Periodontal disease is a common oral health condition that affects the gums and supporting tissues around the teeth. It is important for both dental professionals and patients to understand how to stage and grade periodontal disease. This knowledge forms the foundation for proper diagnosis, personalized treatment planning, and long-term management. Evaluating the severity and risk of progression of periodontitis helps ensure that each patient receives the most effective care based on their individual needs.
Understanding Periodontal Disease: An Overview
Periodontal disease, also known as gum disease, is the result of chronic bacterial infection and inflammation of the tissues that support the teeth. If left untreated, it can lead to tissue destruction, bone loss, and ultimately, tooth loss. Proper assessment of the disease involves two main steps: staging and grading. staging describes how severe the disease is, while grading assesses how quickly the disease is likely to progress.
The Purpose of staging and grading
The staging and grading system of periodontal disease is designed to help dental professionals quantify both the extent of tissue destruction and the complexity of managing the condition. staging focuses on measurable damage, while grading takes into account factors that influence disease progression, such as patient age and risk factors. This system aids in clear communication, personalized patient care, and optimal disease management.
staging Periodontal Disease
The first step in this process is staging. staging classifies the severity and extent of the disease based on observable tissue destruction. There are four main stages:
stage 1: initial periodontitis
This stage is characterized by minor damage to the soft tissue and the supporting bone. At this point, bone loss is slight and often limited to the area around one or a few teeth. Pocket depths (the space between the tooth and gum) are usually shallow. Most patients may notice mild gum inflammation, but symptoms are often subtle.
stage 2: moderate periodontitis
In this stage, damage has progressed further. Bone loss is more noticeable and may affect multiple teeth. Pocket depths are greater, and loss of attachment between the tooth and the gum becomes more apparent. Patients may experience bleeding, gum recession, and early tooth mobility.
stage 3: severe periodontitis with potential for tooth loss
Stage 3 involves significant tissue destruction. There is extensive bone loss, and teeth may become loose or shift from their original position. Deep pockets are present, and tooth loss is likely if the disease is left untreated. This stage typically affects a large number of teeth and may alter how the teeth fit together.
stage 4: advanced periodontitis
This is the most severe stage. Patients with stage 4 periodontitis have experienced major bone and tissue destruction, and multiple teeth are at risk of loss or have already been lost. The ability to chew and function normally may be compromised. Oral hygiene becomes difficult, and the risk of further complications is very high.
Assessing Extent and Distribution
After determining the stage, it is important to assess the extent and distribution of the disease. This is categorized as:
- localized: Less than 30% of teeth involved
- generalized: More than 30% of teeth involved
This classification helps dentists understand the spread of the disease and plan for appropriate treatment.
grading Periodontal Disease
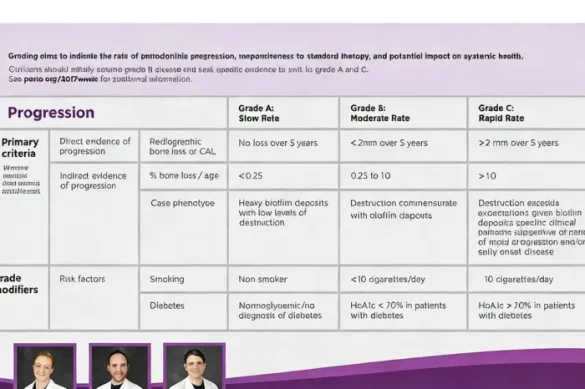
While staging measures the current severity, grading evaluates how quickly the disease is likely to progress in the future. grading is based on several criteria, including the rate of bone loss compared to the patient’s age, the presence of risk factors, and radiographic evidence. There are three grades:
grade a: slow disease progression
Patients in grade A tend to have a slow rate of bone and tissue destruction. Typically, this occurs in older individuals or in those with heavy plaque deposits but minimal tissue loss. These cases often show minimal disease progression over time.
grade b: moderate disease progression
Grade B represents cases where disease destruction and bone loss are moderate compared to the patient’s age and general health. Most patients with periodontitis fall into this category, and the risk of progression is average.
grade c: rapid disease progression
This grade is assigned to patients who show a high rate of tissue destruction relative to their age. Rapid progression may be seen in younger individuals or in cases with minimal plaque but significant tissue damage. These patients require more aggressive management and close monitoring.
Factors Influencing Grade
Beyond observable clinical signs, grading is also influenced by specific risk factors. These include:
- Smoking
- Diabetes
- Genetic predisposition
- Ineffective oral hygiene
These factors can increase or decrease the likelihood of rapid disease progression. For example, smokers and people with uncontrolled diabetes are more likely to fall into grade C and require additional interventions.
The Importance of radiographic assessment
Dentists use radiographs (dental X-rays) taken over time to assess the progression of periodontal disease accurately. Comparing images allows them to evaluate changes in bone levels, which is crucial for determining both the stage and grade of the disease. Radiographs provide objective evidence of disease progression and help guide treatment decisions.
Patient-Centered Care and Communication
The staging and grading system allows dental professionals to tailor treatment plans for each patient. By understanding individual risk factors and disease severity, dentists can explain the situation clearly to patients, discuss preventive strategies, and address modifiable risks like smoking and diabetes. This approach ensures more effective and long-lasting outcomes.
Practical Steps for Dental Professionals
- Conduct a thorough examination, including probing pocket depths and assessing attachment loss.
- Collect patient history, including risk factors like smoking, diabetes, and oral hygiene habits.
- Take diagnostic radiographs for baseline and follow-up comparison.
- Assign a stage based on observed tissue destruction.
- Assess extent (localized or generalized disease involvement).
- Assign a grade based on risk factors, progression evidence, and radiographic findings.
- Develop a personalized treatment plan and communicate it clearly to the patient.
Conclusion
staging and grading periodontal disease are critical steps in precise diagnosis, personalized treatment planning, and ongoing management. By following a systematic approach that considers both the severity and risk of progression, dental professionals can optimize outcomes and help patients maintain healthy teeth and gums for a lifetime. Understanding the importance of proper assessment helps patients take an active role in their oral health.
Frequently Asked Questions
What is periodontal disease?
Periodontal disease is an infection of the gums and tissue supporting the teeth, often caused by bacteria in dental plaque.
How do dentists stage periodontal disease?
Dentists assess the amount of tissue and bone destruction, distribute the disease as localized or generalized, and assign a stage ranging from 1 to 4.
What are the main risk factors for rapid disease progression?
Smoking, diabetes, poor oral hygiene, and genetics are major factors influencing rapid progression.
Why is grading important?
grading helps predict how quickly the disease may get worse and shapes the treatment plan accordingly.
Can periodontal disease be prevented?
Yes, good oral hygiene, regular dental check-ups, and managing risk factors significantly reduce the risk of developing advanced periodontal disease.