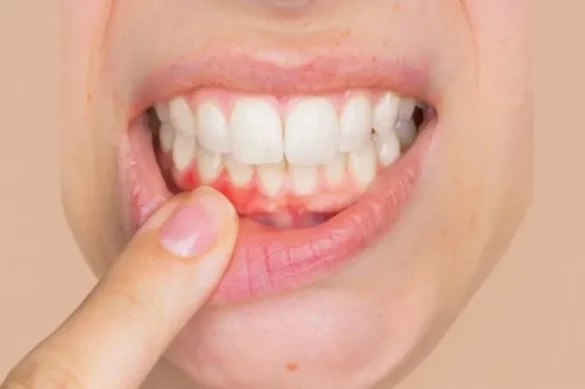
Gingivitis is a common form of gum disease that causes inflammation of the gums. It often starts as a mild irritation around the base of the teeth. If left untreated, gingivitis can progress into more severe forms of gum disease, such as periodontitis.
Understanding the factors that worsen gingivitis is essential for maintaining healthy gums and preventing tooth loss. Gingivitis is preventable and reversible in its early stages. Proper dental care and lifestyle choices play a crucial role in controlling it.
Poor Oral Hygiene
One of the main reasons gingivitis worsens is inadequate oral hygiene. When teeth are not brushed and flossed regularly, plaque builds up on the gum line. Plaque is a sticky film of bacteria that produces toxins. These toxins irritate the gums, causing redness, swelling, and bleeding. Brushing twice daily and flossing at least once a day can remove plaque and prevent gingivitis from worsening.
Incorrect Brushing Techniques
Even if you brush daily, using improper techniques can contribute to gingivitis. Brushing too hard can damage gum tissue, while brushing too lightly may not remove plaque effectively. Using a soft-bristled toothbrush and gentle circular motions is recommended. Electric toothbrushes can also improve plaque removal and help control gingivitis.
Neglecting Flossing
Flossing reaches areas between the teeth that a toothbrush cannot. Plaque accumulation in these areas can worsen gum inflammation. Skipping flossing regularly allows bacteria to thrive, which can intensify gingivitis symptoms. Daily flossing is crucial for gum health and preventing progression to periodontitis.
Diet and Nutritional Factors
What you eat also influences gingivitis. Diets high in sugar and refined carbohydrates increase the risk of plaque buildup.
Bacteria feed on sugar, producing acids that irritate gums and teeth. On the other hand, a diet lacking in essential nutrients, especially vitamin C, can weaken the immune system and reduce the gums’ ability to heal. Maintaining a balanced diet with fruits, vegetables, and whole grains can help gums stay healthy.
Vitamin Deficiencies
Vitamin C deficiency, also known as scurvy, can cause bleeding gums and worsen gingivitis. Other vitamins like vitamin D and B-complex also play a role in immune function and gum repair. Ensuring an adequate intake of these vitamins supports oral health and prevents inflammation from escalating.
Smoking and Tobacco Use
Smoking is a major risk factor for worsening gingivitis. Nicotine reduces blood flow to the gums, which slows down healing and immune response. Smokers are more likely to have severe gum inflammation, deep pockets between teeth and gums, and a higher risk of progressing to periodontitis. Quitting smoking significantly improves gum health and reduces gingivitis severity.
Medical Conditions
Certain medical conditions make gingivitis worse by affecting the immune system or blood circulation. These include diabetes, autoimmune diseases, and hormonal changes. Individuals with poorly controlled diabetes often experience more severe gum inflammation because their immune response is weakened. Autoimmune disorders can also increase susceptibility to infections, including gum infections.
Hormonal Changes
Hormonal fluctuations during pregnancy, menstruation, or menopause can make gums more sensitive and prone to inflammation. Pregnant women may develop “pregnancy gingivitis,” which can worsen if proper oral hygiene is not maintained. Regular dental check-ups during these periods are essential.
Medications
Some medications can worsen gingivitis by reducing saliva flow or causing gum enlargement. Dry mouth reduces the natural cleaning effect of saliva, allowing plaque to accumulate. Drugs such as certain antihypertensives, anticonvulsants, and immunosuppressants may cause gum overgrowth or inflammation. Discussing side effects with a dentist or doctor is important if gingivitis is present.
Stress and Immune System
Chronic stress can weaken the immune system and impair the body’s ability to fight bacterial infections, including those affecting the gums. Individuals under stress may also neglect oral hygiene habits, further increasing the risk of gingivitis worsening. Managing stress through exercise, relaxation techniques, and adequate sleep supports gum health.
Poorly Fitted Dental Appliances
Braces, dentures, and other dental appliances can worsen gingivitis if they are not fitted correctly or cleaned regularly. Food particles and plaque can accumulate around these devices, causing irritation and inflammation of the gums. Regular cleaning and dental check-ups help prevent gingivitis related to dental appliances.
Dry Mouth and Saliva Reduction
Saliva plays a critical role in neutralizing acids, washing away food debris, and controlling bacteria in the mouth. Conditions such as xerostomia (dry mouth) can accelerate plaque buildup and worsen gingivitis. Causes of dry mouth include dehydration, certain medications, and medical conditions like Sjögren’s syndrome. Staying hydrated and using saliva substitutes can help protect the gums.
Genetic Factors
Some individuals are genetically predisposed to gum disease. Family history can influence susceptibility to severe gingivitis or rapid progression to periodontitis. While genetics cannot be changed, careful oral care and frequent dental visits can help manage the risk and prevent worsening gum disease.
Age-Related Factors
As people age, gum tissue naturally recedes, and oral hygiene may become more challenging. Older adults may also have chronic conditions or medications that contribute to gingivitis. Maintaining routine dental care, including professional cleanings, is essential for preventing gingivitis from worsening with age.
Prevention and Control
Preventing gingivitis from worsening requires consistent oral care, lifestyle changes, and regular dental visits. Brushing twice daily, flossing, using antibacterial mouthwash, and maintaining a balanced diet are key preventive measures. Quitting smoking, managing medical conditions, and reducing stress also contribute to gum health. Early treatment of gingivitis is highly effective in reversing inflammation and preventing progression to periodontitis.
Regular Dental Check-Ups
Professional cleanings remove tartar that cannot be removed by brushing alone. Dentists can also detect early signs of worsening gingivitis and provide tailored treatment. Visiting the dentist every six months is recommended for most individuals, though those with gum disease may require more frequent visits.
Good Oral Hygiene Routine
Establishing and following a consistent oral hygiene routine is critical. This includes brushing for at least two minutes, flossing daily, and using mouthwash if recommended. Regular cleaning prevents plaque accumulation and reduces inflammation.
Conclusion
Gingivitis is a common and reversible gum disease, but it can worsen if risk factors are not addressed. Poor oral hygiene, diet, smoking, medical conditions, medications, stress, dry mouth, dental appliances, genetics, and aging all play a role in worsening gingivitis. Understanding these factors helps individuals take proactive steps to maintain healthy gums.
Consistent oral care, professional dental check-ups, lifestyle modifications, and early intervention are key to controlling gingivitis and preventing severe gum disease.