Canker ulcers, also called aphthous ulcers, are among the most common oral lesions seen in dental clinics. They affect children, adults, and older people. They often appear without warning. They can cause pain during eating, speaking, and brushing. They can reduce quality of life. They can also interfere with proper oral hygiene. When brushing becomes painful, plaque control becomes poor. This may increase the risk of gum disease over time.
Many patients believe canker ulcers are harmless. This belief is only partly true. Most canker ulcers heal on their own. However, recurrent or severe ulcers can signal nutritional deficiencies, immune imbalance, or mechanical trauma. Poor management may worsen discomfort. It may delay healing. It may also increase stress, which further slows recovery.
What Are Canker Ulcers?
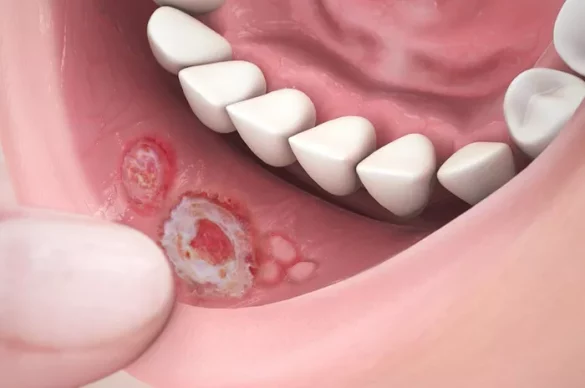
Canker ulcers are non-contagious sores that form inside the mouth. They usually develop on soft tissues. Common sites include the inner cheeks, lips, floor of the mouth, soft palate, and tongue. They do not appear on the outer lips. They are different from cold sores. Cold sores are caused by herpes viruses. Canker ulcers are not viral.
A typical canker ulcer has a round or oval shape. It has a white or yellow center. It has a red inflamed border. Pain often appears before the ulcer is visible. The pain may feel burning or tingling. Eating spicy or acidic foods often worsens discomfort.
Types of Canker Ulcers
There are three main types of canker ulcers.
Minor aphthous ulcers are the most common. They are small. They usually heal within 7 to 14 days. They do not leave scars.
Major aphthous ulcers are larger and deeper. They may last several weeks. They can cause significant pain. They may leave scars after healing.
Herpetiform ulcers are less common. They appear as clusters of many tiny ulcers. They may merge into larger lesions. Despite the name, they are not related to herpes infection.
Understanding the type of ulcer helps guide management. Minor ulcers often respond well to simple care. Major ulcers may require professional intervention.
Why Proper Treatment Matters
Ignoring canker ulcers is common. Many patients wait for them to disappear. This approach is not always ideal. Pain may worsen. Secondary irritation may occur. Poor oral hygiene may develop due to discomfort. This can increase plaque accumulation. Plaque is a major risk factor for gum disease.
When patients avoid brushing painful areas, bacteria multiply. Inflammation of the gums may follow. Bleeding may occur. Over time, untreated gingival inflammation may progress to periodontitis. This is why canker ulcer care should not be separated from overall oral health management.
5 Tips for Curing Canker Ulcers in 2026
Tip 1: Maintain Gentle but Consistent Oral Hygiene
Good oral hygiene is essential, even when ulcers hurt.
Many patients stop brushing near an ulcer. This is understandable. Pain discourages contact. However, avoiding brushing allows plaque and bacteria to accumulate. This can delay healing. It can also irritate surrounding tissues.
Choosing the Right Toothbrush
A soft-bristled toothbrush is essential. Hard bristles can cause mechanical trauma. Trauma is a known trigger for canker ulcers. Soft bristles reduce irritation. They also protect sensitive tissues.
Patients with Sensitive Teeth should be especially cautious. Aggressive brushing can worsen tooth sensitivity and oral sores at the same time.
Using the Correct Technique
Brush gently. Use small circular motions. Avoid scrubbing. Focus on cleaning, not force. If direct contact with the ulcer is painful, clean the surrounding area carefully. Do not skip entire sections of the mouth.
Mouth Rinsing Practices
Rinsing helps reduce bacterial load. Use alcohol-free mouth rinses. Alcohol can dry tissues. Dryness delays healing. Saltwater rinses are simple and effective. Salt helps reduce inflammation. It also cleans the area.
Maintaining oral hygiene supports healing. It reduces the risk of secondary infection. It also protects against gum disease during painful episodes.
Tip 2: Modify Diet to Reduce Irritation and Support Healing
Food choices directly affect ulcer pain and recovery.
Certain foods irritate ulcers. Others support tissue repair. Dietary modification is a core strategy in canker ulcer management.
Foods to Avoid
Spicy foods increase pain. Acidic foods irritate tissues. Citrus fruits, tomatoes, and vinegar should be limited. Hard or sharp foods can cause mechanical trauma. Chips and crusty bread may scrape the ulcer surface.
Sugary foods increase bacterial growth. This may worsen inflammation. Excess sugar also contributes to plaque formation. This is relevant for patients concerned about gum disease.
