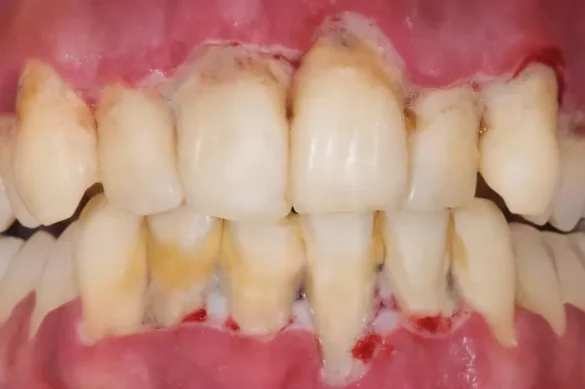
Necrotizing periodontal disease is a severe and rapidly progressing oral condition that affects the gums and the surrounding structures of the teeth. It is marked by distinctively painful symptoms and can lead to significant tissue loss in a very short time. This disease mainly occurs in individuals with weakened immune systems or those exposed to specific risk factors, emphasizing the vital need for early recognition and management.
What Is Necrotizing Periodontal Disease?
necrotizing periodontal disease (NPD) is a term covering a group of related infections that result in the death (necrosis) of gum tissue. NPD may include necrotizing gingivitis, necrotizing periodontitis, and necrotizing stomatitis, depending on which tissues are affected and how far the disease has progressed. These conditions form one category of periodontitis as defined by leading dental organizations. NPD distinguishes itself by the rapid breakdown of gum tissue, spontaneous pain, and its tendency to spread if not addressed promptly.
Forms and Stages of necrotizing periodontal disease
NPD presents in several forms. The mildest form is necrotizing gingivitis, which only affects gum tissues. If the disease progresses, it evolves into necrotizing periodontitis, characterized by the destruction of the ligaments and bone supporting the teeth. In severe cases, the infection spreads beyond the gums into surrounding oral structures, known as necrotizing stomatitis. In the most advanced and rarest stage—noma—major destruction of mouth and facial tissues can occur, usually among malnourished children in low-resource areas.
Clinical Features and Symptoms
The most distinguishing feature of necrotizing periodontal disease is tissue necrosis. Patients typically experience intense gum pain, spontaneous bleeding, and rapid onset of symptoms. Other common signs include:
- severe halitosis (bad breath), often with a characteristic unpleasant odor
- swollen and ulcerated gums with a greyish pseudomembrane (a protein and white blood cell layer over dead tissue)
- Crater-like or “punched-out” appearance of the gums
- Swelling or tenderness in the lymph nodes beneath the jaw
- fever and general discomfort in advanced stages
- Difficulty in eating due to pain, which can lead to poor nutrition
Loss of gum attachment and the exposure of tooth roots or bone can occur quickly. Deep periodontal pockets are rare since the rapid tissue destruction does not allow time for typical pocket formation seen in other gum diseases.
Causes and Key Risk Factors
necrotizing periodontal disease is primarily caused by bacterial infections in the mouth. Certain bacteria, such as Prevotella, Treponema, Selenomonas, Fusobacterium, and spirochetes, play a major role. However, the disease typically only develops in the presence of specific risk factors such as:
- weakened immune system (e.g., HIV/AIDS, underlying medical conditions)
- malnutrition and vitamin deficiencies
- poor oral hygiene and accumulation of plaque
- Using tobacco products
- Extreme psychological stress or sleep deprivation
- pre-existing gum disease or history of necrotizing periodontal conditions
These risk factors compromise the body’s ability to keep normal mouth microorganisms in check, increasing vulnerability to infection and rapid tissue destruction.
Diagnosis
Diagnosing NPD is primarily clinical, based on the appearance of the gums, patient history, and associated risk factors. Dentists or periodontists will often note the typical ulcerated, “cratered” gingival tissues, spontaneous bleeding, and pseudomembrane formation. Additional diagnostic steps may include:
- X-rays to check for bone loss around the teeth
- Blood tests to uncover underlying immunosuppression or other conditions
- Evaluation for symptoms of systemic illness
Careful investigation helps confirm the disease while excluding other similar mouth illnesses, such as herpetic infections, allergic reactions, or abrasive injuries.
Complications and Disease Progression
If NPD is not detected and managed early, the risk of severe complications increases. These can include:
- progressive loss of soft tissue and bone supporting the teeth
- tooth loosening or eventual tooth loss
- Extension of infection into the cheeks, tongue, or palate (necrotizing stomatitis)
- In rare, extreme cases, widespread destruction of facial tissues (noma)
Worsening oral function, changes in appearance, and increased risk of secondary infections can all result, especially in populations with significant underlying health or nutritional deficits.
Treatment Approaches
Early and comprehensive treatment is essential to control necrotizing periodontal disease and prevent further tissue damage. Therapy is tailored to the stage of the disease and typically includes:
- mechanical removal (debridement) of dead tissue and bacterial deposits by a dental professional
- Prescription of antiseptic mouth rinses or systemic antibiotics (such as metronidazole)
- Pain management with suitable medications
- Strong emphasis on oral hygiene maintenance: brushing twice daily, careful cleaning, and regular dental checkups
- Addressing and correcting risk factors where possible, such as improving nutrition, stopping tobacco use, and managing psychological stress
In advanced or complicated cases, oral surgery may be needed to reconstruct lost gum or bone tissue and restore function. Successful treatment also involves identifying any underlying or systemic disease—such as HIV infection or other immune disorders—and coordinating medical care as necessary.
Prevention Strategies
Because NPD is strongly linked to modifiable risk factors, prevention is both possible and effective. Key preventive actions include:
- Maintaining good daily oral hygiene practices (regular brushing and flossing)
- Professional dental cleanings and check-ups
- Ensuring adequate nutrition, vitamins, and access to safe water and food
- Reducing or eliminating tobacco products
- Practicing stress management and ensuring enough sleep
- Managing any chronic illnesses in consultation with a healthcare team
Early identification and prompt action at the first signs of mouth discomfort or bleeding can prevent significant damage and improve outcomes.
Conclusion
necrotizing periodontal disease is a serious but preventable form of gum disease that can rapidly cause severe damage to mouth tissues if left unmanaged. With its strong association with immune suppression, poor oral hygiene, and additional risk factors, awareness and early diagnosis are critical. Treatment focuses on removing the infection, restoring oral health, and addressing underlying causes. By following sound preventive measures and seeking timely care, most people can avoid the most harmful consequences and preserve their oral health.
Frequently Asked Questions
What are the early signs of necrotizing periodontal disease?
The earliest symptoms are gum pain, spontaneous bleeding, and swollen, ulcerated gums with a bad smell. Prompt dental consultation is advised at the first sign of these symptoms.
Can necrotizing periodontal disease be cured?
If caught and treated early, NPD can be controlled and reversed. If detected late, some tissue loss may be permanent, but treatment can still halt the disease and prevent its spread.
Is necrotizing periodontal disease contagious?
No. Although the bacteria responsible are common in the mouth, NPD only develops in people with certain risk factors. It does not spread directly from one person to another.
Who is most at risk?
Individuals with weak immune systems, malnutrition, poor oral hygiene, tobacco use, and high stress levels are more susceptible to NPD.