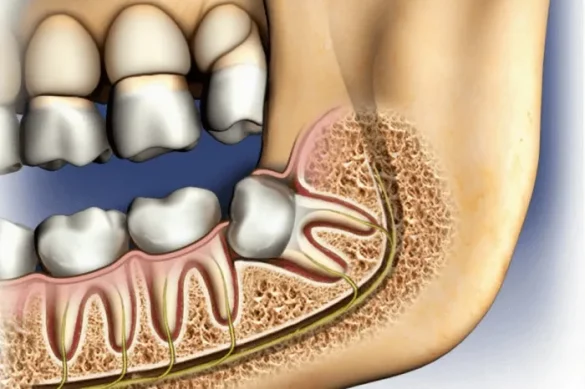
Wisdom teeth removal has long been regarded as a preventive dental procedure. Dentists previously recommended that most, if not all, wisdom teeth be removed in young adults, often before they caused any problems. Today, this long-standing practice is increasingly questioned. New research challenges the necessity of routine extraction, raising critical questions about the potential downsides, risks, and whether keeping wisdom teeth might sometimes be the better option.
Understanding Wisdom Teeth and Their Removal
Wisdom teeth, or third molars, are the last set of molars at the back of a person’s mouth. They usually emerge during the late teens or early twenties. For some people, these teeth grow in without any issues and become functional parts of their mouth. For others, wisdom teeth can cause pain, infection, damage to adjacent teeth, or alignment problems. Traditionally, dentists have removed wisdom teeth as a preventive measure against these possible complications.
Why Routine Removal Was Standard Practice
In the past, it was common for dentists to advise wisdom teeth removal for most patients. The main reasons included preventing future crowding, impaction, misalignment, or cavities because wisdom teeth are hard to clean. The concern was that, even in the absence of symptoms, these teeth would eventually cause problems. Early removal became almost automatic, especially in teenagers and young adults, justified by the idea that younger patients heal faster and face fewer complications.
Evolving Dental Guidelines: A Shift Away From Routine Extraction
Recent advancements in dental research suggest that not all wisdom teeth need to be removed. Dentists and oral surgeons are moving toward a more individualized approach. They now recommend monitoring, rather than removing, wisdom teeth that are healthy, fully erupted, and properly aligned. This shift is supported by evidence-based dentistry—a focus on using the latest studies and scientific data to guide clinical decisions.
Risks and Downsides of Removing Wisdom Teeth
Oral Surgery Risks
Wisdom teeth extraction is a minor surgery, but it still carries risks. The procedure requires anesthesia (either local or general) and may involve incisions in the gum and even bone removal. Common downsides include:
- Infection: Like all surgical procedures, there is a risk of infection at the extraction site.
- Dry socket: This is a painful condition where the blood clot at the surgery site is lost, exposing bone and nerves.
- Delayed healing: Some patients heal slowly, especially if they smoke or have medical conditions affecting recovery.
- Bleeding: Post-operative bleeding can occur, though it is usually manageable.
Pain and Swelling
After wisdom teeth removal, patients commonly experience pain, swelling, and discomfort. These symptoms may last several days and usually require pain management using over-the-counter medications like ibuprofen and acetaminophen. Swelling can occur in the cheeks and jaw, occasionally limiting normal daily activity during recovery.
Other Complications
Some less common complications include:
- Nerve injury: Particularly with lower wisdom teeth, there is a small risk of nerve damage, which may cause tingling or numbness in the lips, tongue, or chin. This can be temporary or, in rare cases, permanent.
- Sinus problems: Removal of upper wisdom teeth located close to sinus cavities may lead to sinus issues, such as pain or small openings between the mouth and sinus.
- Jaw stiffness: In some cases, jaw movement can be limited following surgery, though this generally improves over time.
Are There Long-Term Downsides to Extraction?
Beyond the immediate surgical risks, there may also be long-term effects associated with wisdom teeth removal. Some possible downsides to consider include:
- Loss of natural teeth: Each tooth plays a role in chewing and the stability of the dental arch. Removing wisdom teeth that are otherwise healthy can affect the overall structure of your bite.
- Bone loss: Extracting teeth removes the root from the jawbone, which can, over time, lead to slight bone thinning where the tooth once was.
- Tilting of adjacent teeth: In some instances, removing a tooth can cause the neighboring teeth to shift toward the empty space, potentially affecting alignment.
When Is Wisdom Teeth Removal Necessary?
Dentists still recommend removing wisdom teeth if there are clear problems, such as:
- Infection or gum disease associated with the tooth
- Tooth decay not treatable by filling or other dental work
- Impacted teeth trapped in the jawbone or gums
- Cysts or tumors associated with tooth development
- Damage to neighboring teeth
If you or your dentist observe pain, swelling, frequent infections, or obvious misalignment caused by a wisdom tooth, extraction may be the best option. However, if the teeth are healthy, not causing problems, and can be easily cleaned, they may not need to be removed.
Monitoring and Individualized Care
The trend in modern dentistry is to adopt a personalized approach for wisdom teeth. Dentists use X-rays and regular exams to track changes in wisdom teeth, only recommending removal if they see specific risks or symptoms. Individual factors, such as jaw size, tooth position, and risk of future problems, all play a role in decision-making. This method helps avoid unnecessary surgical interventions and reduces the potential downsides linked to extraction.
Recovery and Managing Pain After Surgery
When wisdom teeth are removed, proper aftercare is essential to reduce the risk of complications. Dentists usually instruct patients to keep the area clean, avoid vigorous rinsing, and eat soft foods during the early stages of recovery. Pain is managed with common pain relievers—ibuprofen and acetaminophen are frequently recommended. It is important not to exceed the advised dosage and to consult your dentist if severe pain, swelling, or bleeding occurs.
Conclusion
In the past, wisdom teeth removal was almost routine, but dental professionals now encourage a more thoughtful and personalized approach. The downsides of unnecessary removal include surgical risks such as infection, nerve injury, and delayed healing; possible long-term effects like bone loss and shifting teeth; as well as the loss of healthy, functional teeth. People should consult with their dentist to discuss whether extraction is necessary for their unique situation. By focusing on individualized care, patients can maintain oral health while minimizing the potential risks associated with unnecessary surgery.
FAQs
1. Is wisdom teeth removal always necessary?
No, not all wisdom teeth need to be removed. Extraction is recommended if the teeth cause pain, infection, damage, or cannot erupt properly.
2. What are the risks involved in removing wisdom teeth?
Removal can lead to swelling, pain, infection, dry socket, nerve injury, and delayed healing.
3. Can keeping wisdom teeth benefit oral health?
If properly aligned and healthy, wisdom teeth can contribute to chewing efficiency and help maintain jaw structure.
4. How does my dentist decide if removal is needed?
Dentists assess each case individually, considering symptoms, tooth position, jaw size, and future risks based on exams and X-rays.