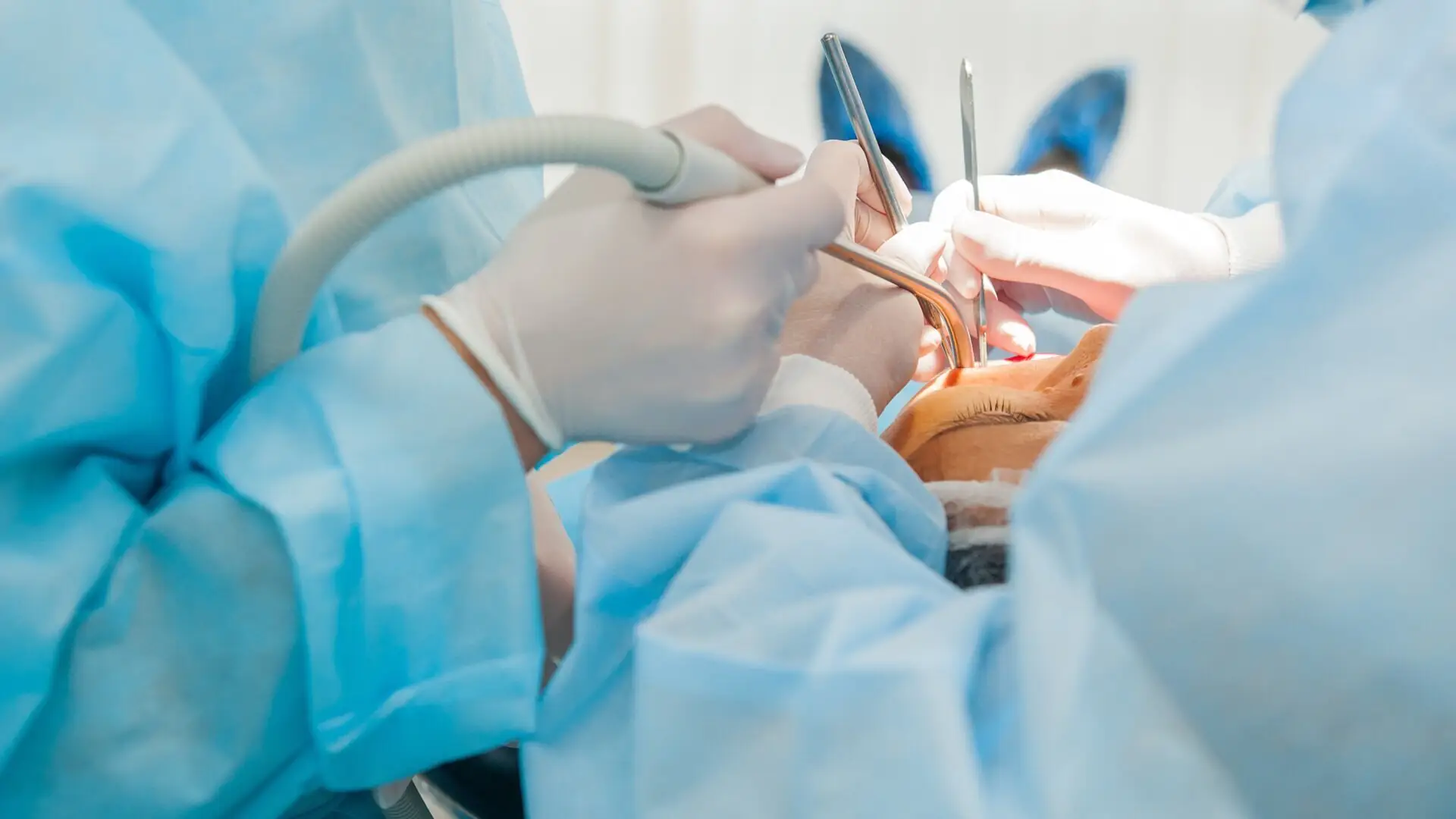
The digital revolution in dentistry has introduced increasingly efficient and predictable workflows, enabling clinicians to drastically reduce treatment times while maintaining high standards of precision and functionality. In particular, the combination of guided surgery and chairside prosthetic manufacturing technologies is reshaping the approach to single-tooth implant restorations.
