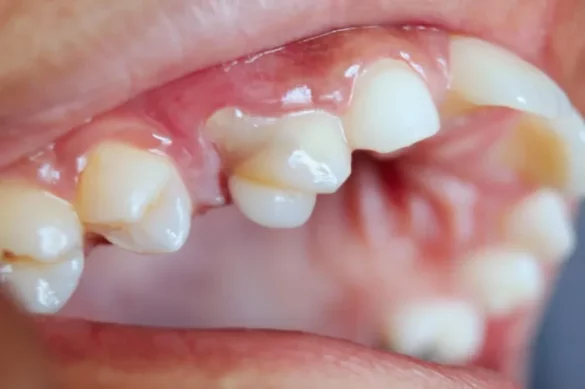
Tooth decay is a problem that many people experience during their lives. While occasional cavities are common, some people notice that their teeth seem to decay much faster than expected. Rapid tooth decay can have serious consequences, including pain, infection, and even tooth loss. It is important to know that certain diseases can make your teeth decay faster. Understanding these medical conditions can help you take better care of your smile and prevent further problems.
What Is Rapid Tooth Decay?
Rapid tooth decay means that teeth are damaged quickly over a short time. Normal decay happens gradually, but rapid decay means cavities form or worsen much faster than usual. This process can be alarming and may signal an underlying health problem. Recognizing rapid tooth decay and finding the cause is an important step for good oral health.
How Does Tooth Decay Happen?
Tooth decay begins when bacteria in the mouth break down sugars and produce acids. These acids can erode the outer layer of your teeth, called enamel. Over time, acid can make small holes, or cavities, in your teeth. If not treated, decay can spread deeper, causing larger cavities or even infecting the tooth’s nerve. While poor oral hygiene and a sugary diet are common causes, some diseases can make this process happen much faster.
Medical Conditions That Cause Rapid Tooth Decay
Certain diseases can change the way your mouth works, leading to rapid decay. Here are some of the main illnesses known to accelerate tooth decay:
Diabetes
Diabetes affects your whole body, including your mouth. High blood sugar levels in people with uncontrolled diabetes can help bacteria grow quickly. Bacteria use sugar as food and turn it into acids that damage teeth. Diabetes can also reduce saliva production. Saliva is important because it helps wash away food and bacteria. Without enough saliva, your mouth becomes dry and more likely to develop cavities. People with diabetes are also at higher risk for gum disease, which can make tooth decay worse.
Sjogren’s Syndrome
Sjogren’s syndrome is an autoimmune disease where the body attacks its own moisture-producing glands. This includes the salivary glands in your mouth. A dry mouth is one of the main symptoms of Sjogren’s syndrome. Without enough saliva, acids stay on your teeth longer and bacteria can thrive. This creates the perfect conditions for rapid tooth decay. People with Sjogren’s syndrome often have trouble swallowing and may sense a constant dryness in their mouth.
Xerostomia (Dry Mouth)
Xerostomia is another name for dry mouth. Sometimes it is not caused by a disease but by certain medications or by dehydration. Many drugs for allergies, high blood pressure, depression, and other illnesses can reduce saliva flow. With less saliva, your mouth cannot neutralize acids or clean away food as easily. This leads to more rapid decay. People who experience frequent dry mouth may notice sticky saliva, trouble speaking or swallowing, and bad breath.
Eating Disorders
Eating disorders, such as bulimia and anorexia, can cause significant damage to teeth. Bulimia involves repeated vomiting. Stomach acids from vomiting can wear away tooth enamel very quickly. Anorexia can lead to poor nutrition, which weakens teeth and makes them more prone to cavities. Both conditions can decrease saliva production, which adds to the risk. People with eating disorders may also avoid certain foods, missing out on vitamins and minerals important for strong teeth.
Gastroesophageal Reflux Disease (GERD)
GERD is sometimes called acid reflux. It happens when stomach acid comes up into the mouth. When teeth are often exposed to stomach acid, the enamel can erode, leading to rapid decay. The process is even faster if vomiting is frequent, as in cases of persistent reflux. Symptoms of GERD include frequent heartburn, sour taste in the mouth, and chest discomfort.
