Diagnostics is the ultimate key to success for any treatment, and it can be particularly challenging in clinical situations that require a great deal of information in order to put the puzzle together. In this article, we will focus on three such clinical situations and present a rare case of mastocytosis, cases of lesions related to bisphosphonate treatment and a case of a traumatic bone lesion. Of course, anamnesis is the starting point of any diagnosis, but patients’ information in cases of traumatic lesions is extremely important because these lesions can be slow to develop and date back several years—even 20 years.
Mastocytosis bone lesion
Systemic mastocytosis is a rare disorder that results in abnormal proliferation of mast cells. Signs and symptoms of systemic mastocytosis depend on the part of the body affected. Bone involvement is the most common and significant imaging finding in patients with systemic mastocytosis and is a prognostic indicator because it may reflect a more aggressive disease course. When interpreted in conjunction with clinical features, skeletal imaging can raise suspicion of systemic mastocytosis.
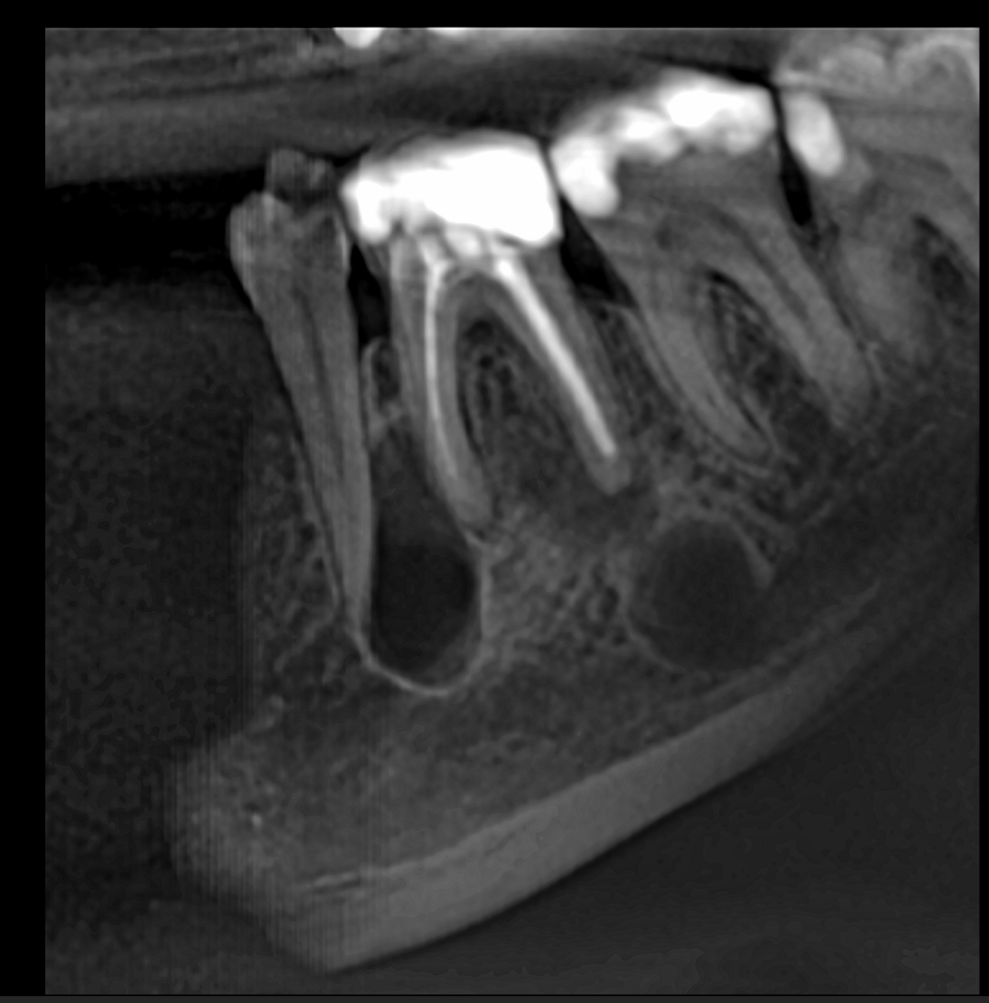
Fig. 1: 2D image generated from the DEXIS OP 3D scan, showing multiple bone lesions.