3D-printing technologies (additive methods) are now emerging as viable alternatives to subtractive methods (e.g. milling), particularly in scenarios where time efficiency and in-office production are critical. Resin-based additive manufacturing systems such as the Dfab tilting stereolithography (TSLA) laser printer with Photoshade technology enable clinicians to produce aesthetic and functional restorations directly in the dental office with unprecedented speed and accuracy.
Screw-retained implant restorations are a widely accepted option owing to their retrievability, lack of cement-related complications and simplified maintenance. Their use in single-tooth cases, when combined with a fully digital workflow, offers the potential for same-day prosthesis delivery, improving patient comfort and reducing the number of clinical appointments.
This report presents the case of a patient with a single edentulous site in the mandibular posterior region. A fully digital chairside workflow was employed, including prosthetically guided planning, guided implant placement and immediate fabrication of a screw-retained crown using a 3D-printing resin. The definitive prosthesis was delivered in a single visit.
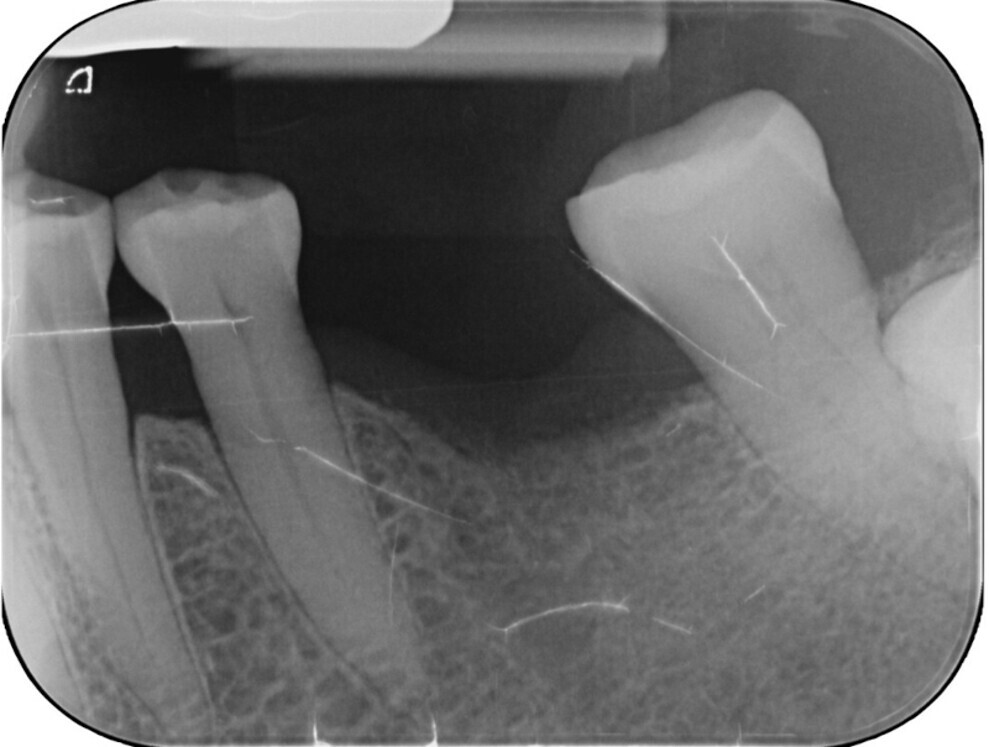
Fig. 1: Radiograph of the single edentulous site in the region of tooth #36 requiring restoration.
Case report
Patient assessment and initial situation
A 62-year-old female patient presented with a single edentulous site in the mandibular left first molar region (tooth #36; Fig. 1). The missing tooth had been extracted six months previously owing to a vertical root fracture. The patient was in good general health and expressed a desire for rapid and minimally invasive implant-supported rehabilitation. Clinical and radiographic evaluation confirmed sufficient bone volume and soft tissue to allow placement of a standard diameter implant without requiring regenerative procedures.
