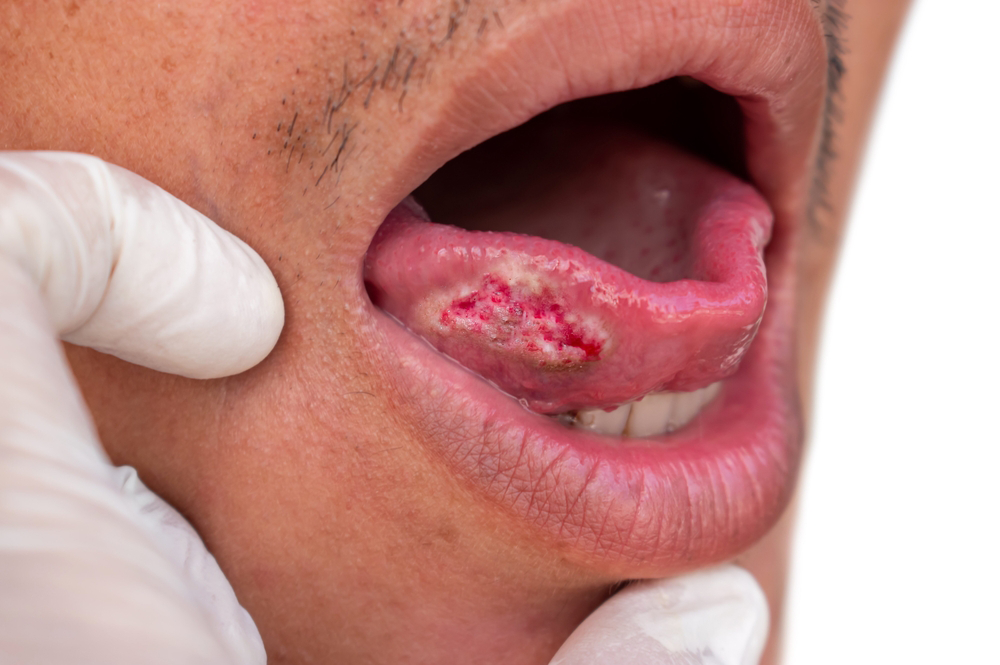
 In dentistry, comprehensive patient care goes far beyond prophylactic treatments and restorative work. Oral cancer detection is also a pivotal aspect of a dental clinician’s meticulous visual and tactile examination during routine dental check-ups. , ,Clinicians typically begin the oral cancer detection process by closely inspecting the oral cavity, including the lips, buccal mucosa, gingiva, tongue, floor of the mouth, and palate, for any abnormalities such as persistent ulcers, lumps, or red or white patches. Palpation is crucial, involving a thorough assessment of lymph nodes in the head and neck region for potential signs of metastasis., ,Advanced diagnostic tools further enhance the detection process. Intraoral imaging effectively aids in identifying suspicious lesions that may not be apparent during a standard visual examination. Additionally, biopsies are instrumental for definitive diagnosis, involving the removal and analysis of a tissue sample for pathological evaluation., ,Recognizing the warning signs is paramount. Persistent nonhealing sores, changes in oral sensation, and unexplained bleeding are red flags that demand attention. Timely identification allows for intervention in early stages when treatment outcomes are more favorable., ,Treatment options vary based on the extent and stage of oral cancer. Surgical resection, radiation therapy, and chemotherapy are common modalities, often employed in combination for optimal results. , ,The collaborative efforts of dental clinicians, oral surgeons, and oncologists play a crucial role in navigating the complexities of oral cancer management. Regular continuing education on evolving diagnostic technologies and treatment protocols empowers dental clinicians in contributing significantly to the timely detection and management of oral cancer within their practice.
In dentistry, comprehensive patient care goes far beyond prophylactic treatments and restorative work. Oral cancer detection is also a pivotal aspect of a dental clinician’s meticulous visual and tactile examination during routine dental check-ups. , ,Clinicians typically begin the oral cancer detection process by closely inspecting the oral cavity, including the lips, buccal mucosa, gingiva, tongue, floor of the mouth, and palate, for any abnormalities such as persistent ulcers, lumps, or red or white patches. Palpation is crucial, involving a thorough assessment of lymph nodes in the head and neck region for potential signs of metastasis., ,Advanced diagnostic tools further enhance the detection process. Intraoral imaging effectively aids in identifying suspicious lesions that may not be apparent during a standard visual examination. Additionally, biopsies are instrumental for definitive diagnosis, involving the removal and analysis of a tissue sample for pathological evaluation., ,Recognizing the warning signs is paramount. Persistent nonhealing sores, changes in oral sensation, and unexplained bleeding are red flags that demand attention. Timely identification allows for intervention in early stages when treatment outcomes are more favorable., ,Treatment options vary based on the extent and stage of oral cancer. Surgical resection, radiation therapy, and chemotherapy are common modalities, often employed in combination for optimal results. , ,The collaborative efforts of dental clinicians, oral surgeons, and oncologists play a crucial role in navigating the complexities of oral cancer management. Regular continuing education on evolving diagnostic technologies and treatment protocols empowers dental clinicians in contributing significantly to the timely detection and management of oral cancer within their practice.