Foods That Promote Healing
Soft foods are easier to tolerate. Yogurt, mashed vegetables, and soups are good options. Foods rich in vitamins and minerals support tissue repair. Vitamin B complex, iron, zinc, and folate are particularly important.
Protein supports cell regeneration. Lean meats, eggs, and legumes are helpful. Adequate hydration keeps tissues moist. Moist tissues heal faster.
Addressing Nutritional Deficiencies
Recurrent canker ulcers may be linked to deficiencies. Low levels of iron, vitamin B12, or folic acid are common triggers. A balanced diet reduces recurrence risk. In some cases, supplementation may be recommended by healthcare providers.
Tip 3: Use Evidence-Based Topical Treatments
Topical therapy targets pain and inflammation directly.
Topical agents are widely used for canker ulcers. They provide localized relief. They protect the ulcer surface. They may speed healing.
Protective Pastes and Gels
Barrier pastes form a protective layer. They reduce irritation from food and teeth. They help ulcers heal undisturbed. These products are especially useful during meals.
Anti-Inflammatory Agents
Some topical treatments reduce inflammation. They may contain corticosteroids. These are usually prescribed for severe ulcers. They reduce immune-mediated tissue damage. Proper use is important. Overuse may cause side effects.
Antimicrobial Mouth Rinses
Antimicrobial rinses reduce bacterial load. This lowers infection risk. They are useful when oral hygiene is compromised by pain. Alcohol-free formulations are preferred.
Topical treatment should be chosen carefully. It should match ulcer severity. Professional guidance is advised for recurrent or severe cases.
Tip 4: Manage Underlying Triggers and Risk Factors
Canker ulcers often have identifiable triggers.
Treating the ulcer alone is not enough. Preventing recurrence requires addressing underlying causes.
Mechanical Trauma
Biting the cheek is a common cause. Sharp tooth edges and broken fillings also cause trauma. Orthodontic appliances may irritate soft tissues. Dental evaluation is important. Smoothing sharp edges reduces recurrence.
Stress and Immune Response
Stress affects immune balance. Many patients report ulcers during stressful periods. Sleep deprivation and anxiety may contribute. Stress management supports overall health. It also reduces ulcer frequency.
Oral Care Products
Some toothpaste ingredients may trigger ulcers. Sodium lauryl sulfate is a known irritant for some individuals. Switching to milder formulations may help. This change also benefits patients with Sensitive Teeth.
Systemic Health Conditions
Recurrent ulcers may be associated with systemic conditions. Examples include gastrointestinal disorders and immune diseases. Persistent ulcers require medical evaluation. Early diagnosis improves outcomes.
Tip 5: Know When to Seek Professional Dental Care
Most ulcers heal within two weeks. Some do not. Professional assessment is essential in certain cases.
Warning Signs
Ulcers lasting longer than two weeks require evaluation. Severe pain that interferes with eating is concerning. Large ulcers or frequent recurrences should not be ignored. Fever or systemic symptoms require prompt attention.
Differential Diagnosis
Not all oral ulcers are canker ulcers. Traumatic ulcers, infections, and oral cancer may appear similar. Dental professionals are trained to distinguish these conditions. Early detection saves lives.
Comprehensive Oral Health Assessment
Dental visits allow full oral examination. Gum health is evaluated. Plaque and calculus are removed. This reduces inflammation. It also lowers the risk of gum disease during ulcer episodes.
Relationship Between Canker Ulcers, Sensitive Teeth, and Gum
DiseasePain from ulcers may lead to altered brushing habits. Inadequate cleaning increases plaque. Plaque irritates gums. Gum inflammation worsens oral discomfort. This creates a cycle.
Patients with Sensitive Teeth may already brush cautiously. The addition of ulcers may further reduce cleaning effectiveness. Education is essential. Proper techniques allow cleaning without pain.
Managing canker ulcers supports overall oral health. It protects gums. It helps maintain comfort during daily hygiene routines.
Prevention Strategies for Long-Term Control
Prevention reduces suffering and recurrence.
Preventive measures are often simple. They are based on awareness and consistency.
Regular Dental Checkups
Routine visits allow early detection of issues. Sharp edges are corrected. Oral hygiene is reinforced. Professional cleaning reduces bacterial load.
Balanced Lifestyle
Adequate sleep supports immune health. Balanced nutrition prevents deficiencies. Stress management reduces flare-ups.
Personalized Oral Care Routine
Choose products suited to individual needs. Mild toothpaste benefits sensitive tissues. Soft brushes reduce trauma. Consistency is key.
Conclusion
They may be common. They may be small. Their impact is significant. Pain affects daily life. Poor management affects oral health. This article presented five practical tips. Gentle oral hygiene protects healing tissues. Dietary modification reduces irritation. Evidence-based topical treatments control pain. Trigger management prevents recurrence. Professional care ensures safety. Caring for canker ulcers is part of comprehensive dental care. It supports comfort. It protects against gum disease. It helps patients maintain healthy routines, even with Sensitive Teeth.