Digital planning and preoperative prosthesis fabrication
A digital workflow was started with the acquisition of intra-oral scans of the maxillary and mandibular arches using the ViSIOScan WL wireless scanner (Cefla; Fig. 2). The STL files were aligned with the CBCT data in RealGUIDE software (3DIEMME), which allowed prosthetically guided planning of the implant position (Fig. 3).
Based on the virtual implant position, a screw-retained crown was fully designed and fabricated prior to surgery without the need for an intra-oral scan after implant placement. The aim was to transfer the prosthetic plan to the surgical phase by ensuring perfect congruence between the digitally planned and clinically executed implant positions.
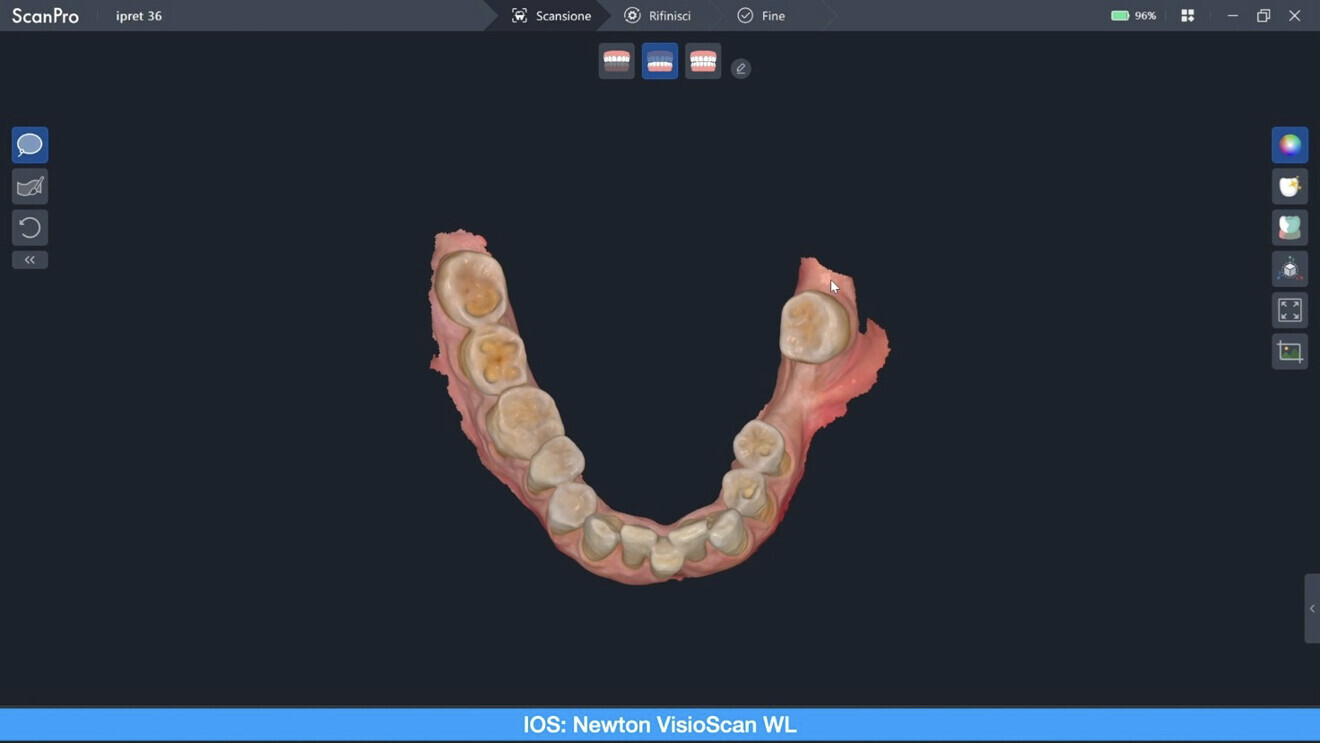
Fig. 2: Intra-oral scan of the mandibular arch.
