INTRODUCTION
Clinical procedures concerning the need for posts and the protocol for core buildups in endodontically treated teeth have evolved significantly over the last few decades with the advent of dentin bonding protocols. Likewise, the dental literature has evolved yet is fraught with contradictions. However, the consensus in the literature today is that posts weaken teeth, and when adequate tooth volume is present, a post is contraindicated, and only a core buildup should be done.
There is a misconception often quoted in the literature that the reason a post is needed is to retain the core buildup. Perhaps this was true before adequate dentin bonding protocols existed, but this is simply no longer true. Posts cannot retain a buildup because the post itself is retained by the cement and buildup. Posts have no inherent retention. The only reason to place a post is to avoid horizontal fracture of the core buildup. In addition, many authors subscribe to the necessity of the ferrule effect, while others debunk the idea. Many clinical studies on the ferrule effect are simply studying residual tooth structure volume rather than any effect ferrules may have. Clinical decisions on how to best restore endodontically treated teeth must be made with a jaundiced eye toward the literature since there are so many contradictions in the “evidenced-based” literature.
Much of the conflict in the endodontic literature on post placement stems from the clinical protocols used in the studies. Any study done using paper points to dry a canal where dentin bonding is used is flawed because paper points simply will not sufficiently dry a canal for dentin bonding to work. Studies done with acid-based cements that do not bond to the unique post space dentin and the post are also flawed. Likewise, the use of dual-cured resins to place posts results in a flawed study since complete conversion requires light activation, and light will not penetrate to the depth of a post space.
Therefore, a clinician is left to decide on how to restore an endodontically treated tooth based on observable “facts” within their own practices. Those observations over decades with teeth they have restored and followed will lead the clinician to prudent management. I have been fortunate to have observed these “facts” for more than 5 decades. My first lecture was in 1972 to our local dental society on how to fabricate and place a gold post. Since that time, I have restored thousands of endodontically treated teeth out of the more than 65,000 units I have placed and have been fortunate to practice in the same community for more than 50 years. I have followed the outcome of what I did for my patients on the majority of those 65,000 units. As materials and my experience evolved, so did my clinical protocols on how best to restore endodontically treated teeth.
Here are the thoughts I have on restoring endodontically treated teeth today in the 21st century based on my clinical experience for more than 5 decades and a belief in shards of uncompromised dental literature:
1. Properly restored teeth are better than implants. Implants are considered the route of last resort in our office. Well-done endodontic treatment, coupled with appropriate restorative procedures, can preserve teeth for decades.
2. Posts should not be placed when there is no need since the placement of a post weakens teeth and is fraught with complications both from the endo-
dontic fill and biomechanical perspectives.
3. Active screw posts should never be used because they split teeth.
4. Acid-soluble cements should never be used to place posts. The function of the cement is to retain the post. Acid-base cements are too weak to do that.
5. Glass ionomer cemented posts do not resist the formation of decay along the post space.
6. The need for a post is not to retain the core but rather to prevent horizontal fracture of the core buildup. There is no other need for a post.
7. Posts are not indicated for teeth that are not planned for full-coverage restorations.
8. Posterior endodontically treated teeth require cusp-coverage restorations. Simple direct composites as definitive restorations are inadequate for the long-term success of endodontically treated teeth.
9. Metal posts resist fracture of the core better than plastic or ceramic ones, which are prone to fracture.
10. Post spaces should never be initially prepared with end-cutting drills. Root perforation is common when this is done. Initial prep to depth (anything less than 10.0 mm is almost worthless) should be done with Peeso reamers or Gates Glidden drills, followed by sizing the post space with the end-cutting drill.
11. Post spaces can only be properly rinsed and dried with a Stropko Irrigator (Stropko). Paper point drying a canal to evaporate alcohol or acetone in primers simply will not take the substrate to the hydrophobic level necessary for successful bonding.
12. Teeth with core buildups that have adequate dimensions to resist fracture do not need posts. Molar teeth with posts result in many catastrophic failures.
13. Core buildups should always be separate from the crown. Casting, pressing, or milling the core as part of the crown is a significant compromise.
14. The primary cause of failure on teeth restored with posts is root fracture, which is secondary to the cement’s failure to retain the post. Once the post is loose, any occlusal force will likely stress the fragile root enough to fracture it.
15. The secondary cause of failure on teeth restored with posts is coronal microleakage down the post space, resulting in failure of the endodontic fill.
16. Endodontically treated teeth become brittle over time and, additionally, are usually biomechanically compromised. Appropriate distribution of occlusal forces on endodontically treated and restored teeth is critical for long-term success.
17. Posts should be embedded in the core buildup as much as possible since the opacity of the buildup will block the appearance of the metal post, and if it is centered in the buildup, it will increase the fracture resistance of the buildup.
18. Titanium posts do not rust like stainless steel. Rust compromises cosmetics. Flexure of the core buildup causes fracture of the buildup and, frequently, the roots. Plastic posts flex and often break because they do not resist fracture of the core buildup. Ceramic posts do not flex but fracture easily.
19. Titanium ParaPosts XP (Coltene) smaller than 4.5 are flexible and should be used with caution. Titanium alloy is more flexible than stainless steel, but that flexibility is clinically insignificant.
20. Only chemically activated composite cement should be used to cement posts. Dual-cure cement requires light to fully cure, and light will not penetrate to the base of the post space where a complete cure is mandatory.
21. Molars almost never need posts since the volume of core material will not need to be reinforced to prevent fracture.
22. Bicuspids rarely need posts unless they are fractured off at the tissue level.
23. Most posts “succeed” because there was never a need to place one initially. This is one of the confusing aspects of retrospective studies on posts.
24. There are cases where heroics can keep a tooth for quite some time, but when the volume of tooth structure is severely compromised, the prognosis is poor, and the outcome eventually will be failure.
25. It is prudent to attempt heroics when the age of the patient is factored into the treatment plan. Elderly patients may well benefit from a decade or so of service out of a heroic attempt to keep a tooth. Likewise, younger patients may benefit from keeping a tooth for a decade or so as the knowledge and prognosis of implant management grows at an exponential rate. Who knows, but what stem cell may grow a new tooth in the next decade or so?
26. Placing a post or core buildup requires a precise protocol to ensure decades of success. Protocols that we use for core buildups and post placement are free to download at our website,
struppbrummseminars.com. Click on “Protocol Downloads” to access them. These protocols are bulletproof, if followed precisely. In addition, our products list is also free to download. It contains all the products we use and a contact source to get them.
Two cases are presented here with captions to explain what was done. In addition, other photos are included to expand on certain aspects that require clarification. If you have any questions about this article, we will be happy to answer them on our Facebook page, Strupp/Brumm Dental Protocols, where more than 16,000 of the best dentists in the world gather to learn.
CASE REPORTS
Case 1: Teeth Nos. 6 to 11 necessitated replacement. These restorations were made with porcelain butt joints in the cosmetic zone and placed with zinc phosphate cement. Posts were placed with Fuji Glass Ionomer Cement (GC) in Nos. 7, 8, and 10 (Figure 1).