The patient in this case requested a second opinion on a molar that was causing him some discomfort, for which his dentist had recommended extraction and referred him to a dental surgeon. The radiograph did not show normal bone density or a typical periapical lesion. When asked about his health and medical history, the patient reported that he had an autoimmune condition, mastocytosis.
The patient was asked to search for a centre in his area with the DEXIS OP 3D unit, which provides high-quality images, and to request a 5 × 5 scan in endodontic mode, because it has the highest level of detail. A 2D view was generated from the scan to obtain a preview of the situation (Fig. 1). This showed a large lesion at the level of the mesial root between the molar and the premolar, a smaller lesion under the distal root, a minor lesion at the apex of the mesial root and a large lesion under the distal root at the lower level of the mandible. The question was whether this was one lesion or multiple lesions and one pathology or several.
The scan was then analysed using DTX Studio Clinic (DEXIS; Fig. 2). It fully supports importing and viewing of any DICOM file and can be used for 2D radiographs and intra-oral photographs. The platform integrates multiple artificial intelligence tools in 2D and 3D workflows, boasting several innovative features. One of its most useful features is that the software processes the image in order to produce the best quality to support the clinician in accurate diagnosis.
After adjusting the horizontal and vertical axes according to the axis of the distal root, we could see clearly that the lower bone lesions were well defined (Fig. 3). The clear separation between the lesions, which was evident in the coronal and sagittal views, indicated that they were two different pathologies. The periodontal ligament of the mesial root was present and uninterrupted, marking the separation between the lesion located between the molar and premolar and the mesial root of the molar (Figs. 4a–d & 5). This again confirmed a clinical situation with two kinds of pathologies. The large bone lesions were due to the mastocytosis, and the apical infection of the roots was due to failed root canal treatment.
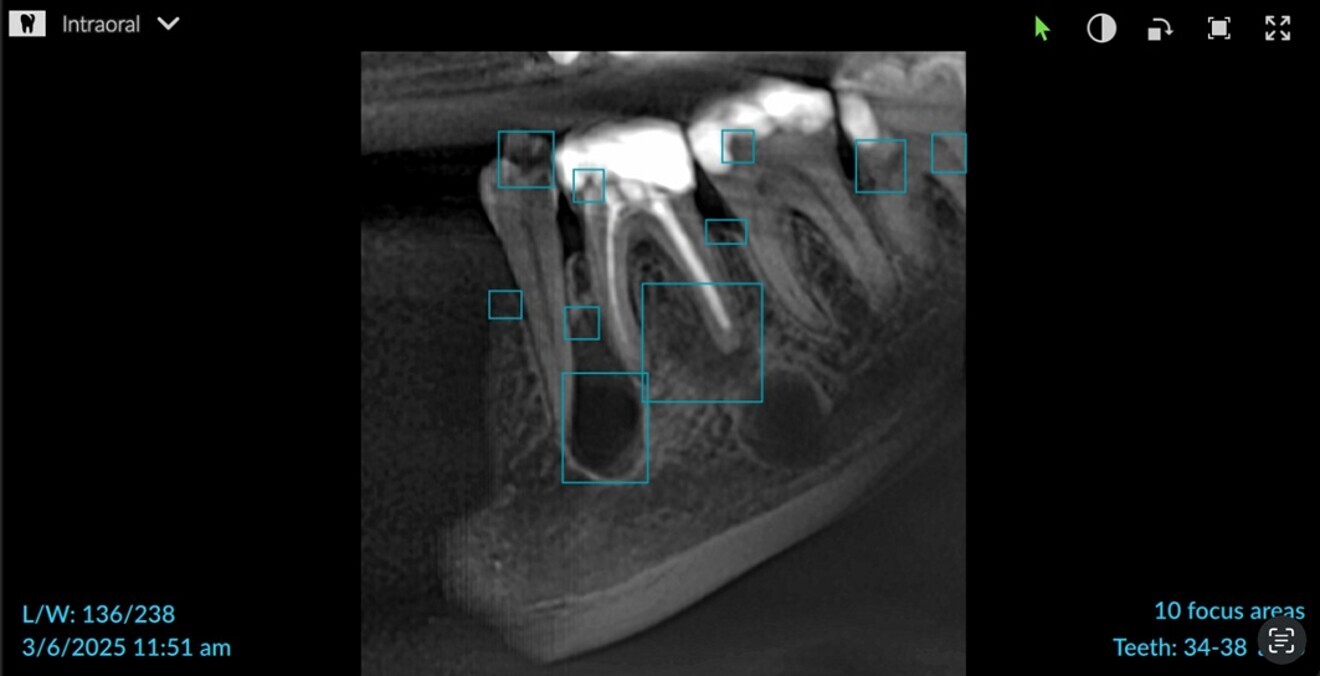
Fig. 2: Application of artificial intelligence to the 2D radiograph to focus on multiple areas in DTX Studio Clinic.
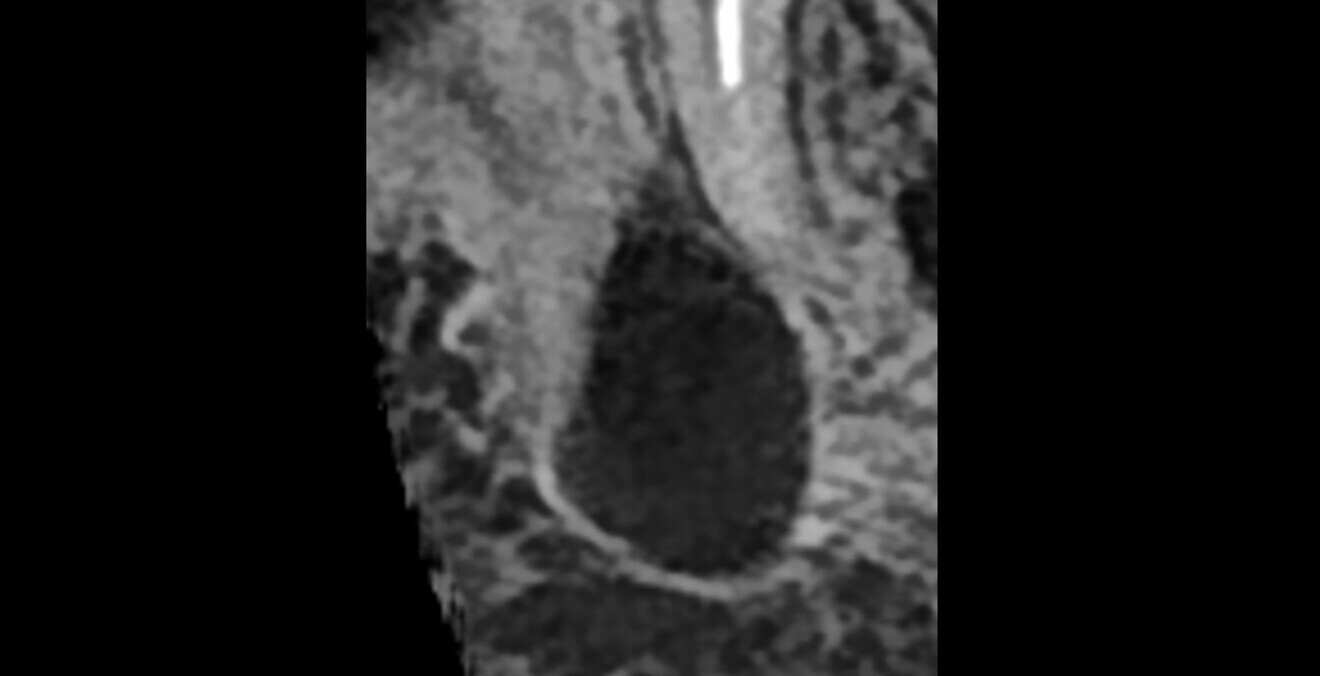
Fig. 3: Clear separation between the two lesions in the analysis of the 2D image generated from the DEXIS OP 3D scan in DTX Studio Clinic.