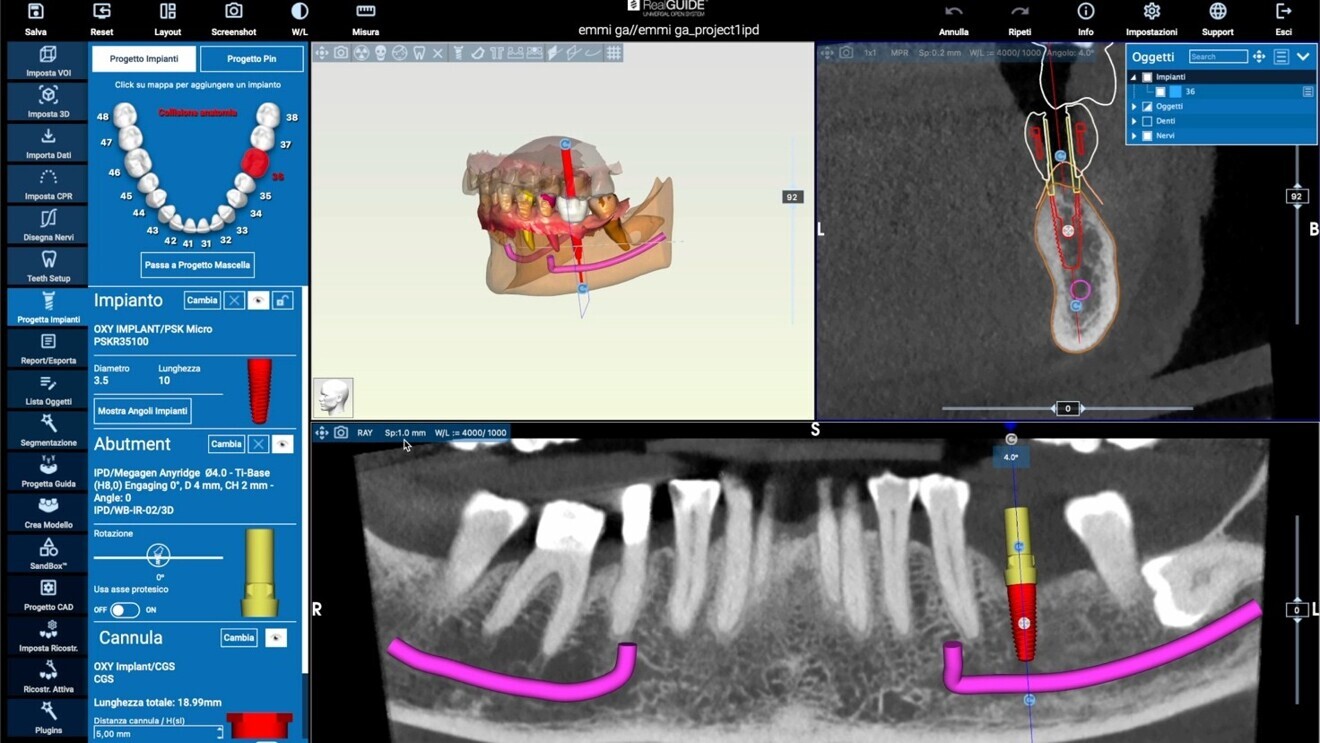
Fig. 3: RealGUIDE software showing the alignment of the STL files with the CBCT data for prosthetically guided planning of the implant position.
The crown was designed using digital prosthetic libraries (IPD Dental Group) to ensure compatibility with both the Oxy Implant PSK implant system (Biomec) and the selected titanium base (Ti-base). The emergence profile, occlusal morphology and screw access hole were designed to fit precisely on the Ti-base, assuming strict adherence to guided placement (Fig. 4).
The final design was then printed in-house using the Dfab TSLA printer with Photoshade technology (RD-Printing; Fig. 5), which allowed for high-resolution reproduction with aesthetic colour gradation. The printing time was 22 minutes, and post-processing included ultraviolet (UV) and heat photopolymerisation, finishing and cementation to the Ti-base.