Case 2: Black discoloration along the labial porcelain butt joints was clinical evidence of decay. A 0.2 to 1.0 mm of recession over 30 years, coupled with the black discoloration along the margins, created a “cosmetic need” for the patient. The degree of pathology under the restorations was not clinically evident. Most restorations cemented with acid-soluble cement should be replaced after 2 to 3 decades, even if they “look” good (Figure 2).

After removing the old restorations, a significant amount of tooth structure was decayed because of the leaking restorations and dissolution of the acid-soluble cement. This was made worse by the patient’s habit of drinking acidic beverages. There was no bleeding tissue because a soft-tissue scrub with Pure 4% CHG (Best Buy Discount Dental Supply) was done 2 days before the preparations (Figure 3).

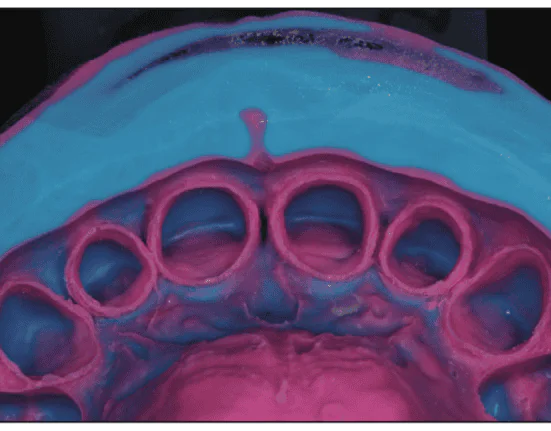
Case 3: Extensive loss of tooth volume occurred as the diseased tooth structure was removed. The glass ionomer cemented posts were removed using a sonic scaler. This exposed extensive decay along the post space walls, especially in the post space of No. 8. Because the projected volume of core buildup in No. 8 would satisfactorily resist horizontal fracture, a post was not indicated. Posts were indicated to resist horizontal fracture of the core buildups in Nos. 7 and 10, however, because the projected thin dimension of the core buildups were at risk for horizontal fracture without them (Figure 4).

Case 4: Our post placement protocol is the most critical protocol we use in advanced restorative cases, and the substrate to which we will bond must not be compromised. OpalDam Green (Ultradent Products) was used to cover the substrates and post spaces in Nos. 7 and 10 to prevent the products used in the core buildup protocol for Nos. 6, 8, 9, and 10 from touching the substrates and post spaces (Figure 5).