Weak Immune System
A weak immune system can make it easier for harmful bacteria to grow in the mouth. Conditions such as HIV/AIDS or treatments like chemotherapy can weaken the body’s defenses. This increases the risk of oral infections, gum disease, and rapid tooth decay. Autoimmune diseases such as lupus can also affect the mouth and reduce the body’s ability to fight infection.
Additional Factors That Make Tooth Decay Worse
Underlying diseases are not the only cause. Some related factors can hasten decay when these conditions are present:
Medications
Many drugs, especially those for allergies, depression, and heart diseases, can reduce saliva production. This side effect can lead to chronic dry mouth, making teeth more vulnerable to rapid decay.
Malnutrition
Illnesses that affect how your body uses food or that lead to poor nutrition can weaken teeth. Lack of vitamins and minerals like calcium and vitamin D makes tooth enamel less strong.
High-Carbohydrate Diets
People with certain diseases may eat more carbohydrates. Carbohydrates break into sugars in the mouth, feeding bacteria and speeding up decay.
Acidic Foods and Drinks
Acidic foods and drinks can wear away tooth enamel if consumed often. This is a bigger problem for people whose saliva production is already low due to disease or medication.
Signs of Rapid Tooth Decay
You should look for:
- Increased sensitivity to hot or cold
- Pain when eating sweet foods
- Visible black, brown, or white spots on teeth
- Rough spots or holes in your teeth
- Persistent bad breath
Rapid tooth decay may also cause swelling, redness, or sores in the mouth. If you notice these signs, especially with known medical conditions, see a dentist promptly.
How to Reduce the Risk
Early action is very important. Here are some ways to protect your teeth if you have one of the diseases mentioned:
- Brush teeth at least twice daily with fluoride toothpaste, and floss once a day.
- Visit your dentist regularly—at least every six months or as advised.
- Inform your dentist about any diagnosed health conditions and all medications you take.
- Drink plenty of water to keep your mouth moist and wash away food particles.
- Ask your dentist about products for dry mouth, such as artificial saliva or sugar-free chewing gum.
- Work with your doctor to manage underlying health conditions. Controlling blood sugar, for example, helps protect your teeth.
- Avoid tobacco, limit sugary snacks and acidic drinks, and eat a balanced diet with plenty of fruits and vegetables.
When To See Your Dentist Or Doctor
If you already have a condition like diabetes, Sjogren’s syndrome, or another illness discussed, schedule regular checkups with both your doctor and dentist. Early detection of dental problems can prevent the need for more complex and costly treatment later. Managing your underlying condition is a key step toward healthier teeth.
Conclusion
Rapid tooth decay happens faster than normal and can lead to serious dental problems. While poor oral hygiene and diet play major roles, many medical diseases—such as diabetes, dry mouth from various causes, eating disorders, GERD, and weakened immunity—can speed up the process. By understanding which diseases cause rapid decay and taking steps to protect your oral health, you can minimize damage and keep your smile healthy longer. If you notice changes or have underlying health conditions, speak with your dentist and physician promptly.
Frequently Asked Questions (FAQs)
What is the most common disease that causes rapid tooth decay?
Diabetes is one of the most common systemic diseases linked to rapid tooth decay, as it affects both saliva production and the body’s ability to fight infection.
How do I know if my tooth decay is caused by a medical condition?
If you notice rapid changes, new dry mouth, or decay despite good oral hygiene, talk to your dentist and physician. Blood tests and other evaluations may reveal an underlying disease.
Can rapid tooth decay be stopped?
In many cases, yes. Treating the underlying disease, improving oral hygiene, and following your dentist’s advice can slow or stop further tooth decay.
Should my dentist know about my other medical conditions?
Absolutely. Share all your medical history and a list of medications with your dentist during every visit. This helps create the best plan for your oral health.