Guided surgery and prosthesis delivery
A stereolithographic surgical guide generated from the RealGUIDE planning was used to perform fully guided implant placement under local anaesthesia. A PSK implant was inserted at the site of tooth #36 to a final torque of 50 N cm, confirming sufficient primary stability for immediate restoration.
A straight Ti-base was placed according to the angulation designed in the prosthetic plan. The prefabricated screw-retained crown was seated immediately after implant placement without the need for modification or intra-oral scanning. Clinical verification confirmed excellent marginal adaptation and passive fit, both visually and radiographically. Minimal occlusal adjustment was required, and the crown was permanently screwed in place. The screw access hole was sealed with PTFE and composite resin. The patient was discharged with full function and aesthetics restored in the same session.
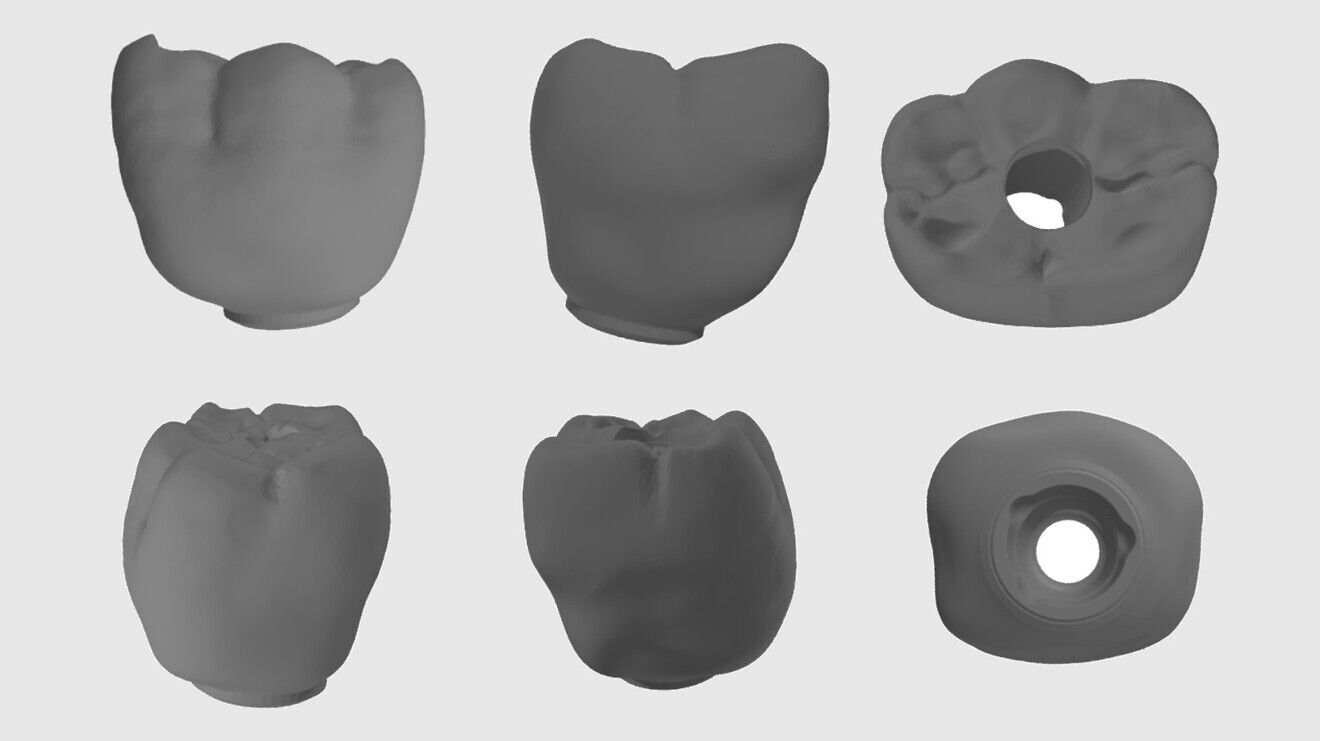
Fig. 4: 3D CAD in STL format.