Case 5: Core buildups were done for Nos. 6, 8, 9, and 11. Excessive buildup material was placed to allow preparation of an ideal shape and form and to cover as many open tubules as possible in the vital teeth. Properly done core buildups on vital teeth are like immediate dentin sealing on steroids (Figure 6).

Case 6: Using the Strupp/Brumm protocol, 4.5 Titanium ParaPost XP (Coltene) posts were placed with the chemical cure cement PANAVIA 21 (Kuraray). The core buildups were placed simultaneously with post cementation so that both composites would set together. There is a dot after the 4 and before the T on the post. This indicates a size 4.5 and that the post is titanium alloy (Figure 7).

Case 7: Definitive preparations were done. We avoid touching the tissue as much as possible while creating an ideal shape and form to the abutments, which will accept the final lithium disilicate restorations. A single Sil-Trax Epi #00 retraction cord (Pascal) was soaked in Retrax AC (Pascal), blotted, placed, and immediately rinsed after placement on each tooth. Highly acidic hemostatic agents (which all hemostatic agents are) must immediately be rinsed to avoid severe damage to the abutments and necrosis of the tissue. Postoperative sensitivity usually results if these agents are not thoroughly rinsed immediately after use (Figure 8).

Case 8: The ideal shape to make a perfect chamfer margin is the Diamond Bur #6877K/014 (Brasseler), which has a 55° elliptical radius. The same shape in the Polaris Diamond is #G-62 (Figure 9).

Case 9: A definitive impression using Imprint 4 VPS (3M) was made that recorded unprepared tooth structure apical to the margin along with the entirety of the preps. We believe all margins recorded in an impression must include sound tooth structure apical to them to ensure a perfect fit of the final restoration (Figure 10).

Case 10: The cast from the first pour of the impression is used for dies. A second pour cast is made but not sawed. The second pour cast is used for checking proximal contacts on the final restorations after the soft-tissue zones are trimmed away from the margins to ensure a definitive seat of the final restorations (Figure 11).

Case 11: Provisional restorations that fit perfectly and are cemented with Durelon (3M) are critical for tissue health on the day of final cementation. Patients are seen one week post-op to ensure all provisional cement is removed and the patient is doing appropriate home care and for a scrub with Pure 4% CHG (Best Buy Discount Dental Supply). Controlling the microbiome during the provisional phase is critical for long-term success. Cementing into a pool of blood produces certain failure, and is a disservice to the patient (Figure 12).

Case 12: Durelon sticks to the teeth when the provisionals are removed. Its antimicrobial character keeps vital pulps vital and calm and minimizes the issue of cement sepsis (microbial growth under a restoration). Durelon is easily removed with a SONICflex (KaVo), which leaves black marks on the buildups. Painless anesthesia is always used for definitive cementation because we never want to hurt a patient during the placement process. Without anesthesia, the patient will never refer their friends because we hurt them (Figure 13).

Case 13: Air abrasion with CoJet Sand (3M) removes all of the black marks and residual Durelon. Air abrasion can open a capillary, but that is usually very easy to control by scrubbing the open capillary with Retrax AC, which must be thoroughly rinsed away to avoid compromising the resin cement and substrate to which we will bond (Figure 14).

Case 14: The cosmetic outcome is approved by the patient before definitive placement. Tissue health is mandatory for placement. A Pure 4% CHG scrub 2 days before placement minimizes bleeding, which is caused by a dysbiotic microbiome that invariably forms around margins on provisional restorations near the tissue. The second pour solid cast with the tissue trimmed away is used to confirm perfect interproximal contacts in the laboratory. Adjusting contacts clinically is a time suck and invariably results in loss of patient confidence (Figure 15).

Case 15: All of our patients are taught preventive dentistry techniques, and any bleeding tissue is scrubbed with Pure 4% CHG on a weekly basis until there is no bleeding due to aggressive brushing. This patient received preventive dentistry instructions, 3 scrubs with Pure 4% CHG, and a prophy. The microbiome present at the end of this protocol was symbiotic, and there was no bleeding tissue. The success of any clinical protocol depends on soft-tissue health before, during, and after the using the protocol. Posts or core buildups cannot successfully be done in a sea of blood, nor can cementation be successful in such conditions (Figure 16).

Case 16: The photos before core buildups/post placement and after crown placement were remarkable and were given to the patient. The anterior envelope of function was designed in the laboratory with the weak teeth in mind, and occlusal loading was placed where it could best be sustained by the available biology. Communication with the laboratory and precise placement protocols are critical in cases with weakened biology. The bonding protocols used for post placement and core buildups will make or break a case of this complexity, but they are meaningless unless the occlusal forces are properly distributed (Figure 17).