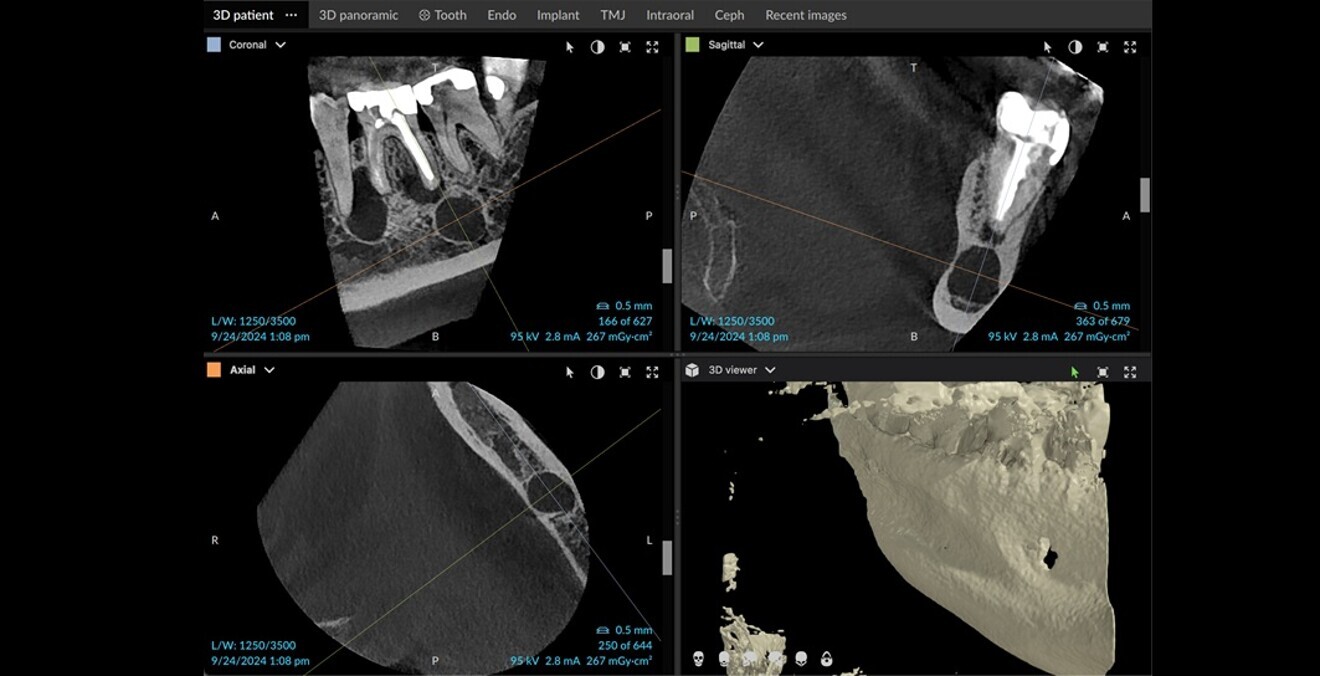
Figs. 4a–d: After adjusting the axial view according to the roots, the extent of the lesions and the separation between the lesions could be seen clearly.



