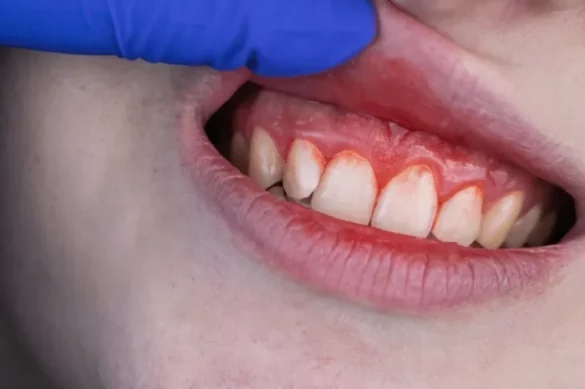
USA — Researchers have released updated, evidence-based guidance to help dentists manage a common but challenging dental condition: gingival recession occurring alongside non-carious cervical lesions (NCCLs).
The findings, published in the Journal of Periodontology by Mauro Pedrine Santamaria of the University of Kentucky College of Dentistry and colleagues, provide a refined framework for clinical decision-making.
Gingival recession, where the gum margin recedes and exposes the tooth root, is frequently seen in dental practice. Roughly half of these cases coincide with NCCLs—areas of tooth structure loss near the gum line not caused by decay. When both conditions appear on the same tooth, they are classified as combined defects (CDs), which are more complex than isolated recession and require customized treatment strategies.
The researchers conducted a narrative review of major databases, including Medline/PubMed, Embase, BIREME, and Google Scholar. They classified NCCLs using the Pini-Prato system and gingival recession according to the Cairo classification and gingival phenotype. Using these criteria, they developed an updated decision tree to guide clinicians toward the most suitable treatments.
Key insights from the review include:
Treatment options vary by defect severity: Mild cervical defects (A−, A+, B−) often do not require restoration. Surgical root coverage alone can suffice.
Technique selection depends on gingival characteristics: The choice of root coverage procedure in mild cases should reflect the type of recession and the patient’s gingival thickness.
Advanced defects require combined approaches: For more severe lesions (B+ or V-shaped), restoring the cervical defect with composite materials alongside root coverage improves both function and aesthetics. Around 25% of CDs fall into this category, underscoring the need for careful assessment and planning.
Gingival phenotype guides grafting decisions: Thin gingival tissue typically benefits from autogenous soft tissue grafts using the patient’s own tissue, while thick tissue may achieve good outcomes without grafts. In moderate cases, both autogenous grafts and commercially available biomaterials may enhance long-term success.
The updated guidance integrates recent evidence, including advances in soft tissue grafting, providing practical recommendations tailored to defect severity and tissue type. By aligning treatment strategies with individual patient needs, the framework aims to improve outcomes for patients and support clinicians in managing these commonly encountered combined periodontal and restorative challenges.