Periodontal disease, also called gum disease, is a common oral health problem that affects the tissues supporting your teeth. Early identification is critical because gum disease can progress painlessly, causing serious damage before you notice clear symptoms. Dentists use a systematic approach to detect periodontal disease, combining clinical expertise with specialized tools to ensure early and accurate diagnosis.
Understanding Periodontal Disease
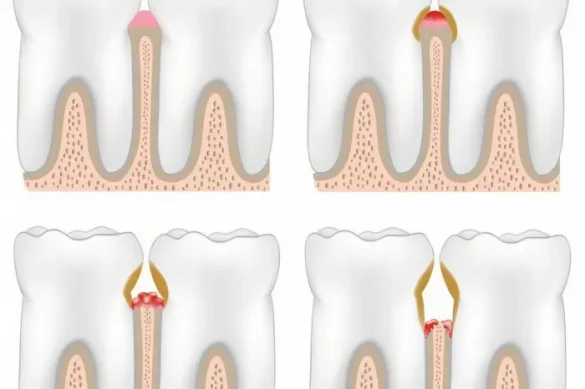
Periodontal disease refers to inflammation and infection in the gums and supporting bone around teeth. Poor oral hygiene is a primary cause, but genetics, lifestyle habits, and underlying health conditions can also increase risk. The disease usually advances through several stages — from gingivitis (mild gum irritation) to moderate and severe periodontitis, which can result in tooth loss and affect overall well-being.
Why Early Detection Is Important
Many people with gum disease do not experience pain, especially in the early stages. Because gum disease can silently destroy gum and bone tissue, early detection enables less invasive treatments and a higher chance for reversal, particularly during the gingivitis stage. Managing periodontal disease early also reduces risks for complications in general health, including links with heart disease, diabetes, and stroke.
Symptoms Dentists Look For
During routine dental checkups, dentists first ask about any changes or symptoms you may have noticed, such as bleeding gums, bad breath, gum tenderness, or problems with chewing. Some common warning signs they evaluate include:
- Swollen, red, or purplish gums
- Gums that bleed when brushing or flossing
- Receding gums (pulling away from teeth)
- Loose teeth
- Changes in the way your teeth fit together
- Persistent bad breath
Not everyone will develop noticeable symptoms, so relying on regular professional examinations is essential.
The Process: How Dentists Check for Periodontal Disease
Visual Oral Examination
Dentists begin by visually inspecting your mouth. They check the color, shape, and texture of your gums. Healthy gums appear pink and firm, while diseased gums may look swollen, shiny, or bleed easily. Dentists also look for signs of pus, plaque buildup, or gum recession aroud the teeth.
Measuring Gum Pockets: Periodontal Probing
A key step in diagnosis is periodontal probing. Dentists use a small, graduated instrument called a periodontal probe. They gently place this probe between your teeth and gums to measure the depth of the space, or ‘pocket,’ around each tooth. Healthy gums usually have pocket depths of 1 to 3 millimeters. Deeper pockets suggest infection and loss of supporting tissue:
- 1–3mm: Healthy
- 4–5mm: Early to moderate gum disease
- Above 5mm: Advanced gum disease
The deeper the pocket, the more severe the periodontal issue. Probing is painless and helps track the disease’s progression over time.
Evaluating Gum Recession and Tooth Mobility
Dentists also examine whether your gums are receding (pulling away from teeth) and whether any teeth feel loose. Recession and looseness often signal long-term tissue or bone loss. By gently moving your teeth or measuring the length of exposed tooth surfaces, dentists can assess the extent of the problem.
Assessing Bite and Jaw Alignment
Any changes in the way your teeth come together or your bite feel can indicate bone loss or shifting teeth caused by gum disease. Dentists may ask you to bite down or check your jaw’s alignment to spot these subtle signs.
Dental X-rays: Looking Beneath the Surface
To get a detailed view of the bone supporting your teeth, dentists routinely take dental X-rays. These images help identify areas where the bone has been lost under the gum line, which is not visible to the naked eye. Comparing current X-rays to previous ones allows dentists to detect progressive bone loss and plan appropriate treatments.
Reviewing Your Health and Lifestyle Factors
Accurate diagnosis also involves discussing your medical history and lifestyle habits. Dentists may ask about:
- Past gum disease experience
- Smoking or tobacco use
- Diabetes or autoimmune disorders
- Family history of gum disease
- Medications affecting gum health
This assessment provides context for risk and helps customize prevention and treatment plans.
When Dentists Refer to Periodontists
If a dentist suspects advanced periodontal disease or identifies complex gum problems, they may refer you to a periodontist — a gum specialist. Periodontists are equipped to handle deep cleanings, surgical procedures, and advanced regenerative treatments to stabilize the disease.
Follow-Up and Monitoring
Once an examination is complete, your dentist will share their findings and explain any areas of concern. They may recommend regular cleanings, improved oral hygiene, or more specialized treatments based on the severity of the disease. Follow-up appointments and periodic re-evaluation help monitor the effectiveness of treatment and prevent recurrence.
Conclusion
Checking for periodontal disease is a structured and proactive process. Dentists combine visual inspection, gentle probing, and advanced imaging to accurately diagnose gum disease in its earliest stages. Regular dental visits, combined with excellent oral hygiene, can significantly reduce your risk of developing severe periodontal disease and protect both your oral and overall health.
Frequently Asked Questions (FAQs)
What should I expect during a periodontal exam?
You can expect a gentle but thorough check of your gums, probing to measure pocket depths, and dental X-rays. Your dentist will also ask about any symptoms or risk factors.
How often should I have my gums checked for periodontal disease?
Routine dental exams every six months are recommended. If you are at higher risk or have been diagnosed before, your dentist may suggest more frequent visits.
Is probing painful?
No, probing is a simple, mostly painless procedure. Any discomfort is mild and brief.
Can periodontal disease be reversed?
Early-stage gum disease (gingivitis) can be reversed with professional cleanings and good oral hygiene. More advanced stages can be managed but usually not fully reversed.
Why are dental X-rays important for diagnosing periodontal disease?
X-rays help your dentist see bone loss that cannot be detected by looking or probing alone. They are critical for accurate diagnosis and treatment planning.