A root canal is a common dental procedure often needed when the inner pulp of a tooth becomes infected or inflamed. Many people worry about the costs involved and wonder whether dental insurance can help pay for root canal treatment. Knowing how to claim insurance for a root canal and what is usually included in coverage is important for making informed decisions and reducing financial stress.
What Is a Root Canal?
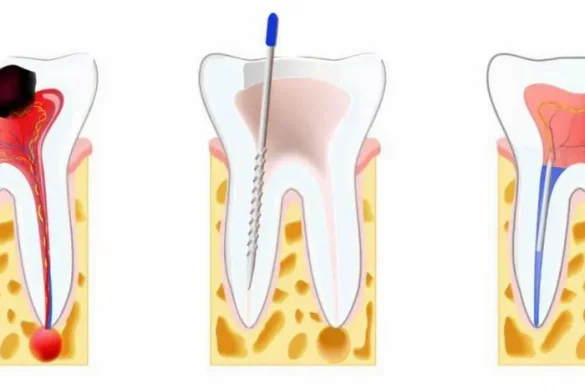
A root canal treatment removes infected or damaged pulp from inside a tooth. This prevents the spread of infection, relieves pain, and saves the tooth from extraction. The process involves cleaning out the inside of the tooth, disinfecting it, and then filling and sealing the space. Sometimes, a crown is placed on the treated tooth for additional protection and strength.
Root canals are typically recommended when there is deep decay, cracks, repeated dental procedures, or trauma to the tooth. Without this treatment, infection can worsen and even result in tooth loss or other serious health issues.
Does Dental Insurance Cover Root Canal Treatment?
Most dental insurance plans do cover root canal treatment, but the extent of that coverage can vary considerably. Dental insurance policies usually categorize procedures into three groups: preventive, basic, and major. Root canal therapy is generally considered a basic or major procedure, depending on the insurance provider. Coverage levels are often set at a percentage of the treatment cost—typically ranging from 50% to 80% for root canal work.
For example, if your root canal costs $1,200 and your plan covers 80%, you are responsible for the remaining 20% (or $240), plus any deductible and co-payment.
The Importance of Insurance Networks
A key aspect of your dental insurance is whether your dentist or endodontist is in-network or out-of-network. An in-network provider has negotiated specific fee reductions with the insurance company, which usually translates to higher coverage and lower out-of-pocket costs for you.
Out-of-network providers may still file claims with your insurer, but you might face higher costs and lower reimbursement rates. Always check your plan’s provider network before starting treatment to maximize savings and avoid surprises at billing.
Factors Affecting Root Canal Coverage
Your ability to claim insurance for a root canal depends on several details in your plan:
Type of Insurance Plan
Most people have either a Preferred Provider Organization (PPO) or a Health Maintenance Organization (HMO) plan. PPO plans offer more flexibility in choosing your dentist and usually provide higher coverage for major procedures, especially with an in-network provider. HMOs often have lower premiums but may limit your choice of providers and require referrals or pre-authorization for certain treatments.
Annual Maximums
Dental insurance plans set a yearly maximum payout for dental services. If the cost of your root canal treatment pushes you over this annual limit, you may have to pay the remaining costs out of pocket. It’s important to know your policy’s maximum limit before committing to treatment.
Deductibles and Co-pays
Most plans require you to pay a deductible before coverage begins. After you meet this deductible, you may have to pay a set percentage of the treatment (co-insurance) or a fixed amount (co-pay), while the insurer pays the rest.
Waiting Periods
Some dental insurance policies have waiting periods before certain services, such as root canals, are covered—especially if you recently enrolled. These can range from six months to one year. Check your plan documents or call your insurer to clarify if a waiting period applies.
Pre-authorization Requirements
Certain insurance plans need pre-authorization for expensive procedures like root canals. This means your dentist must get approval from the insurer before starting treatment. If you skip this step, your claim may be denied or result in reduced reimbursement.
How to Claim Insurance for a Root Canal
The process to claim insurance for your root canal usually involves these steps:
Step 1: Confirm Coverage
Review your dental policy to verify whether root canal treatment is included and what percentage is covered. You can contact your insurance provider or ask your dental office for help in understanding your benefits.
Step 2: Choose the Right Provider
Make sure your dentist or endodontist participates in your insurance network, if possible. This will maximize your coverage and reduce your out-of-pocket expenses.
Step 3: Pre-Treatment Estimate
Ask your dentist to send a pre-treatment estimate, sometimes called a pre-authorization or pre-determination, to your insurer. This will clarify what your insurance will pay and your expected costs before you commit to the procedure.
Step 4: Complete the Procedure
Once you know your coverage, proceed with treatment. Most dental offices will bill the insurance company directly on your behalf, but always check whether you need to pay any portion upfront.
Step 5: File a Claim
If your dental office doesn’t handle the paperwork for you, collect the necessary documents (invoice, description of procedures, dental records, and insurance claim form) and submit them to your insurer. Be sure to follow up to ensure the claim is processed and paid promptly.
Limitations and Exclusions in Dental Policies
Every insurance plan includes some exclusions and limitations. These may include:
- Caps on the amount the plan will pay annually.
- Waiting periods after enrolling before certain treatments are covered.
- Specific exclusions for pre-existing conditions or repeat procedures.
- Restrictions on frequency (e.g., a root canal on the same tooth may not be covered twice in one year).
It’s crucial to read your policy documents carefully and consult your insurer or dental office if you are unsure about your coverage.
What if Your Claim Is Denied?
In some cases, root canal insurance claims are denied or only partially paid. Reasons for denial might include incomplete paperwork, missing pre-authorization, or surpassing annual limits. Always review the denial letter and contact your dental office or insurer for clarification. You can usually appeal a denial by providing extra documentation or clarifying the necessity of treatment.
Financing Options if You Lack Coverage
If you do not have dental insurance, or your policy doesn’t cover most of your root canal cost, many dental providers offer financing plans. Some offices provide payment plans, or you might qualify for third-party financing solutions. Always discuss these options with your dentist to find an affordable arrangement.
Conclusion
You can usually claim dental insurance for root canal treatment, but the amount covered depends on your policy details, provider network, and a range of other factors. To increase your chances of a smooth claim process and lower costs, confirm your insurance coverage in advance, choose an in-network provider, and understand your financial responsibilities. Always read your policy documents and check with your insurance and dental office if you have questions. Managing your dental health proactively can save both your teeth and your wallet.
Frequently Asked Questions (FAQs)
Does dental insurance always cover a root canal?
Dental insurance often covers root canal treatment, but the level of coverage and out-of-pocket costs depend on your plan details and network status.
How much of the root canal cost does insurance pay?
Most plans pay from 50% to 80% of the cost, subject to deductibles, annual maximums, and other policy limits.
What should I do if my insurance claim for a root canal is denied?
Check the reason for denial, provide any missing information, and file an appeal if justified. Your dental office can help resubmit claims.
Are root canals considered major dental work?
Depending on the plan, root canals can be categorized as basic or major dental procedures. Coverage usually differs by category.
Can I get a root canal without dental insurance?
Yes, you can pay out-of-pocket or seek financing options through your dental office or a third-party lender if you lack insurance coverage.