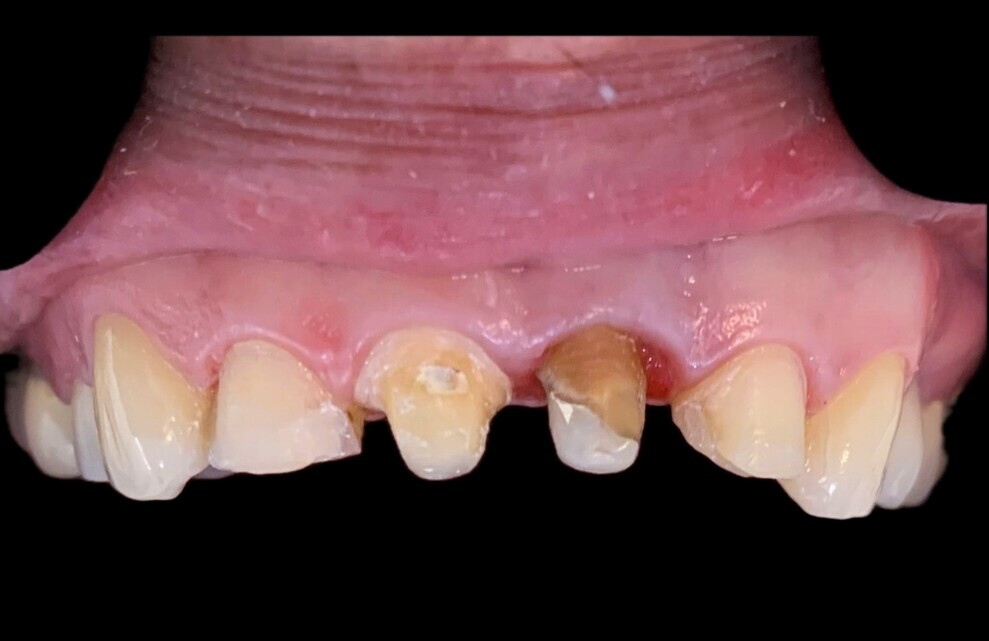
Fig. 4: Clinical situation just before placement of the definitive restoration.
When the tooth reached the desired position, gentle pressure was applied in a labial–palatal direction using a gauze soaked with chlorhexidine to achieve haemostasis before splinting the tooth. While interdental sutures for stabilising the tooth are the first choice according to the literature,17 we chose to use nylon monofilament line with a diameter of 1 mm. This decision was based on its cost-effectiveness, availability, flexibility for splinting, and non-plaque-retentive surface, facilitating good oral hygiene maintenance by the patient. The splint was applied using a flowable composite resin (Nexcomp Flow, Meta Biomed) and a two-step adhesive protocol (EZ Bond Universal, Meta Biomed). The splinting duration was set at three weeks, as recommended to achieve dental stability and minimise the risk of ankylosis.17, 18 The literature indicates that mobility will decrease cons